Casting versus surgery for ankle fractures in older adults
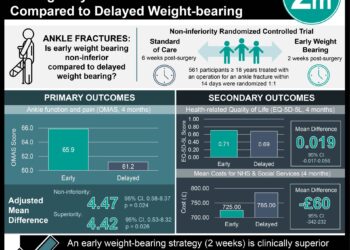
1. Among older adult patients with ankle fractures, close contact casting resulted in similar functional outcomes at 6 months compared to surgery, suggesting casting as appropriate treatment for such patients.
2. There were no significant differences in secondary outcomes between these two groups in terms of quality of life, pain, ankle motion, mobility, and patient satisfaction.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Older adults who sustain an ankle fracture have disproportionately poor outcomes compared to younger patients, and their optimal treatment remains an open question. A new casting technique, close contact casting, uses minimal padding and attains fracture reduction through pressure and anatomic fit.
This blinded, randomized controlled trial evaluated the outcomes of older patients with ankle fractures treated with either close contact casting or surgery. Regarding functional outcomes, close contact casting provided similar results as surgery. However, patients who received casting had lower rates of infection and wound breakdown.
Though the results of this study show that casting may be superior to surgery for older patients with ankle fractures, there are a few limitations. For instance, only a limited number of castings were performed by each surgeon in the study, and differences in performance may exist across sites. Furthermore, functional outcomes were only analyzed up to 6 months after treatment, and a longer term follow-up would give greater certainty on how effective and safe casting is compared to surgery.
Click to read the study in JAMA
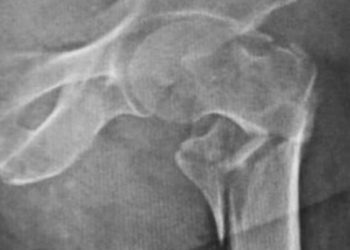
In-Depth [randomized controlled trial]: This study evaluated the effectiveness of close contact casting compared to surgery in improving functional outcomes of older adult patients with ankle fractures. This multicenter, blinded, randomized control study was performed at 24 UK trauma centers and general hospitals. Patients were greater than 60 years of age and had both an acute malleolar fracture and demonstrated ankle joint instability on initial radiograph. The primary outcome measure was the OMAS (Olerud-Molander Ankle Score – 0-100), with a higher score indicating higher function. Secondary outcomes included the 12-item short form health survey (0-100, indicating quality of life), pain (assessed using the OMAS), and patient satisfaction (scale of 1-5).
A total of 620 patients were randomized to receive either surgery (n = 309) or casting (n = 311). Due to various reasons such as surgery cancellation, being lost to follow-up, and withdrawals, 291 patients who received surgery were analyzed at the 6-month time point, and 267 patients who received casting were analyzed. The analyses showed no significant difference in OMAS scores between close contact casting versus surgery at 6 months (mean difference = -0.6 OMAS points; 95%CI -3.9 to 2.6).
There were no differences between secondary outcomes of quality of life (both mental and physical), ankle pain, and patient satisfaction at both 6 weeks and 6 months. There were small differences in ankle mobility at 6 weeks, but no significant difference at 6 months. The number of participants who experienced infection and/or would breakdown was 29/298 (10%) for surgery compared to 4/275 (1%) for close contact casting, yielding an odds ratio of 7.3 (95%CI 2.6-20.2).
Image: CC/Wiki
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.