Overall survival with triplet therapy in BRAF V600 mutation-positive advanced melanoma
1. OS in triplet combination therapy (atezolizumab, vemurafenib, and cobimetinib) while numerally better, was not statistically improved when compared to treatment with just a BRAF inhibitor and a MEK inhibitor.
2. Grade 3-4 reactions occurred at similar rates between both groups, but there were some differences in the atezolizumab group (more bloodwork abnormalities and reactions).
Evidence Rating Level: 1 (Excellent)
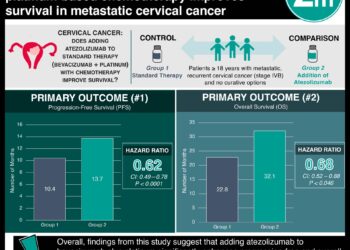
Study Rundown: Triplet combination therapy with immunotherapy, a BRAF inhibitor, and a MEK inhibitor has been thought to provide high response rates and long durability for patients with BRAF-positive metastatic melanoma. A previous study investigated vemurafenib (BRAF inhibitor) and cobimetinib (MEK inhibitor) in combination with either placebo or atezolizumab (PD-L1 inhibitor) in a randomized multicenter phase 3 study and found the triplet therapy showed significant improvement in progression-free survival (PFS) although overall survival (OS) data was immature. This paper reports a second interim analysis of OS based on the results of the first study. The primary outcome was PFS, and the secondary outcomes were OS, objective response rate (ORR), duration of response (DoR), and quality of life. This secondary analysis found that the median OS was 39 months in the atezolizumab group vs 25.8 months in the control group and while OS was similar at 12 months between both groups, the OS rate started to diverge afterwards. PFS was better in the atezolizumab group than in the control group (HR 0·79). ORR was similar across the groups but the median DoR was improved in the atezolizumab group, 21.0 months vs 12.6 months. Grade 3-4 reactions occurred at similar rates between both groups, but there were some differences in atezolizumab group (more bloodwork abnormalities and reactions). The strengths of this study included longer follow-up time. Limitations to this study included a small sample size. Overall, this secondary analysis has shown that the overall survival in patients with BRAF-positive advanced melanoma treated with triplet combination therapy while numerally better, was not statistically improved when compared to treatment with just a BRAF inhibitor and a MEK inhibitor and pending further studies are likely needed to be more confident of the effectiveness of triple therapy.
Click to read the study in Lancet Oncol
In-Depth [ randomized controlled trial]: This randomized double-blind, placebo-controlled, multicenter phase 3 study recruited 514 patients aged 18 years or older who had previously untreated, histologically confirmed stage IV or unresectable stage IIIc melanoma, BRAFV600 mutation-positive, and were ECOG 0 or 1. Patients were randomized (1:1) to atezolizumab, vemurafenib, and cobimetinib (256 patients) or placebo, vemurafenib, and cobimetinib (258 patients). The median follow-up duration was 29.1 months for the atezolizumab group and 22.8 months for the control group. Median OS was 39 months (95% CI, 29.9-not estimable) in the atezolizumab group and 25.8 months (95%CI, 22.0-34.6) in the control group (HR 0.84 [95%CI, 0.66-1.06], p=0.14). OS at 12 months was 76% in both groups and OS at 24 months was 62% (95%CI, 55-68) in the atezolizumab group vs 53% (95%CI, 47-60) in the control group. Investigator-assessed PFS continued to show a benefit in the atezolizumab group over the control group (HR 0·79 [95%CI, 0.64-0.97], p=0.022). ORR was similar across both groups, but median DoR was improved in the atezolizumab group, 21.0 months (95%CI, 16.6-32.2) vs 12.6 months (95%CI, 10.5-16.7) in the control group. Grade 3-4 reactions occurred at similar rates between both groups, but the atezolizumab group had more proportions of CK, ALT, AST, and amylase elevations, as well as maculopapular rash, hypertension, arthralgia, photosensitivity reactions, lymphopenia, acute kidney injuries, and infusion-related reactions.
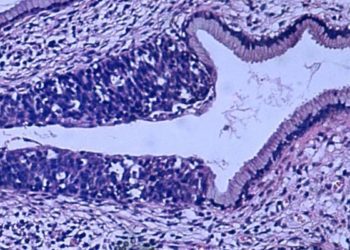
Image: PD
©2022 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.