Inhibiting mitochondrial responses after intra-articular fracture slows progression of posttraumatic osteoarthritis
1. Intra-articular fractures (IAFs) often lead to posttraumatic osteoarthritis (PTOA) through mechanisms that involve mitochondria.
2. In a porcine model of IAF, inhibition of mitochondrial electron transport and oxidative stress with amobarbital or N-acetylcysteine (NAC) slowed progression of posttraumatic osteoarthritis.
Evidence Rating Level: 2 (Good)
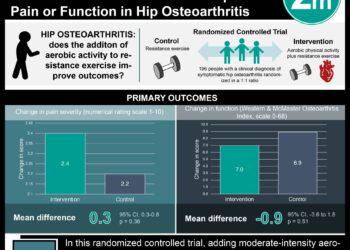
Study Rundown: PTOA is the progressive destruction of articular cartilage in synovial joints that typically occurs after intra-articular fracture. There exist few treatments to prevent the development of PTOA. Previous studies have suggested that progression of PTOA is a result of increased mitochondrial activity of articular chondrocytes. Following from this, the authors of this study explored whether targeting mitochondrial responses slowed the progression of PTOA in a pig IAF model. Using this model, they administered N-acetylcysteine, a nonspecific thiol antioxidant, and amobarbital, an electron transport chain (ETC) complex I reversible inhibitor. Early administration of NAC and amobarbital were both efficacious in slowing PTOA progression and preventing oxidative stress and proton leakage from chondrocyte mitochondrial membranes. Compared to non-treated controls, treated pigs showed improved synovial thickness and a significant increase in proteoglycan content, a measure of chondrocyte quantity. Clinical trials will be necessary to determine whether a similar abrogation of mitochondrial responses is observed in humans treated with these compounds.
Click to read the study in Science Translational Medicine
Click to read an accompanying editorial in Science Translational Medicine
Relevant Reading: Basic Science of Intra-articular Fractures and Posttraumatic Osteoarthritis
In-Depth [animal study]: This study used a porcine hock (ankle) IAF model to investigate whether inhibiting certain mitochondrial responses slowed the development of PTOA. After injury, animals develop PTOA that becomes macroscopically apparent on both the talus and tibia by 6 months. In this study, animals were administered intra-articular injections of either N-acetylcysteine (NAC) or amobarbital, and monitored over the course of 12 months to determine whether either of these compounds could slow the progression of PTOA. Control animals included both normal animals and sham animals which received all surgical procedures and internal hardware except the fracture-inducing impact.
Lysed primary chondrocytes extracted from bovine articular cartilage and treated with amobarbital were shown to display a dose-dependent inhibition of ETC complex I activity (p<0.01). Amobarbital was also shown to be non-toxic to human chondrocytes cultured from surgical discards in the therapeutic 0-5mM range. Minipig IAF animals treated with intra-articular injection of 2.5mM amobarbital or 10mM NAC did not display characteristic macroscopic PTOA lesions, but rather had smoother-appearing articular cartilage. The histologic appearance of the articular cartilage was quantified with automated previously published algorithms into a Mankin score, with lower Mankin scores indicating healthier cartilage. Minimum and average Mankin scores were significantly lower in tissue from amobarbital treated animals (n=7) compared to control animals (n=6).
Treatment of articular tissue harvested 1 week after IAF with NAC increased total glutathione (GSH) and increased the GSSG to GSH ratio (n = 10 for ORIF, n = 7 for ORIF + NAC). Furthermore, intra-articular administration of NAC at the time of injury in the IAF minipig model was shown to decrease proton leakage by mitochondrial membranes (p < 0.05). Early amobarbital treatment was also shown to decrease proton leak in live rabbit chondrocytes harvested 1 week after impact.
Both amobarbital and NAC treatment improved synovial thickness and proteoglycan content throughout the entire depth of the cartilage. Notably, joint-wide indications of inflammation were not significantly altered by NAC treatment or amobarbital, suggesting that the benefits of these treatments were not due to direct inhibition of joint inflammation, but rather a result of inhibition of mitochondria-dependent responses.
Image: PD
©2018 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.