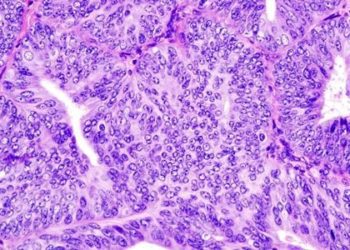
Sentinel lymph node mapping identifies metastases in high-risk endometrial cancer
1. Among women undergoing pelvic and para-aortic lymphadenectomy, 10.6% had metastatic disease to the lymph nodes.
2. The sensitivity and specificity of sentinel lymph node (SLN) histology for metastatic disease confirmed on total lymphadenectomy were 100%.
Evidence Rating Level: 2 (Good)
Study Rundown: Endometrial cancer is the most common gynecologic malignancy in the United States. At the time of diagnosis, most have disease confined to the uterus; a minority has spread to regional organs and lymph nodes, and an even smaller proportion has distant metastases. Current guidelines recommend surgical staging, but there is variation in evaluation of lymph node involvement across providers and institutions. Because prior studies have demonstrated that most women with early stage endometrial cancer have negative pelvic lymph nodes, total lymphadenectomy is not standardly performed. However, sometimes the surgical stage can be underestimated intraoperatively and women who may have lymph node metastases do not receive lymphadenectomy. SLN mapping, which is used in management of breast cancer and melanoma, has been performed in women with endometrial cancer at low risk for nodal involvement. In the present work, the authors studied the use of SLN mapping in women at high risk of nodal involvement.
Results demonstrate a high detection rate with SLN mapping such that in women who met criteria for bilateral pelvic and periaortic lymphadenectomy (PPALAN), 10.6% had lymph node metastases. Strengths included prospective data collection and use of PPALAN to evaluate the test characteristics of SLN mapping in this setting. The study was limited by small sample size, lack of a comparison group and selection bias, since the characteristics of participants who declined were not studied. Randomized trials including a control arm are needed to better understand the role for SLN mapping in high risk cases of endometrial cancer.
Click to read the study in AJOG
Relevant Reading: Prospective assessment of lymphatic dissemination in endometrial cancer: a paradigm shift in surgical staging
In-Depth [prospective cohort]: This study assessed the use of SLN mapping during robotic tumor staging surgery among women with biopsy-proven endometrial cancer (n = 123), including those at high risk for nodal metastasis (n = 85) who underwent planned pelvic and para-aortic (total) lymphadenectomy. The primary outcome of interest was the feasibility of SLN mapping. Secondary outcomes included the sensitivity and specificity of SLN mapping, using total lymphadenectomy as the gold standard.
Bilateral pelvic and para-aortic lymph nodes were mapped in 80% of patients. At least one sentinel lymph node was detected in 97% of participants. Among patients at high risk for nodal metastases who underwent both pelvic and para-aortic lymphadenectomy, 10.6% were found to have lymph node metastases and in 44% of these, the SLN was the only positive node. There were cases in which final SLN pathology was negative but metastatic disease was discovered on completion lymphadenectomy. The sensitivity and specificity of SLN histology for metastatic disease on pelvic and para-aortic lymphadenectomy were both 100%.
Image: CC/Wiki/EdUthman
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.