Patient and provider interventions no better than usual care for osteoarthritis
1. No statistically significant improvement associated with combined patient and provider intervention in osteoarthritis patients compared to usual care.
2. Physical function and depressive symptoms were similar amongst both intervention and control patient groups.
Evidence Rating Level: 1 (Excellent)
Study Rundown: Osteoarthritis is a leading chronic health conditions in primary care settings. As it is a significant cause of pain and disability, effective treatment is highly important in order to ensure good quality of life for osteoarthritis patients. A previous, single-site study suggested that combined patient and provider intervention improved outcomes for patients with knee osteoarthritis. Based on these findings, the authors of this randomized control trial aimed to assess whether patient-based, provider-based, and patient-provider interventions improve osteoarthritis outcomes. In general, no significant association was found between any of the patient/provider interventions and improved osteoarthritis outcomes. This study has several limitations. Mainly, the study involved only one healthcare network. Additionally, while the authors attempted to match provider intervention and provider control sites based on clinical characteristics, some differences in baseline Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) scores existed between the intervention and control groups. Overall, the results of this study contrast prior findings, suggesting that patient and provider interventions for osteoarthritis may not serve as a more effective treatment method.
Click to read the study, published today in the Annals of Internal Medicine
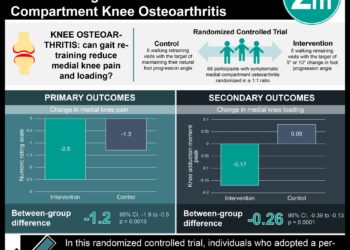
In-Depth [randomized controlled trial]: 537 patients were included in this cluster randomized trial. The study was conducted within the Duke Primary Care Research Consortium, and the intervention took place over 12 months, focusing on physical activity, weight management and cognitive behavioural strategies for managing pain. Greater improvement in mean WOMAC scores between baseline and 12 months did not differ between those in patient or provider interventions (estimated difference -1.6, 95%CI -6.6 to 3.3, p = 0.52). Furthermore, improvement was not observed in any of the intervention groups compared with usual care. Additionally, with respect to WOMAC pain and physical function sub-scales, patients in the patient-provider intervention group did not have greater improvement than in the patient or provider intervention groups (-0.1, CI -1.5 to 1.2, p = 0.83; and -1.5, CI -5.1 to 2.1, p = 0.41, respectively). Again, no difference was observed between any intervention group and usual care.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.