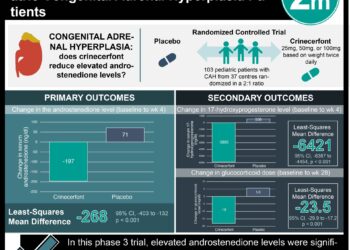
Hypercortisolism of bilateral macronodular adrenal hyperplasia may be corticotropin-dependent
Image: PD
1. Messenger RNA encoding proopiomelanocortin, a corticotropin precursor, was detected in all samples of hyperplastic adrenal tissue.
2. In two patients, corticotropin concentration was higher in the adrenal veins than peripheral veins, suggesting local production.
3. Although bilateral macronodular adrenal hyperplasia has been thought to be corticotropin-independent, these findings suggest that the disease is associated with ectopic corticotropin secretion from the adrenal cortex.
Evidence Rating Level: 4 (Below average)
Study Rundown: “Corticotropin-independent macronodular adrenal hyperplasia” may be a misnomer in light of new findings regarding the pathophysiology of this disease. In this study, Louiset et al. suggest that hypercortisolism in patients with bilateral adrenal macronodular hyperplasia may result from ectopic production of corticotropin in the adrenal cortex. Despite the small sample of 30 patients, the results were convincing with a high degree of consistency among cases. Additionally, the current study found that corticotropin-synthesizing cells co-expressed Leydig- and luteal-cell marker insulin-like 3, which suggests that the these aberrant cells may result from abnormal gonadal-like differentiation or from migration of gonadal stem cells during embryogenesis. Finally, in vitro studies showed that cortisol secretion was reduced with melanocortin 2 receptor antagonists. This may be clinically important as future therapies involving targeted molecular agents may be more effective and less invasive than the current standard therapy – bilateral adrenalectomy.
Click to read the study, published today in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Adrenocortical-pituitary hybrid tumor causing Cushing’s syndrome
In-Depth [case series]: This study investigated the possibility that cortisol secretion in “corticotropin-independent” macronodular adrenal hyperplasia may be driven by local corticotropin production. The study analyzed samples from 30 patients: 13 were collected prospectively at surgery and 17 were analyzed retrospectively with fixed or frozen samples.
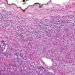
Conventional and RT-PCR tests were positive for proopiomelanocortin mRNA in all 26 samples tested, with values from 4.2 to 62.6 pg of proopiomelanocortin mRNA per 1 ng of cyclophilin mRNA (median, 32.5). Immunohistochemical analysis with anti-corticotropin antibodies were positive in all 25 samples analyzed. The immunoreactive cells were in isolated patterns in 4 of the 25 samples (16%) and in clustered patterns in the other 21 samples (84%). As a negative control, corticotropin immunostaining were all negative in six normal adrenal glands and four cortisol-secreting adenomas.
In two patients, plasma corticotropin levels were measured from the right and left adrenal veins and were found to be higher than those in the peripheral veins (26.6±5.5 and 15.0±2.0 pg/ml in adrenal veins, respectively vs. 2.0±0.5 pg/ml peripherally in patient 12; 54.0±3.6 and 36.0±3.0 pg/ml in adrenal veins, respectively vs. 4.6±1.2 pg/ml in patient 13).
Based on these results, the authors concluded that cortisol secretion by the adrenal glands in bilateral macronodular adrenal hyperplasia may be regulated by local production of corticotropin and thus, may be corticotropin-dependent.
By Xiaozhou Liu and Adrienne Cheung
More from this author: Nivolumab plus ipilimumab shows promise for metastatic melanoma, Prophylactic platelet transfusions prevent bleeding in hematologic cancers, Azithromycin is not associated with increased cardiovascular death in low-risk groups, Health education module reduces parasitic infections, New chemotherapy precludes the need for radiotherapy in primary mediastinal B-cell lymphoma
©2012-2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.