CABG leads to fewer MIs and repeat revascularization vs. stenting
[tabs tab1=”2MM Rundown” tab2= “2MM Full Report”]
[tab]
Image: PD
1. Rates of myocardial infarction, repeat vascularization and a composite of major adverse cardiac and cerebrovascular events were all significantly decreased with coronary artery bypass graft surgery (CABG) compared to percutaneous coronary intervention at 5 years follow-up.
2. Rates of all-cause mortality and stroke did not differ significantly between the two interventions.
3. The SYNTAX score of coronary artery disease complexity can be used clinically to choose the appropriate intervention for patients with atherosclerotic heart disease.
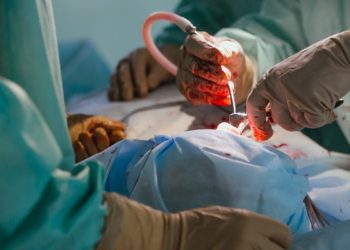
CABG leads to superior intermediate outcomes such as lower rates of heart attack and need for repeat intervention compared to PCI, but does not improve mortality or lower the risk of stroke more than stenting. This study is limited by its inclusion of patients with stable angina who have been previously shown to have unchanged outcomes with optimal medical therapy compared to intervention. An important strength of this study is the creation of the SYNTAX score. This is a practical tool that can be used by providers to make more informed decisions about the most appropriate intervention for their patients with coronary artery disease.
Click to read the study in The Lancet
Click to read the accompanying article “Development and validation of SYNTAX score II”
Click to read the accompanying comment in The Lancet
[/tab]
[tab]
Image: PD
1. Rates of myocardial infarction, repeat vascularization and a composite of major adverse cardiac and cerebrovascular events were all significantly decreased with coronary artery bypass graft surgery (CABG) compared to percutaneous coronary intervention at 5 years follow-up.
2. Rates of all-cause mortality and stroke did not differ significantly between the two interventions.
3. The SYNTAX score of coronary artery disease complexity can be used clinically to choose the appropriate intervention for patients with atherosclerotic heart disease.
This [prospective, randomized] study enrolled 1,800 patients to receive either CABG (coronary artery bypass graft surgery) or PCI (percutaneous coronary intervention) in multiple centers across Europe and United States. Prior to randomization, patients were screened for de-novo three-vessel disease and/or left main coronary disease by both an interventional cardiologist and a heart surgeon. Patients with stable angina were not excluded by the study criteria. The primary outcome of this trial was a composite endpoint defined as the rate of all-cause mortality, stroke, MI and repeat revascularization (major adverse cardiac and cerebral events, or MACCE) at one year, while secondary outcomes included the above vascular complications and death individually at different lengths of time. After 5 years of follow-up, rates of MACCE (26.9% after CABG vs. 37.3% after PCI), estimates of MI (3.8% vs. 9.7%) and repeat vascularization (13.7% vs. 25.9%) were significantly decreased with CABG compared to PCI. Similar to previous studies, rates of death and stroke were did not differ significantly. This study also created a new score of disease complexity (SYNTAX score), and demonstrated that patients with intermediate or high SYNTAX scores had significantly higher rates of MACCE with PCI compared to CABG.
In sum: CABG leads to superior intermediate outcomes such as lower rates of heart attack and need for repeat intervention compared to PCI, but does not improve mortality or lower the risk of stroke more than stenting. This study is limited by its inclusion of patients with stable angina who have been previously shown to have unchanged outcomes with optimal medical therapy compared to intervention. An important strength of this study is the creation of the SYNTAX score. This is a practical tool that can be used by providers to make more informed decisions about the most appropriate intervention for their patients with coronary artery disease.
Click to read the study in The Lancet
Click to read the accompanying article “Development and validation of SYNTAX score II”
Click to read the accompanying comment in The Lancet
By Asya Ofshteyn and Allen Ho
More from this author: Post-operative PTSD intervention improves physical outcomes in trauma patients, Survival improved with lower transfusion threshold in acute upper intestinal bleeds, Single-port appendectomy shows similar outcomes to conventional laparoscopy
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.
[/tab]
[/tabs]