2 Minute Medicine Rewind March 27, 2017
Prevention of Hereditary Angioedema Attacks with a Subcutaneous C1 Inhibitor
Hereditary angioedema (HAE) is a disabling, potentially life-threatening condition, caused by a deficiency or dysfunction in the C1 inhibitor protein. Current therapy revolves around intravenous C1 inhibitor replacement. In this randomized clinical trial, 90 patients with HAE were randomized to receive twice-weekly subcutaneous injection of a C1 inhibitor (CSL830) or placebo to study the safety and efficacy of this self-administered subcutaneous C1 inhibitor in patients with HAE. Secondary outcomes included the number of times rescue medication was used and the percentage of responders (set as greater than 50% reduction in HAE episodes) as compared to placebo. This study employed a crossover design, where patients received either 40 IU or 60 IU of CSL830 per kilogram of body weight twice weekly followed by placebo, or vice-versa. Researchers found that there was a significant decrease in the number of HAE attacks per month in both the 40 IU/kg and 60 IU/kg groups, with a mean difference of -2.42 attacks per month (95% CI -3.38 to -1.46, p < 0.001) and -3.51 attacks per month (95% CI -4.21 to -2.81, p < 0.001), respectively, compared to placebo. No significant difference was observed between the 40 IU/kg and 60 IU/kg treatment sequences. The number of times rescue medications were needed was also considerably reduced when compared to the placebo, where the mean number of uses per month was reduced from 5.55 (95% CI 3.10 to 8.00) to 1.13 (95% CI -1.44 to 3.69) in the 40 IU/kg group, and 3.89 (95% CI 3.23 to 4.55) to 0.32 (95% CI -0.33 to 0.97) in the 60 IU/kg group. Adverse events, most commonly related to local site reactions, occurred in similar proportions between the intervention and control groups. As this study was limited by a short follow-up period of 14 weeks, the long-term effects of continuous prophylaxis with CSL830 are unknown. Nonetheless, this study shows promise in the use of CSL830 for patients with HAE.
Estimated Perinatal HIV Infection Among Infants Born in the United States, 2002-2013
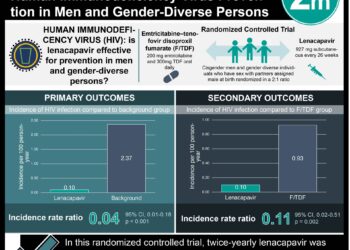
The reduction of vertical transmission of HIV has been promoted through screening to identify HIV-infected mothers, in whom pre- and perinatal antiretroviral therapy can be initiated. In this retrospective cohort study, investigators evaluated data from the Centers for Disease Control and Prevention (CDC) National HIV Surveillance System of births occurring between 2002 and 2013, to assess the incidence of vertical transmission of HIV. The authors also examined characteristics of infants with perinatal HIV infection, including maternal ethnicity, number of maternal prenatal care visits, timing of HIV diagnosis, maternal and child receipt of ARV therapy, breastfeeding status, and mode of delivery. Researchers found that rates of vertical transmission of HIV had decreased from 5.37 per 100,000 live births in 2002 to 1.75 per 100,000 live births in 2013. In examining characteristics of perinatally HIV-infected infants, it was found that 63.0% of mothers were African American, 18.3% were Hispanic, and 13.9% were Caucasian. Among the mothers of all perinatally HIV-infected infants born in 2002-2013, 41.8% were diagnosed with HIV infection prior to the index pregnancy. Only 40% of mothers had at least 1 prenatal visit during the index pregnancy, and 11.2% had no reported prenatal care visits. In addition, while researchers noted an increase in the use of prenatal ARV medications from 28.4% in 2002-2005 to 40.3% during the 2010-2013 study period, only 25.4% of mother-infant pairs received ARV medications prenatally, during labour and after birth from 2002-2013. Breastfeeding was reported by mothers of 10.6% of HIV-infected infants born between 2002 and 2013. This study therefore shows that, despite a reduction in overall perinatal HIV infection in the United Sates, opportunities for prevention continue to be missed. It should be noted that there were considerable gaps in the data used for this study, with 48.9% of cases missing data on variables such as the degree of perinatal care, comorbid conditions such as substance use, and mental health.
