Contemporary trends and outcomes of liver transplants for alcohol-associated liver disease
1. In this study of short and long-term outcomes of liver transplants in the United States, the proportion of transplants performed for alcohol-associated liver disease increased from 2002 to 2016.
2. The long-term post-transplant survival was lower for patients with transplants performed for alcohol-associated liver disease compared to other indications.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Liver transplantation is the only curative option for end-stage liver disease. Recently, alcohol-associated liver disease (ALD) has emerged as the most common reason for liver transplant. The increase in proportions of transplants for ALD may reflect the decreased need of transplant for hepatitis C viral infections, and also the increased use of transplant for alcoholic hepatitis without a mandatory six-month abstinence requirement following positive results from a 2011 clinical trial. The current study sought to further evaluate trends in use of liver transplant in the United States and evaluate short- and long-term clinical outcomes for those with ALD. The study found that the proportion of transplants performed for ALD doubled from 2002 to 2016. Patients with transplants for ALD had similar 5-year survival but slightly worse 10-year survival compared to those transplanted for non-ALD indications.
The main strength of this study was the large, prospectively collected cohort of transplant patients that allowed analysis of 10 year outcomes. The main limitation of the study included the reliance on registry data which precludes establishing casual links and only allows associations to be determined. Further studies will be needed to evaluate the causality between changing attitudes and values and the decision to pursue transplant.
Click to read the study in JAMA Internal Medicine
Relevant Reading: Early Liver Transplantation for Severe Alcoholic Hepatitis in the United States—A Single‐Center Experience
In-Depth [prospective cohort]: This study was a multi-center, prospective, national cohort study using data from the United Network for Organ Sharing registry that included liver transplant patients from 2002-2016. Patients were excluded if they were younger than 18 years old, had HIV infection, had acute hepatic failure, model for end-stage liver disease (MELD) score exception criteria, or previous liver transplant.
The study included 32,913 patients, of whom 9438 had liver transplants performed for ALD. The proportion of liver transplants for ALD increased from 15.3% in 2002 to 30.6% in 2016. After the exclusion of transplants related to hepatitis C this proportion increased from 24.2% in 2002 to 36.7% in 2016. Cumulative 5-year survival was not different between those with ALD or non-ALD related transplants (79% vs. 80%); but 10-year cumulative post-transplant survival was lower for those with ALD (63% vs. 68%, P=0.006).
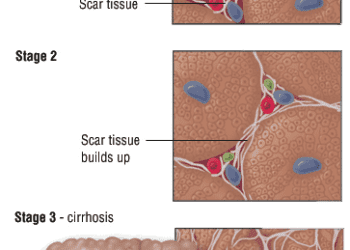
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.