The CHEST-1 & PATENT-1: Riociguat significantly improves exercise capacity in pulmonary hypertension patients
Image: PD
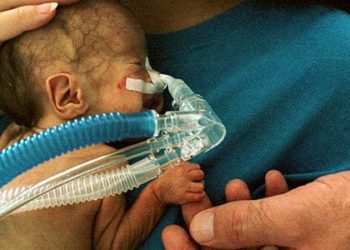
1. In the Chronic Thromboembolic Pulmonary Hypertension Soluble Guanylate Cyclase–Stimulator Trial 1 (CHEST-1), oral riociguat significantly improved exercise capacity as measured by 6-minute walk distance in patients with chronic thromboembolic pulmonary hypertension.
2. In the Pulmonary Arterial Hypertension Soluble Guanylate Cyclase–Stimulator Trial 1 (PATENT-1), oral riociguat significantly improved exercise capacity in patients with pulmonary arterial hypertension, but effect size was similar to that provided by existing pulmonary hypertension medications.
Evidence Rating Level: 1 (Excellent)
Study Rundown: These paired randomized control studies showed that treatment with the soluble guanylate cyclase stimulator riociguat significantly improved exercise capacity in patients with two types of pulmonary hypertension, pulmonary arterial hypertension and chronic thromboembolic pulmonary hypertension. Benefits in exercise capacity were measured by 6-minute walk distance, a surrogate end point that is an independent predictor of death and correlates with changes in functional status and survival. Both studies showed statistically significant benefits in secondary outcomes including pulmonary vascular resistance, NT-proBNP level, and WHO functional class. Oral riociguat acts on the nitric oxide pathway, leading to increased generation of cyclic guanosine monophosphate (cGMP) and ultimately inhibiting vasoconstriction, inflammation, and thrombosis, which are thought to be the pathophysiological underpinnings of these disorders.
The findings of CHEST-1 are particularly meaningful for the management of chronic thromboembolic pulmonary hypertension, which is currently a surgically treated disease and has no approved medical therapy. However, previous research has shown that the benefits of pulmonary endarterectomy performed at a center of excellence surpass the benefits of riociguat reported in the CHEST-1. Therefore, patients who are suitable candidates should continue to undergo surgery for this condition. The findings of the PATENT-1 suggest that riociguat has a comparable effect size to existing treatments for pulmonary arterial hypertension, including bosentan and tadalafil. However, head-to-head studies of these drugs have not yet been conducted. In both studies, patients taking riociguat had similar rates of adverse events as those taking placebo.
Drawbacks to the CHEST-1 and PATENT-1 studies include the fact that they were supported by Bayer HealthCare, which stands to gain substantial revenue should riociguat be approved by the FDA, and the fact that neither study directly assessed the effect of this new pulmonary hypertension drug on the function of the right ventricle.
Click to read the study, published today in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Sildenafil Citrate Therapy for Pulmonary Arterial Hypertension
In-Depth [randomized control trials]: The CHEST-1 and PATENT-1 were international, multicenter, randomized, placebo-controlled clinical trials.
The CHEST-1 enrolled 261 patients who had chronic thromboembolic pulmonary hypertension that was considered to be technically inoperable and patients who had persistent pulmonary hypertension following pulmonary endarterectomy. Subjects were randomized to receive riociguat, dose-adjustable across 12 weeks, or placebo. The primary end point was the change from baseline to the end of week 16 in the distance walked in 6 minutes; secondary end points included pulmonary vascular resistance, NT-proBNP level, and scores on functional scales. At week 16, the 6-minute walk distance increased from baseline by a mean of 39m in the riociguat group, contrasted with a mean decrease of 6m in the placebo group (difference of 46m, 95%CI 25 to 67, P<0.0001); pulmonary vascular resistance decreased by 226 dyn-sec-cm-5in patients receiving riociguat versus an increase of 23 dyn-sec-cm-5 in the placebo arm (P<0.001). Patients receiving riociguat also fared significantly better in terms of WHO functional class. 94% of patients receiving riociguat completed treatment, as compared to 92% receiving placebo.
The PATENT-1 enrolled 443 patients with pulmonary arterial hypertension, including those who were receiving no other treatment and those receiving endothelin-receptor antagonists or non-IV prostanoids. Subjects were randomized to receive dose-adjustable riociguat or placebo. The study had similar primary and secondary endpoints to the CHEST-1. At week 12, the 6-minute walk distance increased from baseline by a mean of 30m in the treatment group versus a decrease of a mean of 6m in the placebo group (difference 36, 95%CI 20 to 52, P<0.001); both pulmonary vascular resistance and NT-proBNP levels decreased significantly.
In both studies, riociguat did not result in significantly greater frequencies of serious adverse events than those observed with placebo.
More from this author: Alternative treatment for acute promyelocytic leukemia promising
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.