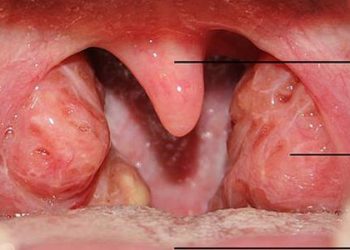
Tonsillectomy may have short-term benefits in recurrent throat infection
1. This meta-analysis reviewed studies comparing tonsillectomy to watchful waiting and found an improvement in throat infections, healthcare utilization, and school absences within the first year after surgery. Longer-term outcomes were limited.
2. Strength of evidence (SOE) was moderate for short-term reduction in throat infections and low for healthcare utilization and school absences in the short term. In the longer term, SOE was low for no difference in missed school and quality of life.
Study Rundown: Tonsillectomy in US children is used to reduce frequency of tonsillitis and limit obstructive sleep apnea symptoms. Previous meta-analyses have included studies of both adults and children, concluding that there were fewer sore throats in the first year after surgery, with greater benefit among those who had more severe infections prior to tonsillectomy. This analysis included all comparative studies of children reviewing the benefits of tonsillectomy versus watchful waiting in reduction of throat infections. Conclusions were then categorized based on SOE. This analysis found that overall, children who received tonsillectomy had greater reduction in throat infections, related healthcare utilization, and fewer missed school and work days in the first year after surgery. No conclusions could be made regarding longer-term benefits, nor could quality of life be evaluated in the short or long term. The SOE for most conclusions was low, but moderate for short term reduction in number of infections. While this study aggregates the most recent data available on tonsillectomy, it is limited by the lack of standardized definitions for tonsillitis and standardized throat infection severity rating. Clinicians should consider the relative dearth of evidence supporting the long-term benefit of tonsillectomy in children.
Click to read the study, published today in Pediatrics
Relevant Reading: Does tonsillectomy lead to improved outcomes over and above the effect of time? A longitudinal study
In-Depth [meta-analysis]: This analysis included 7 English-language published studies from January 1980 through June 2016, comparing throat infection rates of children who received tonsillectomy to those in a watchful waiting cohort. Inclusion criteria included comparative study designs published in English and excluded studies with high risk of bias. Assessment of SOE was done independently, based on consideration of study limitations, consistency in direction of effect, directness in measuring outcomes, precision of effect, and reporting bias. In all studies that included baseline data, the number of infections decreased in both watchful waiting and surgery groups, though moreso in surgery groups. One study showed that children with surgery has 0.50 +/- 0.43 annual sore throats compared to 0.64 +/- 0.49 in the non-surgical group. In another study, the tonsillectomy group has 1.74 episodes compared to 2.93 in the control, a statistically significant but likely clinically insignificant difference. In a retrospective cohort study, reduction in doctor’s visits decreased over time after tonsillectomy, with 2.46 fewer visits in years 1 through 3, and 1.21 fewer visits in years 4 to 6 after tonsillectomy. Quality of life was not markedly different between the 2 groups in any studies reporting this metric. For conclusions related to short-term benefits, SOE was low. Not enough evidence was available for conclusions regarding longer-term effects.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.