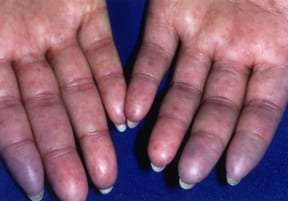
Patient Basics: Scleroderma
Originally published by Harvard Health.
What Is It?
Scleroderma is a poorly understood illness that causes widespread hardening of the skin, especially on the hands and face. It also can damage the lungs, heart, kidneys, digestive tract, muscles and joints. It is a long-lasting (chronic) autoimmune disorder, an illness in which the body’s immune defenses mistakenly attack the body’s own cells rather than protecting them from outside invaders. Scleroderma also is called progressive systemic sclerosis.
There are two types of scleroderma. In the limited form, also called limited systemic sclerosis, the skin is the primary target. In the diffuse form (diffuse systemic sclerosis), the damage not only affects the skin, but also can affect the lungs, kidneys and other internal organs.
In people with scleroderma, scientists have identified abnormal immune proteins called autoantibodies, which are programmed to attack specific components of body cells. They also have found abnormal accumulations of protective T cells (white blood cells that are part of the immune system) in the skin and elsewhere.
Although scientists don’t understand exactly what happens, they believe that the immune system, perhaps involving these autoantibodies or T cells, somehow damages the body’s smallest arteries, called arterioles. These damaged arterioles leak fluid, which causes swelling. They also release chemical factors that stimulate cells called fibroblasts to produce too much collagen, a fibrous protein.
In the skin, this leads to thickening, hardening and tightness. Elsewhere in the body, the autoimmune attack of scleroderma can damage the digestive tract, the linings of joints, the outside sheaths of tendons, muscles (including the heart muscle), portions of the heart that regulate heart rhythm, the small blood vessels and the kidney.
Scleroderma is rare, affecting about 14 in every 1 million people worldwide. It is most common in women aged 35 to 54. The cause is unknown. For some reason, cells called fibroblasts make too much scar-type tissue in the skin and in organs throughout the body.
A number of theories have been proposed to explain this, including abnormalities in blood vessel function, abnormal proteins and antibodies in the circulation, and abnormal amounts of chemical messengers instructing fibroblasts to become overly active. Because scleroderma is more common in women during the childbearing years, researchers have looked for a pregnancy-related factor to explain why scleroderma develops. One theory suggests that leftover fetal cells can still be circulating in the mother’s bloodstream decades after pregnancy, and may play some role in triggering the autoimmune changes behind scleroderma. Genetic factors and infectious triggers have also been proposed.
Older studies have linked scleroderma to exposure to certain chemicals, including vinyl chloride, epoxy resins, aromatic hydrocarbons and ingestion of rapeseed oil adulterated with aniline. Some people who took tryptophan, an amino acid that used to be sold as a dietary supplement, developed a condition similar to scleroderma called eosinophilia myalgia syndrome. Since tryptophan was removed from the market, no further cases of eosinophilia myalgia syndrome have been reported. But the clear link between tryptophan and eosinophilia myalgia syndrome and the scleroderma-like disease associated with contaminated rapeseed oil ingestion raise the possibility that exposure to something in the environment could trigger scleroderma.
Symptoms
The symptoms of scleroderma vary from person to person and can include:
- Raynaud’s phenomenon. In people with this condition, blood vessels in the fingers or toes, and sometimes in the tips of the nose and ears, suddenly constrict. The area turns white or blue and becomes cold and numb. This is followed by a flush of redness as the area warms up again, often together with pain or tingling. Raynaud’s phenomenon can be triggered by exposure to cold or vibration or by emotional stress.
- Skin symptoms. There can be swelling of the fingers, hands, forearms and face and sometimes the feet and lower legs. This is followed by a skin thickening and tightness that can limit body movement. There also can be:
- Skin ulcers
- Skin that is lighter or darker than usual
- Loss of hair
- Abnormal skin dryness, including vaginal dryness
- Calcium deposits in the skin (subcutaneous calcinosis)
- Small red spots caused by localized swelling of tiny blood vessels (telangiectasias)
- Joints. Joints can swell and become painful and stiff.
- Muscles. Muscles can become weak, and tendons can become abnormally thick, causing pain and limited joint motion.
- Digestive system. When scleroderma involves the esophagus, it can cause a feeling of fullness or burning pain (heartburn) in the upper abdomen or behind the breastbone, together with difficulty swallowing or keeping food down. Other digestive symptoms include bloating, constipation, lower abdominal pain or difficulty controlling bowel movements.
- Lungs. Symptoms can include shortness of breath, especially when you exercise, and a dry cough that doesn’t bring up sputum or mucus.
- Heart. Problems can include chest pain, abnormal heart rhythms and heart failure.
- Kidneys. Kidney damage can lead to high blood pressure, headache, seizures and too little urine being made.
- Other symptoms. Other symptoms can include dry eyes and mouth, sudden episodes of severe facial pain (trigeminal neuralgia), and impotence.
More than 95% of people with scleroderma have both Raynaud’s phenomenon and skin thickening (also called sclerodactyly when the fingers are involved). In addition, those with limited scleroderma tend to have telangiectasias (85% of patients); digestive problems involving the esophagus (80%); and calcinosis (50%), often called CREST syndrome (calcinosis, Raynaud’s, esophageal disease, sclerodactyly and telangiectasia).
Besides having Raynaud’s phenomenon and skin thickening, people with the diffuse form of scleroderma can have digestive symptoms involving the esophagus (80%), joint symptoms (70%), muscle weakness (50%), lung symptoms (40%) and heart failure (30%).
