Robotic-assisted colectomy may provide minimal benefit compared to laparoscopic
Image: PD
1. Robot-assisted colectomies had equivalent clinical outcomes compared to laparoscopic approach, but had higher overall higher overall hospitalization costs
Evidence Rating Level: 3 (Average)
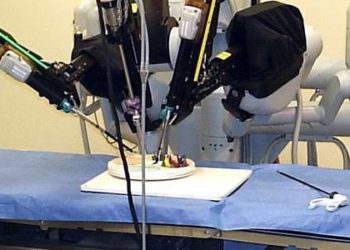
Study Rundown: The use of robotic surgery may address the technical challenges associated with laparoscopic surgery such as the loss of stereoscopic vision. To date, only single-institution, early outcomes studies have been performed for robotic-assisted colorectal surgeries. A retrospective review of a large, multi-centered US surgical outcomes database was conducted to compare the perioperative outcomes and costs of robotic-assisted (RC), laparoscopic (LC), and open colectomies in a large, multi-centered patient database.
The results of this study demonstrate no significant difference in the primary outcome of in-hospital mortality between RC and LC. Additionally, there was no significant difference in secondary outcomes such as overall complication rate, and routine discharge rate. Cost estimate analysis showed greater overall and per day hospitalization costs associated with RC. The strength of this study includes the use of the US-wide, multi-centered population database. However, the database only included a small sample size of RC may attribute to the lack of statistical significance. The study shows that there is currently no additional benefit of robot-assisted colorectal surgery compared to laparoscopic approach.
Click to read the study in JAMA Surgery
Click to read an accompanying editorial in JAMA Surgery
Relevant Reading: Economic evaluation of da Vinci-assisted robotic surgery: a systematic review
In-Depth [retrospective cohort]: This study reviewed perioperative colectomy outcomes using the US Healthcare Cost and Utilization Project Nationwide Inpatient Sample (NIS) from 2008-2010. During this time period, LC accounted for 47.6% of all colectomies and RC accounted for 0.6%. A propensity score method was used to compare the outcomes from 1500 LCs and 1584 RCs. There was no significant difference in in-hospital mortality (RC:0.0% LC:0.7%, p=0.12), complications (RC:14.7%, LC:18.5%, p=0.26), or rate of routine discharge (RC: 88.7%, LC:88.5%, p=0.98). Trends that favor RC were observed in median length of hospital stay and rate of conversion to open colectomy. Estimated overall costs were higher in for RC compared to LC (RC: $14,847, LC: $11,966, p<0.001), as well as adjusted for length of stay (RC: $3407, LC: $2617, p<0.001).
By David Wang and Andrew Bishara
More from this author: “Hospital Report Cards” not associated with improved trauma mortality outcomes, Preoperative vitamin D levels may influence post-surgical infection rate, HIV-infected infant potentially cured with antiretroviral therapy, High prevalence of head impact observed in senior falls, Pediatric appendicitis outcomes in Canada not superior to US
©2012-2013 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.