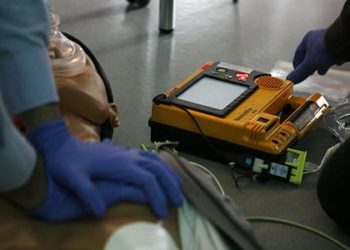
Basic life support associated with greater survival in cardiac arrest
1. Amongst Medicare beneficiaries who experienced an out-of-hospital cardiac arrest in urban areas, those who received basic life support (BLS) had greater survival to hospital discharge and beyond compared to those who received advanced life support (ALS) in the field.
2. Neurologic recovery rates were also higher amongst patients who received BLS compared to those who received ALS.
Evidence Rating Level: 2 (Good)
Study Rundown: There are almost 400,000 cardiac arrests that occur outside of the hospital every year in the US, and 90% of them do not survive to hospital discharge. To improve on this, some organizations have supported teaching advanced life support (ALS) to ambulance providers. Basic life support (BLS) consists of a non-invasive, yet quick strategy, which includes bag-valve masks and automated external defibrillators. ALS is invasive and more sophisticated, including endotracheal intubation, intravenous fluids and drugs, and semiautomatic defibrillation. In several international trials, there has been no evidence that ALS leads to better outcomes than BLS in these situations. This study was performed to compare the effectiveness of the two strategies in the US.
This study, which examined Medicare beneficiaries who experienced an out-of-hospital cardiac arrest in urban areas, showed that a greater percentage of BLS recipients survived to hospital discharge and beyond compared to recipients of ALS. Neurologic recovery rates were also higher amongst patients who received BLS compared to those who received ALS. One of the weaknesses of the study is relying on ICD9 codes to determine the kind of care provided for the patients, since ALS certified providers would always bill to that level regardless of the care they provided. In addition, there may be bias since more ill patients may have received ALS instead of BLS, which would make it difficult to interpret the effectiveness of one strategy over the other. A major strength is the generalizability across most of the urban United States.
Click to read the study, published today in JAMA Internal Medicine
Relevant Reading: Advanced cardiac life support in out-of-hospital cardiac arrest
In-Depth [retrospective cohort]: This study examined a random sampling of Medicare beneficiaries who suffered an out-of-hospital cardiac arrest between 2009 and 2011. Only patients who came from non-rural settings were included in order to compare this study with others. A total of 32,935 ambulance rides were included in the final analysis. BLS care was differentiated from ALS care based on different ICD9 codes, as the billing is different for the two. The primary outcome of the study was survival at hospital discharge, at 30-days, and at 90-days. Secondary outcomes included neurologic recovery.
After propensity score adjustment (which adjusted for demographic and co-morbid conditions), a greater percentage of patients receiving BLS survived to time of discharge (13.1% vs 9.2%; 4.0% difference, 95%CI 2.3-5.7%), at 30-days (9.6% vs 6.2%; 3.4% difference, 95% CI 1.9-4.8%), and at 90-days (8.0% vs 5.4%; 2.6% difference, 95%CI 1.2-4.0). Poor neurologic recovery was lower amongst those receiving BLS vs ALS (6.1% vs 9.7%; 3.5% difference, 95%CI 2.2-4.8). Patients receiving BLS had higher mean medical spending ($11,875 vs $9,097), partially due to these patients surviving longer and receiving more care. All of the aforementioned differences were statistically significant.
More from this author: Non-invasive ventilation linked with lower mortality in COPD exacerbations, Cigarette smoking remains a leading cause of preventable medical problems, Beta-lactam monotherapy may be inferior to combination therapy in pneumonia, Percutaneous intervention outcomes for STEMI similar for women and men, Mechanical aortic valve replacement linked with increased early mortality
Image: CC/GNU Free
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.