Ultrasound-accelerated thrombolysis may improve pulmonary embolism outcomes
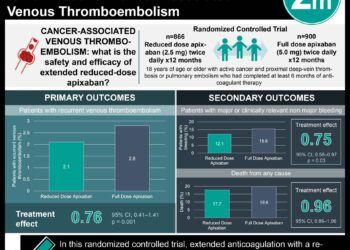
1. In patients with acute submassive pulmonary embolism (PE), ultrasound-accelerated catheter-directed thrombolysis (USAT) safely and effectively improved right ventricular (RV) dysfunction.
2. USAT treatment of acute submassive PE was associated with significantly decreased main pulmonary artery pressure and reduced overall occurrence of acute pulmonary hypertension.
Evidence Rating Level: 2 (Good)
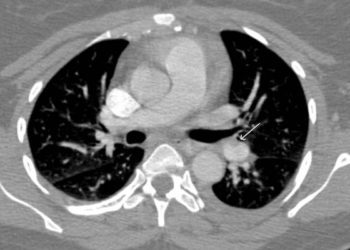
Study Rundown: Acute PE is a potentially life-threatening disease spanning a wide spectrum of outcomes and clinical presentations, ranging from mild shortness of breath to complete circulatory collapse. The main predictors of mortality include systemic arterial hypotension and imaging or biomarker evidence of RV dysfunction at the time of diagnosis. Patients who are hemodynamically unstable are at high risk of death from worsening RV failure and cardiogenic shock. For those at increased risk of death, prompt revascularization by systemic fibrinolysis improves RV dysfunction and may improve survival and recurrent PE. However, systemic thrombolysis is associated with high rates of bleeding complications and guidelines recommend against its routine use. In pursuit of safer treatment and management approaches among patients with PE, therapies associated with a lower risk of adverse events such as USAT are being explored. USAT combines conventional catheter-directed thrombolysis with ultrasound, inducing disaggregation and separation of un-cross-linked fibrin fibers, thus increasing thrombus permeability for thrombolytic drugs. The primary goal of the present study was to retrospectively analyze the safety and efficacy of USAT for submassive PE, defined as PE with evidence of RV dysfunction but without hemodynamic instability. The procedure was successfully completed in all subjects included in the study with minimal complications; all-cause mortality and 30-day readmission rates demonstrated that USAT was a safe method for subjects of this study. Furthermore, USAT was found to be efficacious in this sample, significantly decreasing the main pulmonary artery pressure and improving RV function with minimal complication. The main limitation of this study was its lack of continuing follow up of the subjects’ post-USAT, thus long-term mortality estimates following USAT could not be determined. Future, prospective, controlled trials are necessary before widespread adoption of this treatment method for patients with submassive PE.
Click to read the study in the Journal of Vascular and Interventional Radiology
Relevant Reading: Short-term mortality in acute pulmonary embolism: clot burden and signs of right heart dysfunction at CT pulmonary angiography
In-Depth [retrospective cohort]: This study included data gathered from 45 consecutive patients, all of whom exhibited RV dysfunction as confirmed by right ventricle-to-left ventricle (RV:LV) ratio, who underwent USAT for acute submassive PE with 100% success rate for completion of the procedure. Hemodynamic evaluations were performed immediately after USAT and RV dysfunction was determined using RV:LV ratio evaluation at 48–72 hours after USAT by computed tomography angiography and echocardiography. Adverse outcomes and complications were reported for at least 30 days in each subject. The main pulmonary artery pressure decreased significantly from 49.8 mmHg to 31.1 mmHg (p<0.0001). Moreover, RV dysfunction significantly improved after USAT with mean RV:LV ratios decreasing from 1.59 to 0.93 (p< 0.0001). All-cause mortality at 30 days was 0% in the cohort. Four minor and two major adverse events were recorded, all of which were temporary and without long-term sequelae. No readmissions occurred within the 30-day follow-up period.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.