Salvage esophagectomy may improve survival in patients with esophageal cancer
1. Extent of resection and preoperative tumor depth were significant predictors of improved 3- and 5-year survival in patients who received salvage esophagectomy for recurrent or residual disease following definitive chemotherapy.
2. Resection with negative margins (R0) was associated with earlier stage of cancer (T1/2) at diagnosis and initial complete response with definitive chemotherapy.
Evidence Rating Level: 2 (Good)
Study Rundown: Salvage esophagectomy is offered to patients with residual or recurrent esophageal cancer after definitive chemotherapy (dCRT). Although salvage esophagectomy is a high-risk surgery associated with high rates of morbidity and mortality, several studies have reported that a subpopulation of patients may have improved outcomes with the surgery. This study sought to identify prognostic factors for patients undergoing salvage esophagectomy after failed definitive chemotherapy. The authors found no in-hospital mortality among patients with early stage disease (cT1/2 without nodal involvement) and those who achieved complete response to dCRT. Additionally, they reported that resection with negative margins (R0) and early tumor stage (T1/T2) after dCRT were significant independent predictors for improved survival among salvage esophagectomy patients. R0 resection was associated with tumor depth prior to surgery, tumor depth before dCRT, dCRT response and resectability before dCRT. Major strengths of this study were the large cohort of patients it examined over a span of 25 years, and multivariate analysis of cancer stage and dCRT response on patient survival. However, the study is limited by its retrospective nature, the lack of control for co-morbidities and the lack of comparison groups.
Click to read the study in the Annals of Surgical Oncology
Relevant Reading: Salvage Esophagectomy in the Management of Recurrent or Persistent Esophageal Carcinoma
In-Depth [retrospective cohort]: A total of 63 patients who underwent salvage esophagectomy between April 1988 and December 2013 were included in the study. All surgeries were performed at the Cancer Institute Hospital in Tokyo, Japan. Demographic information, clinicopathologic features and response to chemotherapy were collected for all patients. Outcome measures included postoperative hospital stays, complications, mortality, and overall survival from the date of esophagectomy to the date of death or to the last known follow-up date. Kaplan-Meier survival analysis was performed. Univariate logistic regression was used to identify predictors for R0 resection. There was no in-hospital mortality among 20 patients with cT1-2 tumors, 24 without nodal involvement prior to dCRT or 20 patients who achieved complete response to dCRT. However, there was no statistical difference in clinicopathologic features between the groups, stratified according to the presence or absence of in-hospital mortality. The 3- and 5-year overall survival of the entire cohort was 29.8% and 15.0%, respectively. R0 resection (HR 0.27; 95%CI 0.115-0.614) and preoperative tumor depth (ypT1/2; HR: 0.34; 95%CI 0.141-0.792) were significant independent predictors for improved survival. In addition, R0 resection was associated with tumor depth before dCRT, tumor depth after dCRT, dCRT response and resectability before dCRT on univariate analyses. However, none remained significant on the multivariate analysis.
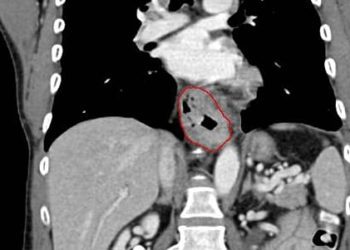
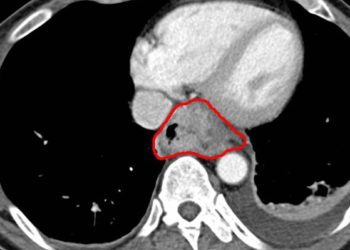
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.