No difference in bowel obstruction rates following closure of diverting loop ileostomy via either handsewn or stapler techniques: the HASTA trial
Image: CC/J.Heilman
Key study points:
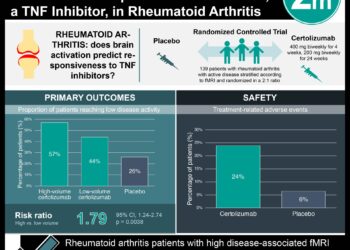
1. No significant difference in 30-day bowel obstruction rates between handsewn and stapler closure of loop ileostomy following lower anterior resection for colorectal cancer.
2. Operative time was significantly decreased by 15 minutes with stapling closure of loop ileostomy.
Primer: Lower anterior resection (LAR) and total mesorectal excision involves removing the proximal two thirds of the rectum is removed with the rectal sphincter preserved is possible, along with removal of the diseased segment of bowel and associated lymph nodes. This is the standard procedure for surgical management of rectal cancer. Usually, a diverting protective stoma is placed until definitive anastomotic healing is achieved, either a loop ileostomy or colostomy. After about 3 months’ time, intestinal continuity is reestablished by closure of the ileo- or colostomy via anastamosis. However, there is still debate as to whether hard-sutured versus stapled anastomosis is a more efficacious technique to reverse a loop ileostomy and to prevent future bowel obstruction and other related complications. Prior studies of this issue were smaller, single-centered trials with heterogeneous patient populations that had conflicting results. The Hand Suture Versus Stapling for Closure of Loop Ileostomy Trial (HASTA Trial) hoped to definitively answer the question of which technique was optimal for closure of loop ileostomies.
Background reading:
1. Weitz J, Koch M, Debus J, et al. Colorectal cancer. Lancet. 2005;365:153–165.
This [multicenter, randomized, controlled ] study: encompassed a total of 327 patients from 27 different centers with rectal cancer randomized closure of loop ileostomy via handsewn or stapled anastamosis following lower anterior resection. There was no statistically significant difference in bowel obstruction rates with either procedure with 10.3% of patients in the stapler arm and 16.6% of patients in the handsewn arm developing bowel obstruction within 30 days (OR = 1.72, 95% CI = .89-3.31). There was also no significant difference in anastamotic leakage rate. Multivariable analysis of risk factors including hand suture, surgical skill, operative time, BMI, age, gender, laparoscopic LAR, extended resection, neoadjuvant therapy, and adjuvant therapy yielded no significant association with bowel obstruction. However, operative time was significantly shower in the stapler group by 15 minutes (P<.001).
In sum: This multicenter, randomized, controlled surgical trial sought to answer the question as to whether there was a preferred technique for closure of diverting loop ileostomy following LAR for colorectal cancer. The study concluded that there was no significant difference in bowel obstruction complications between handsewn and stapler anastomosis techniques. There was also no perceptible difference in anastomotic leakage, although the study was not powered to examine this endpoint specifically. There was a significantly shorter operative time by 15 minutes with the stapler technique, which is important for keeping operative times down. Many hospitals do not utilize stapling anastomosis currently because of cost considerations, and further study needs to be done to see if the cost-savings from shorter operative times justify the increased cost of stapler use. This trial was designed to be generalizable and incorporated institutions from all levels within the health care system, and was adequately powered to detect significant changes in the primary endpoint of 30 day bowel obstruction.
Click to read the study in [Annals of Surgery]
By [AH]
© 2012 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. DISCLAIMER: Posts are not medical advice and are not intended as such. Please see a healthcare professional if you seek medical advice.