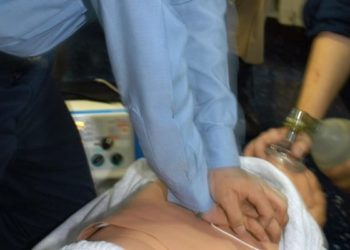
Variability in out-of-hospital pediatric cardiac arrest outcomes
1. Out-of-hospital cardiac arrest (OH-CA) is associated with below-average neurobehavioral outcomes with large variability in the severity of deficiencies
2. Older children suffering OH-CA appear to have worse neurobehavioral outcomes than younger children
Evidence Rating Level: 1 (Excellent)
Study Rundown: Out-of-hospital cardiac arrest is a rare event in children and little data exists regarding the subsequent neurological and developmental outcomes. This study examined 12-month neurobehavioral outcomes in children enrolled in a therapeutic hypothermia trial for out-of-hospital cardiac arrest. The majority of children did not survive OH-CA. Most survivors had below-average cognitive, communication, social, and motor skills one year after cardiac arrest. There was wide variability in the severity of deficiencies, with some children suffering profound impairment, while half functioned generally within normal limits. Children suffering cardiac arrest at an older age appeared to have worse outcomes when compared to younger children, although it may be harder to assess cognition in younger children. Given the rarity of OH-CA, this study examined a fairly large population with excellent follow up using both subjective and objective measures of neurobehavior. Although these results do not allow physicians to predict specific outcomes based on characteristics of patients or the arrest event, they do provide a description of the wide range of neurobehavioral outcomes after OH-CA.
Click to read the study, published today in Pediatrics
Relevant Reading: Therapeutic hypothermia after out-of-hospital cardiac arrest in children.
In-Depth [randomized trial]: This study was a secondary analysis of data from the Therapeutic Hypothermia for Pediatric Cardiac Arrest, Out-of-Hospital (THAPCA-OH) study, a randomized trial evaluating hypothermia versus normothermia for OH-CA in 295 children aged 2 days to 18 years. Family functioning, global functioning, and neurobevahioral outcomes were assessed using both subjective surveys from family members and objective batteries. The former included the Vineland Adaptive Behavior Scales, second edition (VABS-II), a subjective caregiver assessment of neurobehavior, while the latter included the Mullen Scale Early Learning Composite and the Wechsler Abbreviated Scale of Intelligence (WASI), objective assessments of cognition. Of the 96 confirmed survivors, 87 had a pre-arrest subjective neurobehavioral score within in the normal range; 2 of these were lost to follow up. There was significant decline in mean VABS-II scores for neurobehavior between baseline and 12 months, with no difference between normothermia and hypothermia groups. Children older than 6 years had a greater decrease in mean VABS-II scores than younger children. For children <6 years old, 81% had Mullen cognitive scores of either below average or well below average, with 18% scoring the lowest possible score. For children ≥6 years old, 14 (42%) were unable to communicate and therefore ineligible for cognitive testing with the WASI. Of the remaining 19, 48% scored below or well below average on the WASI.
Image: PD
©2016 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.