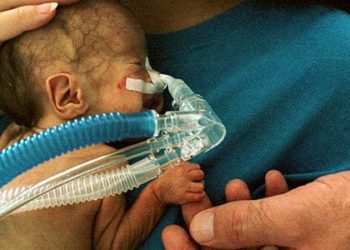
Fetoscopic endoluminal tracheal occlusion improves infant survival for congenital diaphragmatic hernia
1. Fetoscopic endoluminal tracheal occlusion (FETO) was shown to improve survival to discharge in infants with severe left congenital diaphragmatic hernia.
2. The FETO surgical procedure increased rates of preterm, prelabor membrane rupture preterm birth.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Severe congenital diaphragmatic hernia is a birth defect where abdominal contents herniate through the diaphragm and interfere with airway and pulmonary vascular development. Without medical intervention, these patients experience high rates of infant death due to respiratory failure and pulmonary hypertension. FETO, a surgical procedure inflating a balloon within the trachea of the fetus, decreases early neonatal respiratory complications. As such this study investigated the efficacy of FETO in infants with congenital diaphragmatic hernia. The study determined infants receiving FETO had a higher rate of survival to discharge compared to the control group. However, mothers in the FETO group notably experienced higher rates of preterm, prelabor rupture of membranes, and preterm birth. The major limitation of this study was the inability to assess the long-term outcomes of the procedure. Additionally, given that this procedure is highly specialized, and the trial was performed at an experienced fetoscopy center, data on rates of complications and its efficacy at less-experienced centers is warranted. Nonetheless, the study’s results are significant as the results provided evidence for the use of FETO in improving outcomes for infants with severe congenital diaphragmatic hernia.
Click to read the study in NEJM
Relevant Reading: Predictors of neonatal morbidity in fetuses with severe isolated congenital diaphragmatic hernia undergoing fetoscopic tracheal occlusion
In-Depth [randomized controlled trial]: This study enrolled 80 pregnant mothers from 26 neonatal care centers in 12 countries. Patients with a maternal age of 18 years or older carrying a singleton pregnancy, confirmed fetal congenital diaphragmatic hernia, and severe pulmonary hypoplasia on the left side was included in the study. Patients with an elevated risk of preterm birth or maternal conditions increasing the risk of fetal surgery were excluded from the study. The patients were randomized in a 1:1 ratio to either receive FETO or expectant care, respectively. In the FETO group, balloon placement occurred between 27 to 29 weeks of gestation while removal of the balloon occurred around 34 weeks of gestation. The primary outcome was survival to discharge defined as the percentage of fetuses that were healthy to progress to discharge from the neonatal intensive care unit (NICU), post-delivery. Infants in the FETO group experienced significantly higher survival to discharge at 40% (16 of 40) compared to 15% (6 of 40) in the expectant care group (relative risk [RR], 2.67; 95% confidence interval [CI], 1.22-6.11, two-sided P=0.009). All surviving infants progressed to 6 months of age. The study was stopped early for superior efficacy in accordance with the O’Brien-Fleming stopping rules. Additionally, 47% of mothers in the FETO group experienced preterm, prelabor rupture of membranes compared to 11% in the expectant care group (RR, 4.51; 95% CI, 1.83-11.9), and 75% of mothers in the FETO group experienced preterm birth compared to 29% in the expectant care group (RR, 2.59; 95% CI, 1.59-4.52). Overall, FETO provided improved survival to discharge to 6 months of age in fetuses with severe, left congenital diaphragmatic hernia at the increased risk of preterm, prelabor membrane rupture, and delivery.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.