Standardized measures effectively tracked psoriasis and acne outcomes
1. Using the Physician Global Assessment (PGA), patients with acne or psoriasis recorded significant improvement in disease severity at 3-month follow-up.
2. Incorporating the PGA into billing sheets was a feasible method for seamless transition into clinical practice with an observed 100% physician compliance after follow-up.
Evidence Rating Level: 2 (Good)
Study Rundown: Standardized quality measures to track outcomes over time are highly valued, as healthcare moves toward pay-for-performance metrics. Broadly implementing such metrics in dermatology can be challenging because diagnosis and management decisions may be made based on the visual physical examination as opposed to lab results, necessitating novel means of standardization. These authors investigated the utility of the Physician Global Assessment (PGA) by assessing the treatment outcomes of acne and psoriasis. It was found that the PGA scale had good inter-observer agreement and could effectively measure treatment response in both diseases. While the study uniquely aimed to tackle a gap within dermatologic practice using a large cohort and prolonged timeframe, the scale may not be comprehensive as it does not collect data such as scarring vs. non-scarring in patients with acne, which may limit clinical utility. Additionally, selection bias in the psoriasis subset may have been present as 2 of 5 dermatologists had practices primarily consisting of patients with severe disease.
Click to read the study in JAMA Dermatology
Relevant Reading: What dermatology still needs to create meaningful patient outcome measurements
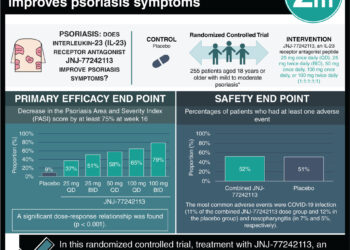
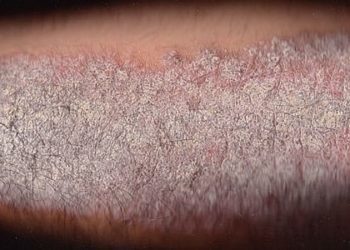
In-Depth [prospective cohort]: The 5-score PGA severity rating (categories: clear, almost clear, mild, moderate, or severe) was incorporated into billing sheets and ultimately 2770 encounters were completed on patients with acne, and 1516 on patients with psoriasis by 30 trained-attending dermatologists. A subset of patients was given the patient global assessments (PtGA), a measure to assess reliability of the PGA within a particular clinic, demonstrating concordant results. Among new patients who subsequently returned for 3-month follow-up evaluation, the majority of patients in the acne or psoriasis subset had moderate-severe disease. Of patients with acne, 14.6% and 22% of patients were graded as clear or almost clear of acne at 3 and 16-month follow-up, respectively. Of patients with psoriasis, 22.3% and 31.5% of patients were graded as clear or almost clear of lesions at 3 and 16-month follow-up, respectively. When acne and psoriasis grades of clear or almost clear at 3-months were compared to baseline (2.1% and 3.1% respectively), both showed significant improvement over time (p<0.001) Interobserver agreement between PGA and PtGA scores was good (acne, κ = 0.68; psoriasis, κ = 0.70).
More from this author: Tech-aided surveillance of patients at high risk for melanoma aids early diagnosis, Indoor tanning linked to high skin cancer risk in US and abroad, Free drug samples may alter prescription habits of dermatologists, Atopic dermatitis may be more persistent than previously understood
Image: PD
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.




![Fluorophores enhance visualization for image-guided surgery [PreClinical]](https://www.2minutemedicine.com/wp-content/uploads/2015/01/FISH_13_21-75x75.jpg)