Diagnosis
Your doctor will ask about your symptoms and will examine your skin, especially on your fingers, hands and face. If your doctor suspects you have scleroderma, he or she may want to order blood and urine tests. Occasionally, a skin biopsy may be recommended during which a small sample of skin is removed and examined in a laboratory. If scleroderma affects internal organs such as the heart, lungs or digestive organs, a chest X-ray and other tests may be necessary.
Expected Duration
Scleroderma is a chronic (long-lasting) disease. Although symptoms may come and go over time, the various forms of this disease usually last a lifetime. The skin swelling that happens first can last for a few weeks or months. This is followed by a gradual thickening of the skin and other skin changes. In the diffuse form of the disease, skin symptoms tend to peak within three years, then stabilize or even improve. If skin changes occur more rapidly, there is often a greater risk that internal organs are being damaged as well. In limited scleroderma, skin symptoms tend to worsen very slowly over a period of many years.
Prevention
There is no way to prevent scleroderma.
Treatment
There is currently no treatment for scleroderma that is reliably effective. A host of drugs have been tried or are in development for the treatment of scleroderma. Among the most commonly prescribed drugs for scleroderma are:
- Cyclophosphamide (Cytoxan, Neosar) also decreases the activity of the immune system, and has been shown to improve lung function when used along with corticosteroids in people with inflammation in the lungs. The risks associated with this powerful medication (including infection, bleeding from the bladder and an increased risk of cancer) require that its use be highly selective and closely monitored.
- Glucocorticoids can be used to relieve inflammation of the membrane surrounding the heart (pericarditis), arthritis and inflammation of the muscles (myositis). However, these drugs also can have serious side effects, including the possibility that they may increase blood pressure and worsen kidney function in people with scleroderma.
- Non-steroidal anti-inflammatory drugs (NSAIDs) may be useful for joint and tendon inflammation.
- D-penicillamine (Cuprimine) decreases the activity of the immune system, and is thought to interfere with collagen production. Some studies suggest that D-penicillamine may reduce skin thickening and prevent organ damage in some patients, but its overall success rate is not high. It also can cause serious side effects that harm the kidneys and blood cells. It is being used much less now than in the past to treat scleroderma.
- Diuretics encourage the body to release excess fluid as urine. They are used to relieve swelling of the hands and feet.
- Omeprazole (Prilosec) or related medications may be quite effective for the heartburn related to esophageal disease.
- Bosentan (Tracleer) or epoprostenol (Flolan) may be effective for a potentially serious condition called pulmonary hypertension in which the blood pressure in the lung’s blood vessels is elevated. These drugs also may improve symptoms of Raynaud’s phenomenon.
- Angiotensin converting enzyme (ACE) inhibitors, such as enalapril (Vasotec), lisinopril (Prinivil or Zestril) or captopril (Capoten), lower blood pressure and may protect the kidney in people with scleroderma.
A promising experimental therapy for severe disease is high dose immunosuppression with stem cell treatment.
Many patients find relief from Raynaud’s phenomenon by limiting their exposure to cold and by wearing warm clothing, especially mittens and socks. Others find that regular exercise, physical therapy, skin massage and moisturizing ointments help skin symptoms. If dry skin becomes ulcerated and infected, antibiotics may be needed.
For more severe cases, medications may be necessary. These include calcium channel blockers such as amlodipine (Norvasc), nifedipine (Procardia, Adalat) or diltiazem (Cardizem), hydralazine (Apresoline), prazosin (Minipress), losartan (Cozaar), sildenafil (Viagra) or tadalafil (Cialis). Each of these medications may have side effects that limit their use.
As an alternative to medication, some patients choose biofeedback or injections called nerve blocks. These injections are given under local anesthesia near the neck, armpit or hand and usually are done only after other approaches have not worked. The injections temporarily or permanently interrupt nerve signals to blood vessels. By removing the nerve signals that tell an artery to constrict, arteries can dilate and improve blood flow.
Patients also are urged not to smoke and to avoid street drugs and certain prescription drugs including beta-blockers, amphetamines, cocaine and ergotamine (Gynergen and other brand names).
When To Call a Professional
Call your doctor if you think that you are experiencing episodes of Raynaud’s phenomenon or other symptoms of scleroderma, especially if you are a woman of childbearing age.
Prognosis
While many people with scleroderma live long, full lives, the death rate is increased by up to eight times for diffuse disease and two times for limited disease. Pulmonary hypertension and diffuse skin disease are risk factors for poor prognosis. However, longevity in this illness seems to be improving over time. Its rarity and variability make it difficult to accurately predict the prognosis in an individual with scleroderma.
Additional Info
American College of Rheumatology
1800 Century Place
Suite 250
Atlanta, GA 30345-4300
Phone: 404-633-3777
Fax: 404-633-1870
http://www.rheumatology.org/
National Institute of Arthritis and Musculoskeletal and Skin Diseases
Information Clearinghouse
National Insitutes of Health
1 AMS Circle
Bethesda, MD 20892-3675
Phone: 301-495-4484
Toll-Free: 1-877-226-4267
Fax: 301-718-6366
TTY: 301-565-2966
http://www.niams.nih.gov/
Scleroderma Foundation
12 Kent Way
Suite 101
Byfield, MA 01922
Phone: 978-463-5843
Toll-Free: 1-800-722-4673
Fax: 978-463-5809
http://www.scleroderma.org/
Scleroderma Research Foundation
220 Montgomery Street
Suite 1411
San Francisco, CA 94104
Phone: 415-834-9444
Toll-Free: 1-800-441-2873
Fax: 415-834-9177
http://www.sclerodermaresearch.org