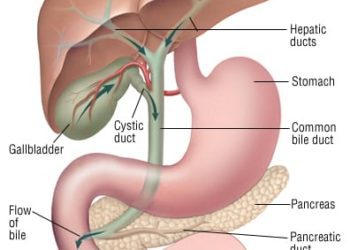
Futibatinib for FGFR2 Mutated Intrahepatic Cholangiocarcinoma
1. Using futibatinib to treat patients with FGFR mutated intrahepatic cholangiocarcinoma resulted in a 42% objective response rate (partial or complete), with no differences in the effectiveness of treatment across various FGFR2 fusions or mutations.
2. Most common grade 3 or higher treatment-related adverse events included hyperphosphatemia (30%), elevated AST levels (7%), stomatitis (6%), and fatigue (6%).
Evidence Rating Level: 2 (Good)
Study Rundown: Fibroblast growth factor receptor 2 (FGFR2) fusions/rearrangements can occur in up to 14% of patients with intrahepatic cholangiocarcinoma. This paper investigates futibatinib, an FGFR1-4 inhibitor which irreversibly binds to the FGFR kinase, for patients with confirmed FGFR mutated intrahepatic cholangiocarcinoma who failed a previous line of systemic therapy in the advanced stage setting. The primary endpoint was objective response rate (ORR) and secondary endpoints included duration of response (DoR), disease control, progression-free survival (PFS), overall survival (OS), safety, and quality of life. This study found that ORR was 42%, median DoR was 9.7 months, and 83% of patients had some disease control. The median PFS was 9.0 months and the median OS was 21.7 months. There were no differences in the effectiveness of treatment across various FGFR2 fusions or mutations. The most common grade 3 or higher treatment-related adverse events included hyperphosphatemia (30%), elevated AST levels (7%), stomatitis (6%), and fatigue (6%). Quality of life was preserved throughout the study. The strengths of this study included the length of follow-up time as well as its detailed genomic profiling analysis. The limitations of this study included the number of patients and the single-arm methodology. Overall, this paper found a measurable benefit in using futibatinib to treat patients with FGFR mutated intrahepatic cholangiocarcinoma in this pre-treated population, and further research is warranted.
Click to read the study in NEJM
Relevant Reading: Phase I, first-in-human study of futibatinib, a highly selective, irreversible FGFR1–4 inhibitor in patients with advanced solid tumors
In-Depth [prospective cohort]: This open-label, single-group, multinational phase 2 study recruited 103 patients who had unresectable or metastatic intrahepatic cholangiocarcinoma with an FGFR2 fusion-positive or rearrangement who failed at least 1 line of systemic therapy. The median follow-up was 17.1 months and the median duration of treatment was 9.1 months. The ORR was 42% (95%CI, 32 to 52), with 72% of those having a response that lasted at least 6 months, and 14% having responses lasting at least 12 months. The median DoR was 9.7 months (95%CI 7.6 to 17.0) and 83% of patients (95%CI, 74 to 89) had disease control. For those patients with a response, the median time to respond was 2.5 months. The median PFS was 9.0 months (95%CI, 6.9 to 13.1) and the median OS was 21.7 months (95%CI, 14.5 to not reached). On an extended follow-up, 8 months post the initial analysis, response and survival rates were found to be similar. The study found that the effectiveness of treatment in patients did not depend on the presence of specific FGFR2 fusions or mutations. With regards to safety, the most common grade 3 or higher treatment-related adverse event included hyperphosphatemia (30%), elevated AST levels (7%), stomatitis (6%), and fatigue (6%). These and other adverse events led to dose interruptions in 50% of patients and dose reductions in 54% of patients. Patient-reported outcomes were evaluated through EORTC QLQ-C30 and EQ-5D and throughout treatment scores remained stable or improved in most patients. Overall, this study found some measurable benefits in using futibatinib to treat patients with FGFR mutated intrahepatic cholangiocarcinoma.
Image: PD
©2023 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.