Warfarin is classically used as an oral anticoagulant for patients with non-valvular atrial fibrillation (NVAF). This vitamin K antagonist has been known to interfere with γ-carboxylation of glutamic acid residues, inhibiting the activation of bone matrix proteins. Based on an animal study, dabigatran, a non-vitamin K antagonist anticoagulant, has been found to be associated with higher bone volume, smaller trabecular separation, and lower bone turnover rate compared to warfarin. In this retrospective cohort study, investigators analyzed the Clinical Data Analysis and Reporting System (CDARS) of the Hong Kong Hospital Authority for NVAF patients on either dabigatran or warfarin between 2010 and 2014 with primary outcomes including hip or vertebral fracture, death, change of prescription to another oral anticoagulant, or discontinuation of treatment. The study included 8152 patients with 3268 on dabigatran and 4884 on warfarin. A Poisson regression analysis found that, overall, patients using dabigatran had a significantly decreased osteoporotic fracture risk compared to warfarin users (0.7 vs. 1.1 per 100 person-years, RR 0.38 (95% CI 0.22 to 0.66, p<0.001)). When stratified according to patients’ history of falls or fractures, however, a significantly decreased risk of fracture with dabigatran use was seen only among patients with a positive history (RR 0.12, 95% CI 0.04 to 0.33, p<0.001). This study therefore shows that compared to warfarin, the use of dabigatran may be associated with a lower risk of osteoporotic fracture, particularly in patients with a history of falls or fracture. Additional studies using randomized clinical trials may be necessary in better understanding the relationship between the two drugs and osteoporotic fracture risk.
Traditional in-person follow-up visits in the first 30 days following ambulatory surgery may not be convenient for all patients. As such, many centers have now begun substituting in-person follow-up care with care delivered by means of a telephone or mobile app. In this randomized clinical trial, 65 patients undergoing elective breast reconstruction surgery were randomized to receive follow-up care via a mobile app or at an in-person visit within the first 30 days of the operation to determine whether the use of a mobile app can avert the need for in-person follow-up care associated with surgery. The mobile app group had no planned in-person follow up visits at 1 week and 4 weeks after operation, but was replaced by examination of surgical site via photos submitted through the mobile app, and assessment of pain via visual analog scale, and a quality of recovery 9-item questionnaire. Researchers found that patients in the mobile app group were significantly less likely to attend in-person follow-up care during the first 30 days after surgery, with a mean number of visits of 0.66 compared to 1.64 in the in-person group
(RR 0.40, 95% CI 0.24 to 0.66, p < 0.001). This difference was maintained at 3 months postoperatively (RR 0.66, 95% CI 0.46 to 0.95, p=0.03). There was no statistically significant difference between groups with respect to the number of phone calls made to patients’ healthcare professionals, however, the mobile app group did send more emails to their health care providers than the in-person group (RR 4.13, 95% CI 1.55 to 10.99, p = 0.005). Participants from the mobile group also reported higher convenience scores, while no differences were found between complication rates, satisfaction score, or phone communications. While this study was underpowered to assess the impact of the intervention on emergency department visits, this study highlights the potential value of mobile app postoperative care in low-risk ambulatory surgery patients.
Secondhand exposure to electronic cigarette aerosol among US youths
The use of electronic cigarettes (e-cigarettes) has increased considerably. In fact, e-cigarettes are the most commonly used tobacco product among US youths. While e-cigarettes do not produce side-stream emissions, non-users can be exposed to the aerosol produced. This secondhand aerosol (SHA) can contain potentially harmful substances such as nicotine, heavy metals, ultrafine particulate and volatile organic compounds. In this cross-sectional study, 17,711 youths participated in a National Youth Tobacco Survey aimed at determining the prevalence of exposure to SHA. Researchers found that 24.2% of students reported SHA exposure. When stratified according to ethnicity, it was found that exposure ranged from 15.3% among non-Hispanic African Americans, to 27.0% among non-Hispanic white individuals. Researchers also stratified participants according to their use of other tobacco products and found that exposure was 51.5% in current users, 32.3% among former users, and 16.8% among never-users. Overall, SHA was reported among 40.0% of students exposed to second-hand smoke (SHS) and among 8.5% of students not exposed to SHS. This study therefore shows that a significant number of US youths are exposed to SHA from e-cigarettes. This has important implications in the development of tobacco prevention strategies that address both SHS and SHA exposure.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.