Discontinuation of oxytocin during active labour may reduce fetal heart rate abnormalities
1. In women undergoing active labour, discontinuation of oxytocin was associated with a slightly higher risk of caesarean section compared to continued oxytocin use.
2. Discontinuation of oxytocin was also associated with decreased uterine hyperstimulation and fetal heart rate abnormalities.
Evidence Rating Level: 1 (Excellent)
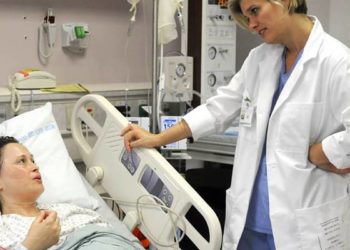
Study Rundown: Labour is induced in about one-in-four pregnant women in the Western world, with oxytocin being the primary drug of choice. Adverse effects of continued oxytocin stimulation include uterine tachysystole and fetal heart rate abnormalities, which could be dangerous for the neonate. One postulated method to combat this is to discontinue oxytocin in the active phase of labour, once the cervix is dilated more than 6 cm. Previous studies have indicated that oxytocin is not needed in the active phase of labour, as contractions have been established, leading to a lower risk of C-section. In this double blind randomized control trial, 1200 women stimulated with IV oxytocin in the latent phase of labour were then randomly assigned to switch to a saline placebo or continue oxytocin once in the active phase. Intention-to-treat analysis of the two groups showed no significant difference in C-section rates between the continued and discontinued group. Secondary outcomes included a longer duration of labour, but a reduced risk of uterine hyperstimulation and fetal heart rate abnormalities for the discontinued group. Other adverse fetal and maternal outcomes were reported and did not differ significantly between the two groups. A major limitation of the study was that a high percentage of women in both groups stopped the study medication during the labour, mostly due to slow progression of labour, even if the criteria was not reached as outlined in the protocol. This could indicate a perception among birth attendants that oxytocin is needed for a safe active labour.
Click to read the study in the BMJ
Relevant Reading: Discontinuation of intravenous oxytocin in the active phase of induced labour
In-Depth [randomized controlled trial]: Between 8 April 2016 and 30 June 2020, 1200 women in nine hospitals in Denmark and one in Netherlands were recruited to the randomized control trial. Eligibility criteria included stimulation with IV oxytocin during the latent phase of labour for either elective induction or following rupture of membranes failing to progress to labour. Once active phase of labour was reached, women were randomized to either continue oxytocin or switch to a saline placebo. Both women, caregivers and trial managers were blinded to this internet-based randomization program. Women were stratified by site, parity and initial reason for IV oxytocin. The primary outcome was caesarean section, which according to intention-to-treat analysis, was not significantly more frequent in the discontinuation group. The relative risk of c-section if oxytocin was discontinued was 1.17 (95% CI 0.90–1.53). Secondary outcomes reported included a longer duration of labour (282 vs. 201 min, P<0.001), reduced risk of hyperstimulation (3.7% v 12.9%, P<0.001), and fetal heart rate abnormalities (27.9% v 40.8%, P<0.001) for the discontinuation group. Other adverse outcomes were similar between groups. Of the 1200 women randomized, 127 never received the allocated intervention, mostly due to rapid progression of labour, but were still analyzed by intention-to-treat. 311 (51.2%) of the placebo group and 197 (33.3%) in the continued group stopped the allocated medicine, primarily because of slow progression of labour. 99 women in the placebo group and 64 women in the continued group discontinued the intervention not in accordance with the study protocol, which led the authors to compare those that adhered to treatment and those that switched to open label oxytocin. They found that those who switched to open label oxytocin had significantly higher c-section rates than those that adhered, even for those women that were assigned to continue oxytocin (5.2% v 29.5%; P<0.0001). Women who did not switch were more likely to be nulliparous, have shorter labours and smaller babies.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.