Targeted therapy improves progression free survival in lung cancer
1. Among patients with non-small-cell lung cancer (NSCLC) and ALK gene rearrangements, treatment with oral crizotinib therapy was superior to standard intravenous chemotherapy in terms of progression-free survival and objective response rate, but not overall mortality.
2. Crizotinib was associated with side effects including vision disorders, diarrhea, and edema, but was also associated with a significantly greater improvement in global quality of life compared to chemotherapy treatment.
Evidence Rating Level: 1 (Excellent)
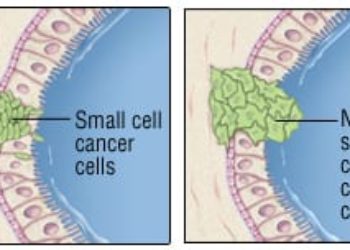
Study Rundown: Rearrangement of the anaplastic lymphoma kinase (ALK) gene has been noted in 3 to 5% of diagnosed cases of non-small-cell lung cancers (NSCLC), a malignancy with adenocarcinoma histology that generally occurs in younger patients who have not smoked. Previous studies showed the efficacy of crizotinib, an oral small-molecule tyrosine inhibitor of ALK, in patients with advanced ALK-positive NSCLC who had previously received platinum-based chemotherapy, but its efficacy and safety profile as first-line therapy for patients with advanced ALK-positive NSCLC is not known.
In this drug-company sponsored study, 343 patients with advanced ALK-positive NSCLC were randomized in a 1:1 ratio to receive either oral crizotinib or six cycles of intravenous pemetrexed-plus-platinum chemotherapy. There was a significantly longer progression-free survival and a higher objective response rate in the crizotinib group compared to the chemotherapy group; however, no difference in overall survival was noted, which was attributed to the relatively low reported deaths in either group (26%) and the fact that 70% of the patients in the chemotherapy group crossed over to the crizotinib group after experiencing disease progression. There were significant side effects in both treatment groups, with vision disorders, diarrhea, and edema occurring more commonly in the crizotinib group. Still, patients receiving crizotinib reported a significantly greater improvement in global quality of life.
This study helps to establish the efficacy of crizotinib as a first-line therapy for a subset of patients with NSCLC who harbor ALK gene rearrangements, also providing a proof of concept for targeted therapy. However, it is important to note the significant side effect profile in those receiving crizotinib and the fact that not all patients responded to this therapy despite its targeted nature.
Click to read the study, published today in NEJM
Click to read an accompanying editorial in NEJM
Relevant Reading: Treating ALK-positive lung cancer–early successes and future challenges
Study Author, Dr. Benjamin Solomon MBBS, PhD, FRACP, talks to 2 Minute Medicine: Associate Professor of Medicine, University of Melbourne, Medical Oncologist, Department of Medical Oncology:
“The findings of our study confirm the importance of molecular testing for ALK gene rearrangements, along with EGFR mutation, in patients with newly diagnosed NSCLC. This international phase III study establishes crizotinib as standard-of-care in previously untreated patients whose tumors test positive for ALK gene rearrangements.”
In-Depth [randomized controlled trial]: This open-label, international randomized controlled study compared the use of crizotinib and standard pemetrexed-plus-platinum chemotherapy in patients with previously untreated advanced ALK-positive non-small-cell lung cancer. Patients were eligible for enrolment if they had histologically or cytologically confirmed advanced NSCLC and had not previously received systemic treatment. In total, 343 patients were randomized to receive oral crizotinib or six cycles of intravenous pemetrexed-plus-platinum chemotherapy. The primary outcome measure was progression-free survival. Patients in the chemotherapy arm were able to crossover to crizotinib treatment if they experienced disease progression.
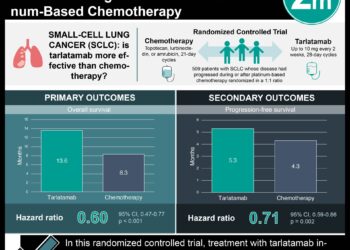
At the time of publication, the median duration of follow-up for overall survival was 17.4 months versus 16.7 months in the crizotinib and chemotherapy groups, respectively. The median progression-free survival was 10.9 months for those receiving crizotinib compared with 7.0 months for those receiving chemotherapy (hazard ratio for progression or death, 0.45; 95% CI, 0.35 to 0.60, P<0.001). The objective response rate was significantly higher in the crizotinib group (74% vs. 45%, P<0.001). There was no significant difference in overall survival between groups (HR for death, 0.82; 95% CI, 0.54 to 1.26, P=0.36).
Both treatment groups experienced significant side effects. Incidence of vision disorders (including visual impairment, photopsia, blurred vision, vitreous floaters, reduced visual acuity, diplopia, and photophobia), diarrhea, and edema was at least 5% higher in the crizotinib group compared to the chemotherapy group. Further, 14% of the patients in the crizotinib group experienced Grade 3 or 4 elevations of aminotransferase levels compared to 2% in the chemotherapy group. One case of fatal pneumonitis was attributed to treatment with crizotinib.
More from this author: Long-acting, reversible contraceptive methods linked to lower teen pregnancy rates, Extraordinary response, and resistance, to everolimus in thyroid cancer pinned to mutations, Triple-combo chemotherapy improves survival for metastatic colon cancer [TRIBE study], Double-unit cord-blood transplantation does not aid survival in children with hematologic malignancy, Early tube feeding unable to reduce infections in pancreatitis [PYTHON trial]
Image: PD
©2014 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. No article should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2 Minute Medicine, Inc.