Gestational weight loss may improve outcomes for obese women
Image: PD
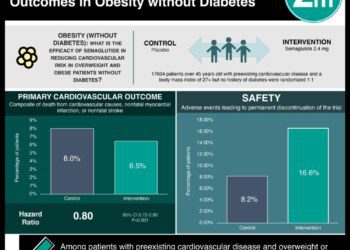
1. Among obese women, gestational weight gain was associated with adverse pregnancy outcomes, including need for cesarean delivery and large for gestational age infants.
2. Gestational weight loss was associated with the lowest average probability of adverse maternal and neonatal outcomes.
Evidence Rating Level: 2 (Good)
Study Rundown: This study found that among obese women, the probability of multiple adverse pregnancy outcomes (need for cesarean delivery, postpartum hemorrhage, large for gestational age infants, and NICU admission) increased with increasing gestational weight gain. The Institute of Medicine currently recommends a 5-9 kg gestational weight gain in women with a body mass index (BMI) ≥30 kg. The results of this study suggest that this guideline may result in sub-optimal maternal and neonatal outcomes, particularly among women with BMI ≥40 kg and that more specific recommendations for different classes of obesity may be warranted.
Strengths of this study include a large sample size and evaluation of multiple pregnancy and neonatal outcomes. Limitations include self-reported weight, retrospective analysis and the lack of a comparison group. Future studies might include a prospective study design and inclusion of individuals with a normal BMI as a reference group.
Click to read the study in the American Journal of Obstetrics and Gynecology
Relevant Reading: IOM: Weight gain during pregnancy – reexamining the guidelines
In-Depth [retrospective cohort study]: This study evaluated pregnancy and neonatal outcomes among obese women by gestational weight change and BMI class [Class I: BMI 30.0-34.9 kg/m2, II (BMI 35.0-39.9 kg/m2) or III (BMI ≥ 40 kg/m2)]. Data was drawn from the Consortium on Safe Labor database and included pregnancies of 20,950 obese women with a term liveborn singleton from 2002-2008. Weight change was classified as weight loss (<0 kg), low weight gain (0-4.9 kg), normal gain (5.0-9.0 kg) or high weight gain (>9.0 kg). The incidences of operative vaginal delivery, cesarean delivery and postpartum hemorrhage as well as a range of neonatal outcomes (birth weight, shoulder dystocia, 5 minute Apgar score <7, NICU admission) were assessed.
Class I obese women who lost weight during pregnancy were less likely to have a cesarean delivery (OR 0.21, CI 0.11-0.42) while also being more likely to have deliver a small for gestational age infant (OR 1.8 CI 1.3-2.5). Across all BMI classes, obese women with high pregnancy weight gain (>9.0kg) were more likely to give birth to an infant large for gestational age (class I OR 2.4, CI 1.9-2.9; class II OR 1.7, CI 1.3-2.1; class III OR 1.6, CI 1.3-2.1). The average predicted probability of cesarean, postpartum hemorrhage, and NICU admission also increased with increasing weight gain.
By Denise Pong and Leah Hawkins
More from this author: Chromosomal analysis not cost effective in evaluation of recurrent miscarriage, Light drinking during pregnancy may be safe, Significant racial disparities in preterm births in infants conceived by IVF
© 2013 2minutemedicine.com. All rights reserved. No works may be reproduced without written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT. Content is produced in accordance with fair use copyrights solely and strictly for the purpose of teaching, news and criticism. No benefit, monetary or otherwise, is realized by any participants or the owner of this domain.