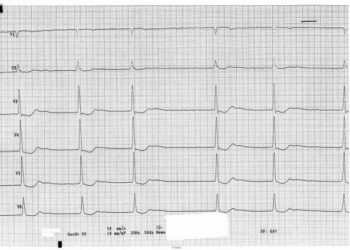
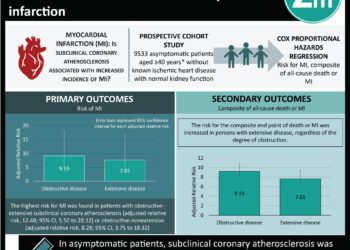
Cardiac troponin elevation without definitive diagnosis associated with higher mortality
1. Among patients admitted for suspected acute coronary syndrome but discharged without a specific diagnosis, higher cardiac troponin levels were associated with elevated all-cause and cardiovascular mortality.
Evidence Rating Level: 2 (Good)
Study Rundown: Cardiac troponin is one of the most commonly ordered lab tests in acute care facilities, and there are numerous cardiac and non-cardiac conditions that can cause troponin elevations. This retrospective cohort study with almost 50,000 patients in Sweden found that among patients admitted to specialized units for suspected acute coronary syndrome who were then discharged without a specific diagnosis, higher levels of cardiac troponin were linked with higher all-cause mortality, myocardial infarction (MI), cardiovascular mortality, non-cardiovascular mortality, hospitalization for heart failure, ischemic stroke, and major adverse events (MAE) defined as composite all-cause mortality and all non-fatal outcomes. This effect remained after correcting for rates of diabetes and hypertension.
This study’s large sample size and long (median 4.9 year) follow up time are major strengths of this study. The main limitation was that there were other clinical differences in the groups, despite accounting for diabetes and hypertension, which may confound the results of the study.
Click to read the study, published today in JACC
Click to read an accompanying editorial in JACC
Relevant Reading: Clinical Use of High-Sensitivity Cardiac Troponin in Patients With Suspected Myocardial Infarction
In-Depth [retrospective cohort]: This was a large (n=48 872) retrospective cohort study using the SWEDEHEART (Swedish Web-system for Enhancement and Development of Evidence-based care in Heart disease Evaluated According to Recommended Therapies) registry. This was a Swedish registry of patients admitted to coronary care units or specialized facilities for suspected acute coronary syndrome (ACS). Recruitment occurred consecutively between January 2005 and April 2013. This study included only patients discharged without a specified diagnosis. Patients were subdivided into 4 groups based on cardiac troponin level: less than or equal to 99th percentile (Group 1), with the remaining patients separated into tertiles (Groups 2-4). Patients were followed until December 31, 2013 (follow-up range 0.5-8.0 years, median follow up 4.9 years). Primary outcomes were all cause mortality, myocardial infarction (MI), cardiovascular mortality, non-cardiovascular mortality, hospitalization for heart failure, ischemic stroke, and major adverse events (MAE) defined as composite all-cause mortality and all non-fatal outcomes. All analyses using cox regression models were adjusted for age, sex, admission year, cardiac troponin assay, and hospital of admission.
There were 39,072 (79.9%) patients had a cardiac troponin level equal to or less then the 99th percentile, with the remaining 9800 (20.1%) split into tertiles based on cardiac troponin. Rates of hypertension, diabetes, and hyperlipidemia increased across increasing strata of cardiac troponin. There were 7,529 (15.4%) patients who had a MAE during the study period. Hazard ratios for all primary outcomes increased with increased strata of cardiac troponin, including all-cause mortality (HR 1.00 vs 1.24 vs 1.58 vs 2.76, p<0.001) cardiovascular mortality (HR 1.00 vs 1.38 vs 2.00 vs 3.27, p<0.001), non-cardiovascular mortality (HR 1.00 vs 1.14 vs 1.30 vs 2.37, p<0.001), myocardial infarction (HR 1.00 vs 1.43 vs 2.08 vs 2.85, p<0.001), heart failure (HR 1.00 vs 1.56 vs 1.77 vs 3.38, p<0.001), ischemic stroke (HR 1.00 vs 1.16 vs 1.35 vs 1.98, p<0.001), and MAE (HR 1.00 vs 1.25 vs 1.53 vs 2.59, p<0.001). Absolute rates of all-cause mortality were 8.9% in Group 1, 15.5% in Group 2, 18.0% in Group 3, and 27.0% in Group 4.
Image: PD
©2019 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.