No association found between third trimester maternal NSAID use and newborn pulmonary hypertension
 [tabs tab1=”2MM Rundown” tab2= “Full 2MM Report” tab3=”About the Authors”]
[tabs tab1=”2MM Rundown” tab2= “Full 2MM Report” tab3=”About the Authors”]
[tab]
Image: CC/SageRoss
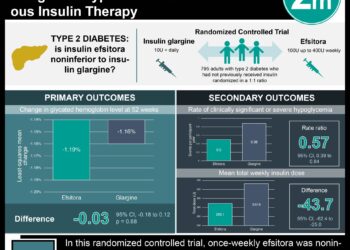
1. Maternal NSAID use in the third trimester is not associated with an increased likelihood of persistent pulmonary hypertension of the newborn (PPHN).
2. Factors found to be associated with increased risk of PPHN included birth by cesarean delivery, gestational age <37 weeks or > 41 weeks, and large for gestational age designation.
These data suggest that despite biological plausibility and some case reports, there is no evidence to support the theory that NSAID consumption during pregnancy increases the risk of PPHN. This study is limited in that it relies on maternal recall for data collection and information about exposure status, and recall bias may contribute to lower estimates of NSAID use during the third trimester.
Click to read the study in Pediatrics
[/tab]
[tab]
Primer: PPHN is a clinical syndrome characterized by hypoxic respiratory failure caused by persistently elevated pulmonary vascular resistance during the postnatal period that prohibits adequate pulmonary blood flow. Patients that develop PPHN are typically term or late preterm (>34 weeks) infants with no other associated congenital anomalies. This increased resistance may be related to underdevelopment of pulmonary vasculature, with reduced cross-sectional area, or to maldevelopment of the pulmonary vasculature, with poor responsiveness to stimuli that would otherwise decrease PVR and promote a smooth transition from fetal to neonatal circulation. Cesarean section, non-vertex position, meconium aspiration syndrome, and post-dates delivery have all been epidemiologically associated with PPHN, as has the maternal use of NSAIDs (aspirin, ibuprofen, etc.) during the third trimester. Fetal NSAID exposure has been theorized to increase the risk of PPHN by increasing pulmonary perfusion in utero with premature closure or spasm of the ductus arteriosus, which thickens the pulmonary vasculature. This study seeks to test the hypothesis that prenatal NSAID exposure predisposes to PPHN using a case-control design.
Background reading:
1. Up To Date: Persistent Pulmonary Hypertension of the Newborn
This [case-control] study: identified 377 infants with PPHN and 836 control cases without PPHN, matched by hospital and birth dates. Mothers were interviewed within 6 months of delivery. The study evaluated two central hypotheses: 1.) that maternal consumption of NSAIDs, but not acetaminophen, is associated with PPHN, and 2.) that the association between NSAID use and PPHN is greatest when the NSAID use occurred during the third trimester.
Third trimester exposure to NSAIDS was not found to be associated with the development of PPHN. The risk for developing PPHN was slightly higher among infants born to mothers with third trimester aspirin use (OR = 1.82), though this did not reach significance. Ibuprofen and acetaminophen were also not found to be associated with the development of PPHN with odds ratios of 0.65 and 0.8, respectively, and confidence intervals including the null.
Increased risk for the development of PPHN was associated with other factors, including birth by cesarean delivery, gestational age < 37 weeks or > 41 weeks, and large for gestational age designation.
In sum: These data suggest that despite biological plausibility and some case reports, there is no evidence to support the theory that NSAID consumption during pregnancy increases the risk of PPHN. This study is limited in that it relies on maternal recall for data collection and information about exposure status, and recall bias may contribute to lower estimates of NSAID use during the third trimester.
Click to read the study in Pediatrics
By [EH] and [DB]
© 2012 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.
[/tab]
[tab]
 Emilia Hermann: Emilia is a 3rd year MD candidate at the University of Pennsylvania. She grew up in Atlanta, Georgia and graduated from the University of Pennsylvania in 2009 with a degree in Anthropology. Her medical interests include pediatrics, infectious disease, and global health. She loves to travel and, when not studying or running around the hospital, can be found planning her next big adventure.
Emilia Hermann: Emilia is a 3rd year MD candidate at the University of Pennsylvania. She grew up in Atlanta, Georgia and graduated from the University of Pennsylvania in 2009 with a degree in Anthropology. Her medical interests include pediatrics, infectious disease, and global health. She loves to travel and, when not studying or running around the hospital, can be found planning her next big adventure.
 Devika Bhushan: Devika is a 4th year M.D. candidate at Harvard Medical School. She has grown up between India, the United States, and the Philippines. She attended Columbia University as an undergraduate, majoring in Neuroscience and Behavior. During medical school, she has discovered a passion for pediatric neurology, and is also interested in behavioral health and social determinants. She is responsible for overseeing content in general pediatrics and in pediatric neurology.
Devika Bhushan: Devika is a 4th year M.D. candidate at Harvard Medical School. She has grown up between India, the United States, and the Philippines. She attended Columbia University as an undergraduate, majoring in Neuroscience and Behavior. During medical school, she has discovered a passion for pediatric neurology, and is also interested in behavioral health and social determinants. She is responsible for overseeing content in general pediatrics and in pediatric neurology.
[/tab]
[/tabs]