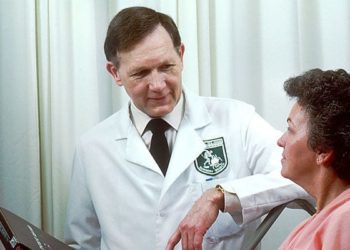
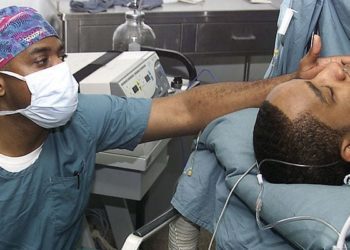
Effects of 24-hour resident physician shifts on patient safety
1. Residents who were randomly assigned schedules without shifts exceeding 24-hours made more serious medical errors when compared to residents working schedules with 24-hour shifts.
2. When accounting for the higher patient volume experienced by residents working under a schedule without 24-hour shifts, there was no increase in medical errors observed.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Over the last decade, there has been significant interest in examining resident work hours and its implications on work quality and patient safety. This, in turn, has been reflected in policy changes from the Accreditation Council for Graduate Medical Education (ACGME) which initially limited first year residents to shifts less than 16 hours in 2011, only to reverse the policy in 2017 upon a number of studies demonstrating the relative safety of extended hour shifts. This study sought to clarify such discrepancies in a population of pediatric residents working in the intensive care unit (ICU). The study found residents who worked schedules without extended (>24-hour) shifts committed higher rates of serious medical errors, preventable adverse events, and near misses when compared to those residents working schedules incorporating 24-hour shifts. This study was well-designed and employed a randomized, cross-over structure across six different study sites. However, its principal finding demonstrated significant site to site variability: three sites reported higher rates of serious medical errors in residents working without extended shifts, two sites reported no difference, and one site reported lower rates of errors. The three sites with highest rates of medical error also had the greatest number of patients per resident. In secondary analysis accounting for the higher patient volume per residents, there was no increase in medical errors observed in residents working without 24-hour shifts. While not designed to specifically test this claim, the study provided some initial evidence that it may be the increased workload that accounted for the higher rates of error committed by residents working schedules without 24-hour shifts. Additional limitations of the study included its focus on pediatric ICU residents, which may limit generalizability and lack of standardization in identification of medical errors. The study also examined only a single schedule structure without extended shifts and involved an integration of day and night shifts which may contrast from a more continuous night-float style of schedule increasingly favored by training programs.
Click to read the study, published today in NEJM
Relevant Reading: Patient Safety Outcomes under Flexible and Standard Resident Duty-Hour Rules
In-Depth [randomized controlled trial]: This study took place from July 2013 to March 2017 across six pediatric intensive care units in the United States. Included ICUs were all staffed by second year residents or above and had been employing schedules with extended hour shifts for residents, which in general were required every third or fourth shift. Study sites were randomized to intervention (elimination of 24-hour shifts for residents) and control schedules. Each site ultimately served as its own control. A four month wash-in period was followed by eight months of data collection with each site following the intervention or control schedule exclusively during this time. This was followed by a four month wash out period, after which each study site then assumed the alternate schedule structure for a subsequent eight month period. Errors were identified by physician observers and chart reviews. A total of 38,821 patient-days were included in the analysis. Resident physicians without extended shift schedules had a higher rate of serious medical error (RR 1.53; 95% CI 1.37-1.72), preventable adverse events (RR 4.03; 95% CI 2.94-5.53), and near misses (RR 1.42, 95% CI 1.26-1.59) when compared to residents with extended shift schedules. In secondary analysis adjusting for the number of patients per resident as a continuous variable, residents working without extended shifts demonstrated a lower risk of serious error (RR 0.54, 95% CI 0.35-0.85) – though significant variability in relative risk estimates were noted when accounting for patient volume as a categorical variable, suggesting instability of the modeling. Work hours were lower (61.9 ± 4.8 vs 68.4 ± 7.4 hours) and sleep hours per week were higher (52.9 ± 6.0) vs 49.1 ± 5.8 hours) in residents working schedules which had eliminated 24-hour shifts.
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.