Carbapenem resistance in Enterobacteriaceae nearly quadrupled in the last decade, new study finds
[tabs tab1=”2MM Rundown” tab2= “2MM Full Report”]
[tab]
Image: PD
1. Carbapenem resistance in Enterobacteriaceae increased from 1.2% in 2001 to 4.2% in 2011.
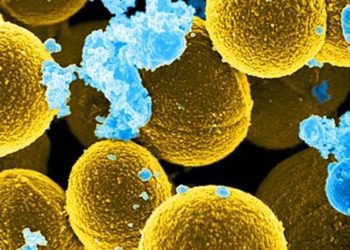
2. Klebsiella had the highest increase in carbapenem resistance.
3. Most CRE infections are acquired in hospitals.
Carbapenem-Resistant Enterobacteriaceae (CRE) have become an increasingly recognized cause of community-acquired and hospital-acquired infections in the United States. Infections associated with CRE yield mortality rates exceeding 40%. The results from this study suggest a disturbingly high increase in the rate of resistance to carbapenem antibiotics among the species of Enterobacteriaceae in the last decade. Between 2001 and 2011, the percentage of Enterobacteriaceae resistant to carbapenems grew by nearly four times, from 1.2% to 4.2%. It also appears as though most of the infections were hospital acquired, either from urinary catheters or intravenous catheters and central lines. While the study was certainly not all inclusive, it spanned several databases and covered multiple sites around the United States to give a reasonable glimpse at the epidemiology of these pathogens. Given the increasing rate of CRE, further attention will need to be directed toward proper utilization of beta-lactams against Enterobacteriaceae, as well as minimizing hospital-acquired infections, and the development of new antimicrobials.
Click to read the study in MMWR
[/tab]
[tab]
Image: PD
1. Carbapenem resistance in Enterobacteriaceae increased from 1.2% in 2001 to 4.2% in 2011.
2. Klebsiella had the highest increase in carbapenem resistance.
3. Most CRE infections are acquired in hospitals.
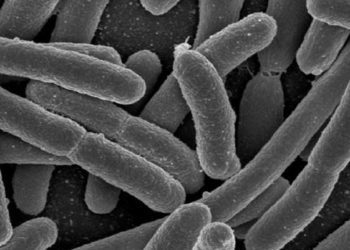
This [restrospective] study investigated the national incidence of Carbapenem-Resistant Enterobacteriaceae (CRE) between 2001 and 2011. The study analyzed data from the National Healthcare Safety Network database, the National Nosocomial Infection Surveillance system and the Surveillance Network-USA to identify cases of hospital-acquired infections involving CRE isolates (E.coli, Klebsiella, and Enterobacter species). Data from the CDC’s Emerging Infections Program were used to corroborate whether identified cases were hospital-associated. According to the study, the proportion of Enterobacteriaceae that were carbapenem-resistant was 1.2% In 2001, and 4.2% in 2011. Klebsiella species yielded the highest increase in carbapenem resistance, from 1.6% to 10.4%. The most common sites of infection were the urinary tract (89%) and blood (10%). 72% of patients with positive CRE cultures had been recently hospitalized.
In sum: Carbapenem-Resistant Enterobacteriaceae (CRE) have become an increasingly recognized cause of community-acquired and hospital-acquired infections in the United States. Infections associated with CRE yield mortality rates exceeding 40%. The results from this study suggest a disturbingly high increase in the rate of resistance to carbapenem antibiotics among the species of Enterobacteriaceae in the last decade. Between 2001 and 2011, the percentage of Enterobacteriaceae resistant to carbapenems grew by nearly four times, from 1.2% to 4.2%. It also appears as though most of the infections were hospital acquired, either from urinary catheters or intravenous catheters and central lines. While the study was certainly not all inclusive, it spanned several databases and covered multiple sites around the United States to give a reasonable glimpse at the epidemiology of these pathogens. Given the increasing rate of CRE, further attention will need to be directed toward proper utilization of beta-lactams against Enterobacteriaceae, as well as minimizing hospital-acquired infections, and the development of new antimicrobials.
Click to read the study in MMWR
By Akira Shisido and Mitalee Patil
More from this author: Pneumocystis linked to sudden infant deaths, Continuous infusion of beta-lactams may be superior to bolus therapy, Novel antiviral drug reduces influenza viral load, Three months of antibiotics appear to effectively treat early-onset spinal implant infections, [Physician Comment] Recurrent early Lyme disease is caused by reinfection, not relapse, Hospital Acquired MRSA pays no attention to vancomycin effectiveness, Oseltamivir treats avian flu early, Linezolid treats Chronic Extensively Drug-Resistant TB but has a high incidence of adverse effects, Intermittent and continuous antiretroviral therapies are equivalent in the treatment of acute HIV-1 infection, Peginesatide is noninferior to epoetin for anemia in hemodialysis patients [EMERALD Trials], Antibiotics improve outcomes in severe acute malnutrition
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain
[/tab]
[/tabs]


![Childhood ADHD associated with increased risk of suicide [Physician Comment]](https://www.2minutemedicine.com/wp-content/uploads/2013/03/PET-image1-e1377449984183-75x75.jpg)


