[Researcher Comment] Structured lifestyle interventions improve both weight and metabolic outcomes in obese children
Image: CC/Lokal_Profil. Kcal/person/day
Study Author, Mandy Ho, MSc, APD, RN, talks to 2 Minute Medicine: The Children’s Hospital at Westmead Clinical School, University of Sydney, Sydney, Australia
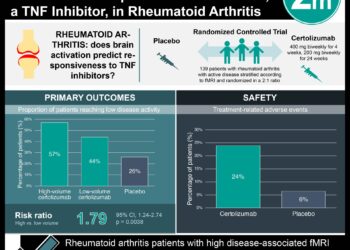
The clinical importance of your study for physicians This [review] provides solid evidence to show that lifestyle interventions are effective in reducing weight and improving cardio-metabolic outcomes across a wide range of treatment settings (including hospital, primary care, community and schools), age groups and severity of obesity. Therefore, lifestyle interventions, involving a multidisciplinary approach, should remain a first line treatment for obese children and adolescents.
The relevance of your study for medical students in training Pediatric obesity is a highly prevalent condition with significant short- and long-term health, social and economic consequences. Yet it is frequently being overlooked in clinical practice.
Medical students in training should equip themselves with the knowledge and skills to identify and monitor obesity and its associated cardio-metabolic risks in children and adolescents. They should also be familiar with using a multidisciplinary approach for delivering lifestyle interventions. Our systematic review also demonstrates that almost all effective interventions (particularly in studies that enrolled children <12 years of age) had a component of family involvement. This could include separate education sessions for parent and child, targeting parents as the sole agent of change, and encouraging parents to lose weight if they were overweight. Therefore, medical students should acquire skills for working with families to optimize treatment effects.
The future implications of your research: The body of research reviewed showed that lifestyle interventions incorporating a dietary component along with an exercise and/or behavioural therapy component are effective for managing childhood obesity and improving the cardio-metabolic outcomes under a wide range of conditions for at least up to one year. Further work is required not only to determine the optimal length, intensity, mode of delivery and the long-term effectiveness of lifestyle interventions, but also to determine what magnitude of weight reduction in the pediatric population is compatible with clinically significant benefits.
Key study points:
1. Patients receiving structured lifestyle interventions show improvements in BMI when compared to patients receiving no care or written instructions.
2. These patients also demonstrate improvements in total cholesterol, LDL, TG, insulin sensitivity, and blood pressure.
3. Lifestyle interventions showed effectiveness across all age groups, BMIs, and in multiple care settings.
Primer: Childhood obesity is a growing medical challenge around the world. Within the United States, over one third of children are overweight (BMI > 85%) or obese (BMI > 95%) with a rising incidence among lower socioeconomic groups. Obesity is related to a broad spectrum of both short-term and long-term health consequences. Obese children are at increased risk for metabolic derangements including impaired glucose tolerance, hypertension, dyslipidemia, and abnormalities in growth and puberty, as well as an increased risk of ischemic cardiac disease as adults. Lifestyle interventions, including both physical activity and behavior modification, have been demonstrated to effectively reduce BMI in children and adolescents; however, fewer studies address the metabolic and cardiovascular benefits of these interventions. This systematic review and meta-analysis addresses the impact of lifestyle modifications on clinical outcomes including fasting insulin, hypertension, LDL, HDL and TG.
Background reading:
2. Up To Date: Comorbidities and complications of obesity in children and adolescents
This [meta-analysis]: evaluated 38 studies conducted between 1975 and 2010 that investigated the effectiveness of dietary intervention on cardiometabolic outcomes, compared with no treatment, minimal advice, or the provision of written educational materials. Nineteen of these studies additionally included physical activity as a component of the lifestyle modification intervention employed. Almost all (33) of the studies evaluated weight loss, and 15 studies evaluated clinical outcomes of lipids, fasting insulin or blood pressure. The studies evaluated interventions with durations between three months and one year in a variety of settings, including hospitals, primary care clinics, schools, and community centers.
Structured lifestyle interventions that included a dietary component lead to more significant weight loss both immediately and up to one year post-treatment, when compared with controls, regardless of the age of the patient, the degree of obesity, or the duration of the intervention. Importantly, significant reductions in LDL, TG, fasting insulin, and blood pressure were also evident. However, no change was seen in HDL levels.
In sum: These data suggest that lifestyle modification, including nutrition education and physical activity, is effective in reducing both BMI and clinical outcomes up to at least one year after the intervention has ended. This meta-analysis is limited, however, in that it includes studies with a high degree of both clinical and statistical heterogeneity, as well as by the use of intermediate clinical outcomes without long-term cardiovascular or metabolic data.
Click to read the study in Pediatrics
By [EH] and [DB]
© 2012 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.