Stool DNA testing may improve screening sensitivity of colorectal cancer
Image: PD
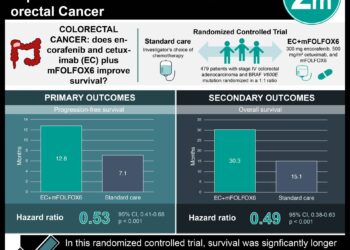
1. A new, non-invasive, multi-target DNA stool test significant increased detection of colorectal cancer in an average-risk cohort compared to fecal immunochemical test (FIT).
2. The DNA stool test also detected significantly more false positive results compared to FIT.
Evidence Rating Level: 2 (Good)
Study Rundown: Despite reducing colorectal cancer (CRC) mortality, a significant proportion of the US population still does not undergo routine CRC screening. The authors of this article analyzed the screening efficacy of a new, non-invasive, multitarget DNA stool test against fecal immunochemical test (FIT) for occult blood in adults with average risk of CRC. Using a cross-sectional design, stool samples from 9989 patients were collected, of which 65 cases of CRC and 757 cases of advanced precancerous lesions were found on colonoscopy. This study demonstrates the potential benefits of utilizing this new DNA stool screening test for CRC; however, there was approximately a 10% false-positive rate for the DNA stool test, which may reduce its utility. The strength of the study is the large population size and the large effect size in comparison to FIT testing. However, in addition to the lower specificity, the higher technical failure rate of sample collection associated with DNA stool test may reduce real-world effectiveness.
Click to read the study in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Screening for Colorectal Cancer: U.S. Preventive Services Task Force Recommendation Statement
In-Depth [cross-sectional study]: This study evaluated 11,016 participants with average risk of CRC. Of those, 689 patients were excluded because of inadequate stool sample of DNA testing, 34 were excluded for inadequate sample for FIT, and 304 were excluded for not completing colonoscopies. Screening sensitivity was significantly higher in DNA testing compared to FIT for both CRC (92.3% vs. 73.8%, p=0.002) and advanced precancerous lesions (69.2% vs. 46.2%, p=0.004). Specificity with DNA testing was significantly decreased compared to FIT (86.6% vs. 94.9%, p<0.001).
More from this author: Radical prostatectomy may trump radiotherapy in non-metastatic prostate cancer, Screening mammography may not decrease overall mortality in women ages 40-59, First report of acute MERS-CoV infection associated with adverse pregnancy outcome, “Hospital Report Cards” not associated with improved trauma mortality outcomes, Preoperative vitamin D levels may influence post-surgical infection rate
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.

![2MM: AI Roundup- AI Cancer Test, Smarter Hospitals, Faster Drug Discovery, and Mental Health Tech [May 2nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/Untitled-design-350x250.png)