Poor humoral response observed in patients undergoing hemodialysis following a single dose of the BNT162b2 SARS-CoV-2 vaccine
1. The findings of this prospective cohort study suggested poor humoral immune response following a single dose of the BNT162b2 COVID-19 vaccine in the hemodialysis patient population compared to two doses.
2. Based on the findings in this study, the second vaccine dose should not be delayed in patients receiving chronic hemodialysis and should adhere to the recommended vaccination schedules set by the manufacture.
Evidence Rating Level: 2 (Good)
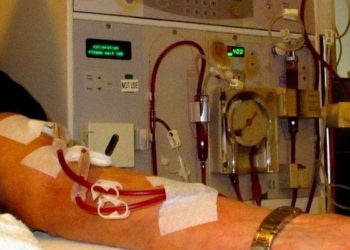
Study Rundown: Patients undergoing hemodialysis often need to visit medical facilities multiple times per week to receive life-sustaining treatments. Despite adherence to public health protocols during the COVID-19 pandemic, these patients were 5 times more likely to be infected with COVID-19 and were associated with a high mortality rate compared to the general population. Furthermore, recent randomized clinical trials evaluating the efficacy of COVID-19 vaccines included few patients with kidney disease, a patient population known to have diminished immune response to vaccination through previous studies for the hepatitis B vaccine. This prospective observational cohort study sought to investigate the humoral response conferred by the BNT162b2 (Pfizer-BioNTech) COVID-19 vaccine in patients undergoing maintenance hemodialysis. This was done by measuring SARS-CoV-2 immunoglobulin G (IgG) antibody levels following 1 vs 2 doses of the vaccine compared to health care workers serving as controls and convalescent serum. The main measures of the analysis were SARS-CoV-2 IgG antibodies to the spike protein (anti-spike), receptor binding domain (anti-RBD), and nucleocapsid protein (anti-NP). In total, humoral response was measured in 66 patients with 1 dose of the vaccine sampled 28 days post-vaccination and 76 patients with 2 doses sampled 14 days after the second dose, for a total of 142 patients and 35 control subjects. Among individuals with a single dose of the vaccine, 6% developed anti-RBD response above the median level of convalescent serum vs 41% of individuals with 2 doses at 1 week, progressing to 60% efficacy by 2 weeks. These findings suggested a poor humoral immune response following a single dose of the BNT162b2 COVID-19 vaccine in the hemodialysis patient population, further indicating that the second dose should not be delayed in this population. A limitation of this study was the small size of the patient cohort given that this was a single-center study, limiting follow-up and the complete evaluation of all factors associated with humoral immune response.
Click to read the study in JAMA Network Open
Relevant Reading: COVID-19 in patients undergoing long-term dialysis in Ontario
In-Depth [prospective cohort]: This prospective, single-center cohort study was conducted from February to April 2021 and included 142 patients (94 [66%] men; median age [IQR], 72 [62-79] years) undergoing maintenance hemodialysis and 35 health care worker controls from Toronto, Canada. SARS-CoV-2 IgG antibodies were measured in 66 patients with 1 vaccine dose, 76 patients with 2 doses, and 35 health care workers with 2 doses. Anti-NP antibodies suggestive of natural SARS-CoV-2 infection was detected in 15 of 142 (11%) patients at baseline, however, only 3 patients had previously confirmed COVID-19 through polymerase chain reaction testing. Additionally, 2 patients contracted COVID-19 after receiving 2 doses of the BNT162b2 vaccine. In 66 patients with 1 dose, seroconversion was detected in 53 (80%) for anti-spike and 36 (55%) for anti-RBD by 28 days post-vaccination. However, a more robust immune response, defined by reaching the median levels of antibodies in convalescent serum from COVID-19 survivors, was detected in only 15 patients (23%) for anti-spike and 4 (6%) for anti-RBD. Among 76 patients with 2 doses, seroconversion was detected in 69 of 72 (96%) for anti-spike and 63 of 72 (88%) for anti-RBD by 2 weeks after the second dose. Furthermore, median levels of antibodies in convalescent serum from COVID-19 survivors were detected in 52 of 72 patients (72%) for anti-spike and 43 of 72 (60%) for anti-RBD. In contrast, all 35 health care worker controls reached and exceeded the median level of anti-spike and anti-RBD detected in convalescent serum within 2 to 4 weeks after the second dose.
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.