Preperitoneal mesh placement a valid option for ventral hernia repair
Image: PD
1. Open ventral/incisional hernia repair in complex patients can be done with mesh placement in the preperitoneal space with low mesh infection and recurrence rates.
2. Biologic, lightweight and C-QUR mesh placement was associated with higher rate of recurrence.
Evidence Rating Level: 4 (Below Average)
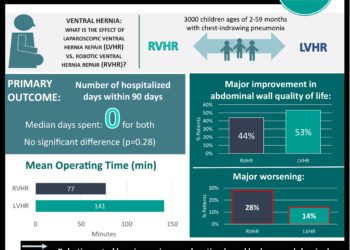
Study Rundown: Authors analyzed preperitoneal ventral hernia repair outcomes of complex patients with multiple comorbidities and prior abdominal surgeries. Their preperitoneal mesh placement technique allowed tremendous overlap between the mesh and tissues surrounding the hernia, allowing for mesh-to-defect ratios of 4:1 and reaching as far as the psoas muscles bilaterally. This method of repair leaves the peritoneum intact, protecting bowel from adhering to the mesh. The choice of mesh and type of ventral hernia repair remains controversial for lack of concrete evidence and this large case series supports the use of preperiotonial mesh placement only in patients with high BMI and co-morbidity rate. This study is limited by its lack of a comparison cohort, its retrospective nature and lack of randomization. However, this is a large case series that examined a set of complicated patients with a complex, widespread and costly issue.
Click to read the study in JACS
Relevant Reading: Prospective, Long-Term Comparison of Quality of Life in Laparoscopic Versus Open Ventral Hernia Repair
In-Depth [retrospective case series]: This study examined 768 patients that underwent open ventral hernia repair with preperitoneal mesh placement at the Carolinas Hernia Center. Most patients were women with an average age of 56, and on average had two or more comorbidities. Almost all have previously undergone an intra-abdominal procedure and 70.3% have had a hernia in the past, with over two prior attempts to repair the hernia on average. Over ninety-five percent were ventral/incisional hernia repairs of signficant size (average area of 205.2 cm2). Almost 90% of repairs utilized synthetic mesh and the rest used biologic implants. The rate of recurrence was 6.1% and the incidence of mesh infection was 2.4%, which are both remarkably low for VHR in a such a complex population. Wound complications occurred at a rate of 28.8%, though less than 1% of the patients died and none had a fistula or small bowel obstruction as a result of the mesh. An analysis of patients that did not receive a biologic, lightweight or C-QUR mesh revealed a recurrence rate of 1.8%. The risk of recurrence was increased in patients who were morbidly obese, received biologic or lightweight mesh and those whose operations were complicated by an enterotomy.
By Asya Ofshteyn and Allen Ho
More from this author: Surgeons may be unaware of own level of burnout, Home Calculator may predict likelihood of home discharge after surgery, Apgar score for surgery predicts mortality in veterans, Frey procedure may yield better outcomes in chronic pancreatitis, Radial artery harvest comparable to saphenous vein harvest for cardiac bypass
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.