Aggressive blood pressure control may be beneficial for intracerebral hemorrhage [INTERACT2]
Image: PD
1. Intensive lowering of blood pressure in patients with intracerebral hemorrhage did not produce a significant reduction in the primary end point of death or major disability at 90 days.
2. Intensive lowering of blood pressure did reduce the degree of disability at 90 days.
3. Intensive lowering of blood pressure is not associated with increased adverse events.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Acute intracerebral hemorrhage is a form of stroke often accompanied by elevated blood pressures. These pressures must be controlled, but it is not clear what the target blood pressure should be. In 2008, the INTERACT trial showed that a target systolic pressure of 140 mm Hg (compared to a guideline-based target of 180 mm Hg) reduced the volume of blood that accumulated in the brain and did not increase adverse events. This was the basis for the INTERACT2 trial, summarized below.
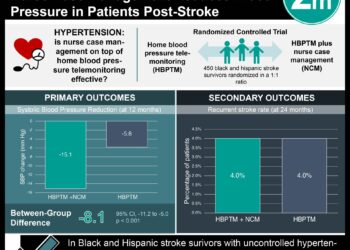
In this trial, the authors were unable to show a significant reduction in the primary end point of death or major disability at 90 days. The final odds ratio was 0.87 (P=0.06). However, a secondary analysis looking more closely at the distribution of disability scores suggests that the intensive treatment strategy does reduce disability overall. In addition, the safety data show that the intensive treatment is well-tolerated.
Although these data suggest benefit and do not show harm from intensive blood pressure management, the matter may not be resolved until the results of additional trials are released.
Click to read the study, published today in the New England Journal of Medicine
Relevant Reading: Intensive blood pressure reduction in acute cerebral haemorrhage trial (INTERACT): a randomized pilot trial
In-Depth [randomized controlled trial]: Nearly 3000 patients with acute intracerebral hemorrhage at centers around the world were randomized to either an intensive treatment strategy targeting a systolic blood pressure of less than 140mmHg within 1 hour of randomization and maintained for 7 days, or a guideline-based standard treatment where blood pressure-lowering treatment was only administered if the blood pressure was higher than 180mmHg.
The primary outcome was death or major disability at 90 days, evaluated using the modified Rankin scale, which ranges from 0 (no symptoms) to 6 (death). Major disability was defined as a score from 3 to 5. The odds ratio for intensive treatment compared to standard treatment was 0.87 (95% CI, 0.75 to 1.01, P=0.06). However, an ordinal analysis showed that the distribution of Rankin scores in the intensive treatment group was shifted towards lower scores, implying less disability.
By Tomi Jun and Mitalee Patil
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.