2 Minute Medicine Rewind January 18, 2016
Clostridium difficile infection (CDI) has become a major burden in healthcare and community settings, with limited treatment options available for patients with recurrent, refractory infections. Recently, fecal microbiota transplantation (FMT) has emerged as a promising means of treating recurrent CDI, where high rates of cure have been achieved when administered by enema. Preparing fresh material, however, presents as a logistic difficulty in FMT. As such, to improve access and availability, the use of frozen-and-thawed FMT has been proposed. In this randomized, controlled trial, 232 patients with recurrent or refractory CDI were randomized to receive either fresh or frozen FMT to determine whether frozen FMT is non-inferior to fresh FMT in the treatment of recurrent CDI. The primary endpoint of the study was no recurrence of CDI-related diarrhea at 13 weeks after receiving up to 2 FMTs without the use of antibiotics specifically for CDI recurrence. Based on a modified intention to treat analysis, researchers found that the rate of primary clinical resolution was significantly higher in the frozen FMT group (75.0%) compared to the fresh FMT group (70.3%) (p<0.001). Researchers also found no observed differences in the proportion of serious adverse events between the 2 treatment arms. This study therefore shows that in patients with recurrent or refractory CDI, the use of frozen or fresh FMT results in similar clinical resolution of diarrhea.
A randomized trial of low-cost mesh in groin hernia repair
Groin hernia repair is one of the most frequently performed surgical procedures worldwide. In resource-poor settings, however, there is a limited capacity with high cost of surgical supplies and materials.While synthetic mesh is used in nearly all hernia repairs in high-income countries, this material is unaffordable to many patients in other areas. The use of mosquito meshes represents a low-cost alternative in hernia repair. In countries such as Uganda, the cost of one commercial mesh is $125 USD compared to $ 1 USD for the mosquito mesh alternative. In this randomized controlled trial, 302 males were randomized to receive groin hernia repair with either low-cost or commercial mesh to assess the long-term effectiveness and safety of the low-cost material in a low-income country. Interviews and physical examination were performed at 2 weeks, postoperatively. At this time, 1 death had occurred in the low-cost mesh group, however there were no other severe adverse events in either group. Postoperative complications occurred in 44 patients (30.8%) and 44 patients (29.7%) from the low-cost mesh and commercial mesh groups, respectively (risk difference 1%, 95% CI -9.5% to 11.6%, p = 1.0). The most common postoperative complication in both groups was hematoma or swelling in the groin, followed by impaired wound healing and superficial infection. At 1 year postoperatively, 4 deaths of unknown cause had occurred, where 1 patient had been assigned to low-cost mesh, and the remaining 3 had been assigned to commercial mesh. With respect to long-term effectiveness, 1 patient from the low-cost mesh group (0.7%) experienced a recurrence of hernia, compared to no patients in the commercial mesh group (risk difference 0.7%, 95% CI -1.2% to 2.6%, p = 1.0). This study therefore shows that rates of hernia recurrence and postoperative complications do not significantly differ between men undergoing groin hernia repair with low-cost mesh compared to commercial mesh.
Variceal bleeding is a major complication of cirrhosis. After experiencing a variceal bleeding episode, the risk of rebleeding within 1 year is approximately 60% if left untreated. Current first-line therapy after variceal bleeding consists of non-selective beta-blockers (NSBBs) and repeated endoscopic variceal ligation (EVL) until variceal eradication is achieved. However, even with current treatment, the 2-year risk of rebleeding remains high. As the major determinants of prognosis after variceal bleeding are decreases in portal pressure made through pharmacological treatment and degree of liver dysfunction, recent research has proposed the use of statins in reducing portal hypertension. In this randomized controlled trial, 158 patients were randomized to receive either simvastatin and standard therapy or standard therapy alone to assess whether the use of statins decreases the risk of rebleeding and death in patients with cirrhosis. The study medication was stopped if patients developed the primary endpoint, received a liver transplant or developed drug-related toxicity. Researchers found that patients in the simvastatin group did not have a significantly reduced risk of variceal rebleeding or death (HR 0.82, 95% CI 0.47 to 1.43, p = 0.42). In assessing rates of mortality alone, however, patients assigned to receive both simvastatin and standard therapy were at significantly reduced risk (HR 0.39, 95% CI 0.15 to 0.99, p = 0.030). This corresponded to a 61% reduction in the relative risk of death compared to standard treatment. In a subgroup analysis, there were also no significant differences between treatment groups with respect to the incidence of adverse events (p = 0.72). Two adverse events that were specifically monitored throughout the study were increases in liver transaminases and rhabdomyolysis, the latter of which occurred in 2 patients from the simvastatin group. This study therefore shows that while the addition of simvastatin to standard therapy does not reduce variceal rebleeding risk, it may be associated with a survival benefit for patients with cirrhosis.
