Significant number of pre-operative diagnostic cardiac catheterizations may be unnecessary
1. In this retrospective descriptive study about patients undergoing cardiac evaluation prior to non-cardiac surgery, about 50% of patients who underwent cardiac catheterization were asymptomatic, and about one-quarter of the cohort that underwent catheterization went on to get revascularized with either percutaneous intervention (PCI) or bypass surgery.
2. This study did not study short-term outcomes after the index surgery, nor did it analyze long-term cardiac outcomes (death, risk of myocardial infarction); however, the results did shed light on potentially non-guideline based practice in regards to cardiac evaluation and revascularization prior to non-cardiac surgeries.
Evidence Rating Level: 3 (Average)
Study Rundown: Although routine cardiac catheterization prior to non-cardiac surgeries is not recommended, patients with certain risk factors are still often referred either for noninvasive cardiac stress testing or directly for cardiac catheterization to evaluate for obstructive coronary artery disease. The patient characteristics, angiographic findings, or clinical outcomes of catheterization are not well studied. This retrospective descriptive analysis aimed to describe these features in clinically stable patients who underwent cardiac catheterization prior to non-cardiac surgery.
Of the study cohort, about one-third of the patients did not undergo a noninvasive stress test prior to cardiac catheterization. About 50% of patients who underwent cardiac catheterization were asymptomatic, and about one-quarter of the cohort that underwent catheterization went on to get revascularized with either percutaneous intervention (PCI) or bypass surgery. One-quarter of patients who were referred for revascularization were asymptomatic. While this study did not evaluate long term outcomes after the index surgical procedure, it did highlight the possible groups of patients who may be receiving over-treatment of their coronary artery disease. However, future studies are necessary to evaluate longer term outcomes in these patients.
Click to read the study, published in JAMA Internal Medicine
Relevant Reading: Risk of major adverse cardiac events following noncardiac surgery in patients with coronary stents
In-Depth [retrospective descriptive]: This retrospective descriptive analysis used the National Cardiac Data Registry from July 2009 to December 2014. Patients who were undergoing non-cardiac surgeries and received a diagnostic catheterization as a part of their preoperative evaluation were included in the cohort. Patients with acute coronary syndrome, cardiogenic shock, cardiac arrest or emergency catheterization were excluded. Baseline demographic characteristics, previous noninvasive cardiac testing, angiographic findings and treatment recommendations were analyzed. Inpatient outcomes for those who underwent PCI were also collected.
Of the 194,444 cohort patients, the majority were Caucasian, male and overweight or obese. Most patients were asymptomatic (117,821; 60.6%). Previous noninvasive cardiac stress testing was done in 65.2% (126,766) of patients, and 86.3% of these previous tests were positive. Bypass surgery or PCI were performed in 46,380 (23.8%) patients. Of these, 27,191 were patients who had been clinically asymptomatic. Revascularization was recommended to 48.3% (45,083) of patients with obstructive disease found on cath, and rarely in patients with nonobstructive coronary disease (1249, 1.3%). The catheterization-related mortality rate was low at 0.05%.
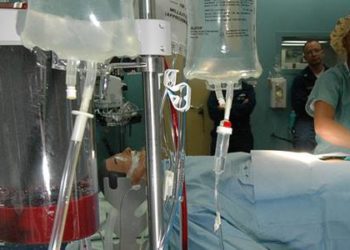
Image: PD
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.