Early, short-term tranexamic acid does not improve clinical outcomes at 6 months in patients with subarachnoid hemorrhage
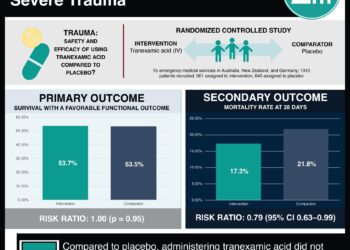
1. Good clinical outcome (mRS 0-3) was observed in 60% of patients in the tranexamic acid group compared to 64% of patients in the control group.
2. The risk of rebleeding, delayed cerebral ischemia, and thromboembolic complications was comparable between groups.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Rebleeding from ruptured aneurysms increases the risk of poor clinical outcomes in patients with CT-confirmed subarachnoid hemorrhage. Although some studies of short-term tranexamic acid have been shown to reduce the risk of rebleeding, its effect on clinical outcome is unclear. This multicenter, randomized controlled trial aimed to determine whether ultra-early, short-term treatment with tranexamic acid improves clinical outcome at 6 months in patients with subarachnoid hemorrhage. Primary endpoint for this study was clinical outcome at 6 months from randomization, assessed by the modified Rankin Scale (mRS), while secondary outcomes included serious adverse events, such as rebleeding, delayed cerebral ischemia, and thromboembolic complications, and all-cause mortality at 30 days and 6 months. According to study results, numerically fewer participants in the tranexamic acid group reported good clinical outcomes (mRS 0-3) compared to those in the control group. In contrast, rebleeding after randomization, but before aneurysm treatment, was modestly decreased in patients receiving tranexamic acid. This study was limited by the lack of longitudinal follow-up as participants were only assessed at 30 days and 6 months post randomization. It is possible that, if assessed for a longer period, an apparent difference in clinical outcome could have been noted. Overall, study results suggest that early, short-term tranexamic acid does not improve 6-month clinical outcomes in patients with spontaneous CT-proven subarachnoid hemorrhage.
Click to read the study in The Lancet
Relevant Reading: Short-term tranexamic acid treatment reduces in-hospital mortality in aneurysmal sub-arachnoid hemorrhage: A multicenter comparison study
In-depth [randomized controlled trial]: Between July 24, 2013, and July 29, 2019, 955 patients were enrolled across eight treatment centers and 16 referring hospitals in the Netherlands. Included patients were those ≥ 18 years with signs and symptoms of subarachnoid hemorrhage, and pathological findings on non-contrast CT. Patients with ongoing treatment for deep vein thrombosis or pulmonary embolism and a history of hypercoagulability disorder were excluded. Altogether, 955 patients (480 in the tranexamic acid group and 475 in the control group) were included in the analysis. Among enrolled patients, the mean age was 58.4 years (standard deviation [SD] 12.4) and 67% (644 of 955) were female. Median time to aneurysm treatment after CT diagnosis was 14 hours (interquartile range [IQR] 5-20, n=708).
Good clinical outcome (mRS 0-3) at 6 months was observed in 60% (287 of 475) of patients in the tranexamic acid group and 64% (300 of 470) in the control group (adjusted odds ratio [aOR] 0.86, 95% confidence interval [CI] 0.66-1.12). No significant difference in clinical outcome was noted between both groups. Excellent clinical outcome (mRS 0-2) was significantly lower in the tranexamic acid group than in the control group (aOR 0.73, 95% CI 0.57-0.95). Additionally, predefined serious adverse events including rebleeding after randomization, but before aneurysm treatment (10% vs. 14%, OR 0.71, 95% CI 0.48-1.04), delayed cerebral ischemia (23% vs. 22%, OR 1.01, 95% CI 0.74-1.37), and thromboembolic complications (11% vs. 13%, OR 0.81, 95% CI 0.48-1.38) were comparable between the tranexamic acid and control groups, respectively. There was no difference in all-cause mortality at 30 days and 6 months. Findings from this study suggest that routine use of tranexamic acid in spontaneous subarachnoid hemorrhage cannot be recommended and alternative strategies should continue to be explored.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.