Fusion for spinal stenosis not associated with improved clinical outcomes: the Swedish Spinal Stenosis Study
1. Fusion surgery for lumbar spinal stenosis was not associated with better clinical outcomes than decompression alone.
2. Patients randomized to fusion surgery had significantly higher medical related costs than those randomized to decompression alone.
Evidence Rating Level: 1 (Excellent)
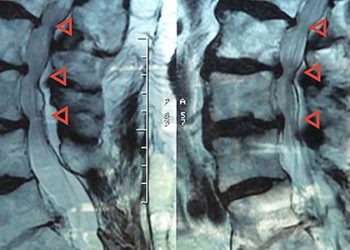
Study Rundown: Lumbar spinal stenosis is a narrowing of the spinal canal that compromises neural structures and significantly impairs quality of life. Current evidence suggests spinal surgery – spinal decompression with or without spinal fusion – is superior to conservative management when the latter has failed for over six months. However, there is a paucity of RCTs evaluating whether the perceived benefit of spinal fusion is clinically significant. The Swedish Spinal Stenosis Study (SSSS) was a multicenter trial that used clinically validated patient-reported data and the 6-minute walk test to measure their outcomes. The study found no significant difference in outcome between decompression surgery alone or decompression surgery with spinal fusion. They also found the use of spinal fusion was associated with substantial increased costs.
Strengths of this trial were the inclusion and exclusion criteria that created similar groups that were randomly distributed to either the decompression alone or fusion and decompression arm. Only clinically objective data was used during follow-up to assess outcomes. Additional RCTs are needed to evaluate whether there may be more specific indications for fusion surgery in patients with degenerative spinal stenosis or if longer follow-up is needed to fairly assess clinical outcomes.
Click to read the study, published today in NEJM
Relevant Reading: Trends, major medical complications, and charges associated with surgery for lumbar spinal stenosis in older adults
In-Depth [randomized controlled trial]: The SSSS was a randomized controlled trial that evaluated the clinical benefit of adding a spinal fusion to decompression surgery in patients with symptomatic degenerative lumbar spinal stenosis for greater than 6 months. After adjusting for exclusion criteria and follow-up, 111 patients who underwent decompression surgery plus fusion surgery and 117 who underwent decompression surgery alone were evaluated (n=228). The primary outcome was the score on the Oswestry Disability Index (ODI). Also, the 6-minute walk test was performed at baseline and at follow-up. Additional validated questionnaires for quality of life and pain were used secondarily. Imaging was not used. Follow-up was done 2 years and 5 years’ post-surgery.
There was no significant difference in the mean ODI score at 2 years (27 in decompression plus fusion group and 24 in decompression only group, p=0.24) or 5 years (27 in decompression plus fusion group and 28 in decompression only group, p=0.24) follow-up. There was also no significant difference in results of the 6-minute walk test at 2 years (p=0.72). A post hoc analysis at 2 years indicated no difference in ODI score depending on the degree of vertebral slip (p=0.98). The mean direct costs were $6,800 higher in the decompression plus fusion group than decompression alone.
Image: PD
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.