Aspirin therapy combined with warfarin without clinical indication associated with increased bleeding
1. In this retrospective cohort study conducted in Michigan, aspirin therapy combined with warfarin for patients without a clinical indication was associated with increased rates of major bleeding, emergency visits for bleeding, and hospital admissions for bleeding.
2. Among these patients, there was no difference in rates of thrombosis or mortality.
Evidence Rating Level: 2 (Good)
Study Rundown: Warfarin and aspirin are two of the most widely used medications in North America, however rates of concomitant use without a clear indication are not clear. Apart from patients with recent acute coronary syndrome or mechanical heart valves, there are few clinical indications for this concomitant use. This was a retrospective cohort study looking at propensity matched pairs of patients with atrial fibrillation or venous thromboembolism started on warfarin between 2010 and 2017 in Michigan. The study found that use of aspirin with coumadin without a clinical indication for the aspirin was associated with more overall and major bleeding, more hospital admission and emergency department visits for bleeding. There was no difference in the rates of thrombosis or overall mortality.
The strengths of the study include the large sample size, propensity matching, long follow up, and documentation of time spent in therapeutic INR range. Weaknesses of the study include the retrospective nature of the study and reliance on chart review to identify clinical indications.
Click to read the study in JAMA Internal Medicine
In-Depth [retrospective cohort]: This was a retrospective cohort study of 6359 patients started on warfarin between January 2010 and December 2016 for atrial fibrillation or venous thromboembolism. Follow up occurred until December 2017. Exclusion criteria included receipt of direct oral anticoagulants, myocardial infarction within six months of warfarin initiation, and history of heart valve replacement (mechanical or bioprosthetic). Patients were recruited through the Blue Cross Blue Shield of Michigan–sponsored Michigan Anticoagulation Quality Improvement Initiative (MAQI2) registry. Data was collected on patient demographics, comorbidities, thrombosis and bleeding risk factors, and medications. Primary bleeding outcomes included any patient reported bleeding, major bleeding (as defined by International Society on thrombosis and hemostasis), emergency department visits for bleeding, and hospitalizations for bleeding. Primary thrombosis outcomes included ischemic strokes, transient ischemic attacks (TIAs), acute coronary syndrome/myocardial infarctions (ACS/MI), emergency room visits for thrombosis, and hospitalizations for thrombosis. Mortality data was also collected.
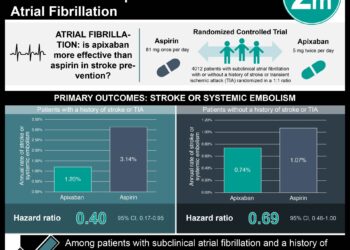
There were 1844 propensity matched pairs (3688 total patients) of patients on warfarin alone versus warfarin with aspirin. 2453 (37.5%) were receiving aspirin without clear indication. In propensity matched groups, patients on aspirin and warfarin had more overall bleeding events (cumulative incidence at one year 26.0% [95% CI 23.8%-28.3%] vs 20.3% [95% CI 18.3%-22.3%] p<0.001), more major bleeding (cumulative incidence at one year 5.7% [95% CI 4.6%-7.1%] vs 3.3% [95% CI 2.4%-4.3%] p<.001), more emergency room visits for bleeding (cumulative incidence at one year 13.3% [95% CI 11.6%-15.1%] vs 9.8% [95% CI 8.4%-11.4.%] p<.001), and more hospitalizations for bleeding (cumulative incidence at one year 8.1% [95% CI 6.8%-9.6%] vs 5.2% [95% CI 4.1%-6.4%] p<.001). There was no difference in thrombotic events for those on aspirin and warfarin (cumulative incidence at one year 2.3% [95% CI 1.6%-3.1%] vs 2.7% [95% CI 2.0%-3.6%] p=0.40). There was no difference in mortality for those on aspirin and warfarin (cumulative incidence at one year 4.4% [95% CI 3.4%-5.6%] vs 3.7% [95% CI 2.8%-4.8%] p=0.34).
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.