2 Minute Medicine Rewind June 17- June 24
June 17 – June 24, 2013
In this section, we will highlight the some of the high-impact studies, updates, and analyses published in medicine during the past week.
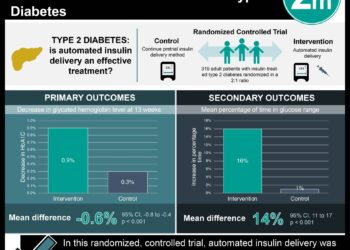
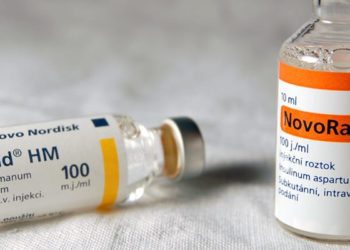
Threshold-Based Insulin-Pump Interruption for Reduction of Hypoglycemia
In this multicenter open label RCT of sensor-augmented insulin pumps for patients with Type I DM and history of hypoglycemic episode, pump interruption at a threshold glucose of <70mg/dL was associated with nocturnal hypoglycemic events (P < 0.001) and fewer documented glucoses <70mg/dL. The threshold was triggered an average of 0.77 times per night, and infusion was interrupted for a median duration of 11.9 minutes. There was no difference in Hgb A1c, insulin dosages, or quality of life metrics between the two treatment and control groups.
Rapid Blood-Pressure Lowering in Patients with Acute Intracerebral Hemorrhage
This multicenter open-label RCT compared a goal SBP <140mmHg vs. a goal SBP <180mmHg in the setting of acute intracerebral hemorrhage. In this study, there was an improvement in Rankin score (evaluation of functional status) with intensive BP treatment (pooled odds ratio for shift to higher modified Rankin score, 0.87; 95% CI, 0.77 to 1.00; P=0.04). There was no statistically significant difference in overall mortality (11.9% vs. 12.0%) or serious adverse events (23.3% vs. 23.6%), however patients in the intensive treatment arm was more likely to withdraw care (5.4% vs. 3.3%; p=0.005).
Crizotinib versus Chemotherapy in Advanced ALK-Positive Lung Cancer
This phase 3 open-label RCT compared 2nd line therapy (cizotinib vs. pemetrexed or doxetrexel) in patients with ALK-positive advanced NSCLC. There was a statistically significant difference in progression-free survival (7.7 months vs. 3.0 months, P < 0.001) and initial response (65% with cizotrinib vs. 29% with pemetrexed and 7% with doxetrexel), however there was no difference in overall survival (interim analysis; 20.3 months vs. 22.8 months; p=0.54).
Endosonography vs Conventional Bronchoscopy for the Diagnosis of Sarcoidosis
In this multicenter RCT, endosonography guided biopsy vs. traditional bronchoscopy and biopsy was compared for the diagnosis of pulmonary sarcoidosis. Significantly more granulomas were detected at endosonography vs bronchoscopy (114 vs 72 patients; 74% vs 48%; P < 0.001).
Seroconversion to Multiple Islet Autoantibodies and Risk of Progression to Diabetes in Children
In this prospective cohort study, investigators identified children with high genetic risk for T1DM and tracked the rate of islet autoantibody seroconversion and eventual development of T1DM. At 10 year follow-up, 69.7% of patients with multiple islet antibodies by age 15 developed T1DM vs. 14.5% of patients with single islet antibody and 0.4% of patients without islet antibodies. Progression to T1DM was faster for patients with earlier islet autoantibody seroconversion.
By David Ouyang
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.