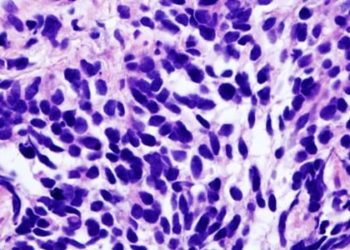
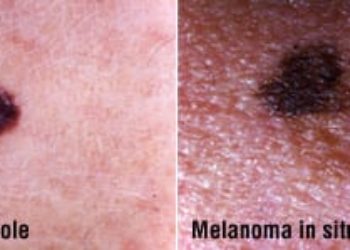
The risk of metastatic spread from malignant melanoma is dependent on histopathological features, including Breslow thickness, mitotic rate and the presence of microscopic ulceration. Whether the surgical margins taken around the primary tumour affect metastatic spread, however, is unclear, despite numerous randomized trials investigating the subject. Current guidelines prescribe a necessary margin of excision for cutaneous melanoma greater than 2 mm in thickness. In a previously conducted randomized controlled trial, 900 patients with high-risk malignant melanoma (Breslow thickness >= 2mm) were randomly assigned to excision margins of either 1 cm (narrow) or 3 cm (wide), the results of which demonstrated that while narrow margins were associated with an increased risk of locoregional relapse, there were no significant differences in overall at survival at 5 years. In the present study, the authors conducted an extended follow-up of a median of 8.8 years, reporting on overall and melanoma-specific survival. In the extended follow-up, researchers found that the rate of death in patients assigned to the 1 cm margin study arm did not significantly differ from patients in the 3 cm group (HR 1.14, 95% CI 0.96 to 1.36, p = 0.14). However, the risk of melanoma-related death was greater in patients assigned to the 1 cm margin group (HR 1.24, 95% CI 1.01 to 1.53, p = 0.041). The estimated absolute difference in melanoma-specific survival at 10 years between the 2 groups was 5.95% (95% CI -0.54% to 12.44%). This study therefore shows that a 1 cm excision margin for malignant melanoma with Breslow thickness greater than 2mm may be inadequate in preventing long-term melanoma-related mortality.
Emphysema is characterized by a loss of lung tissue elasticity, air trapping and hyperinflation. This results in dyspnea, limiting a patient’s ability to exercise and impairing quality of life. Management of severe emphysema is a challenge due to the limited efficacy of currently available treatments. Shape-memory nitinol coils are non-blocking devices that are bronchoscopically-delivered into subsegmental airways to induce regional volume reduction, enhance lung recoil and re-establish small airway tethering. This represents a potentially cost-effective alternative to current lung volume reduction strategies, including surgery. In this randomized controlled trial, 100 patients were randomized to receive usual care or usual care with nitinol coil treatment to evaluate the efficacy, safety and cost-effectiveness of coil treatment in severe emphysema. The primary endpoint of the study was an improvement of at least 54 m in the 6-minute walk test at 6 months. Patients assigned to usual care only were treated at the discretion of the patient’s physician in compliance with international guidelines. This included the use of rehabilitation, inhaled bronchodilators, influenza and pneumococcal vaccination, with or without inhaled corticosteroids, and with or without oxygen. For patients assigned to the nitinol coil group, each lung was assigned a National Emphysema Treatment Trial visual assessment score. The most severely affected lobe of each lung was targeted for coil treatment, and the upper lobe was chosen when ipsilateral scores were the same. At 6 months of follow-up, the authors estimated through multiple imputation that 18 patients from the coil group (36%) and 9 patients from the usual care group (18%) had achieved a 6-minute walk test improvement of at least 54 m (mean difference 18%, 95% CI 4% to unavailable upper limit, p = 0.03). Patients that received coils also exhibited significant improvement on a number of secondary efficacy endpoints at 6 months, including FEV1 (p = 0.001), FVC (p = 0.03), RV (p = 0.01), RV/LTC (p = 0.01), and dyspnea measured through the Modified Medical Research Council dyspnea scale score (p = 0.01) and Transition Dyspnea Index total score (p = 0.04). At 12 months of follow-up, these improvements persisted, however there were no significant differences between groups with respect to the 6-minute walk test. With respect to safety-related outcomes, pneumonia was the most frequent serious adverse event, where it was diagnosed in 9 patients in the coil group (18%) compared to 2 patients receiving usual care (4%) (p = 0.03). The total number of serious adverse events between groups, however, did not significantly differ. The results of a health economic evaluation indicated that the mean difference in QALYs between the 2 groups was 0.061 (95% CI 0.061-0.064, p = 0.02), with an estimated cost-effectiveness ratio of $782, 598 per QALY. The results of this study therefore show that bronchoscopic treatment with nitinol coils compared to usual care may result in improved exercise capacity and measurable lung function, however, improvements in quality of life through this intervention are associated with high costs.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![2MM: AI Roundup- AI Cancer Test, Smarter Hospitals, Faster Drug Discovery, and Mental Health Tech [May 2nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/Untitled-design-350x250.png)