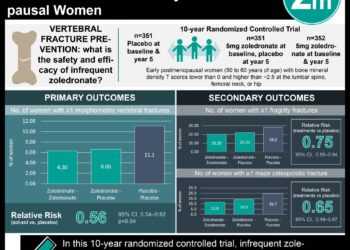
#VisualAbstract: Bone mineral density testing beneficial for older men receiving androgen deprivation therapy for localized or regional prostate cancer
1. Bone mineral density testing was associated with a significant decreased risk of developing major osteoporotic fractures among older men with localized or regional prostate cancer on androgen deprivation therapy.
2. Bone mineral density screening rates remained low in this patient population and was associated with racial, socioeconomic, and geographic disparities.
Evidence Rating Level: 2 (Good)
Study Rundown: Androgen deprivation therapy (ADT) is the mainstay treatment for locally advanced or metastatic prostate cancer; however, it can negatively impact bone health, resulting in decreased bone mineral density (BMD) on dual x-ray absorptiometry (DXA) and fractures. Although, DXA screening is recommended in this patient population, their association with fracture prevention is unknown. This US nationwide population-based cohort study used data from the Surveillance, Epidemiology, and End Results (SEER) database and the Texas Cancer Registry (TCR) to assess DXA screening and fracture rates among men ≥66 years with localized or regional prostate cancer who were initiating treatment with ADT. The main outcomes included frequencies of DXA screening and fracture, and overall survival, where association was evaluated using a multivariable Cox proportional hazards model with propensity score adjustment. Among 54 953 older men with localized or regional prostate cancer who initiated ADT, DXA screening was associated with a reduction in major fractures. Despite this, the use of DXA screening remained low and was associated with racial, socioeconomic, and geographic disparities. These findings provide further evidence for DXA screening in men with prostate cancer to reduce morbidity and mortality associated with fractures. A limitation of this study was the absence of patients with metastatic disease as most patients had localized or regional disease, limiting the generalizability of the results.
Click to read the study in JAMA Network Open
Click to read an accompanying editorial in JAMA Network Open
In-Depth [retrospective cohort]: This cohort study included 54 953 men (median [range] age, 74 [66-99] years; 4689 [8.5%] Hispanic, 6075 [11.1%] non-Hispanic Black, 41 453 [75.4%] non-Hispanic White, 2736 [5.0%] other ethnicities) diagnosed with prostate cancer between 2005-2015 who initiated treatment with ADT. Data on DXA screening from 12 months prior to 6 months after initial ADT claim was collected from the SEER and TCR Medicare-linked databases. Overall, 4362 men (7.9%) received DXA screening, where the screening rate increased from 6.8% in 2005 to 8.4% in 2015. Screening rates were lower in individuals who were single (OR, 0.89; 95%CI, 0.81-0.97; P = .01), non-Hispanic Black (OR, 0.80; 95%CI, 0.70-0.91; P < .001), from small urban areas (OR, 0.77; 95%CI, 0.66-0.90; P = .001) and areas with lower education levels (OR, 0.75; 95%CI, 0.67-0.83; P < .001), and receiving nonsteroidal androgens (OR, 0.57; 95%CI, 0.39-0.84; P = .004). After initial ADT, 9365 patients (17.5%) developed fractures, where the median time to first fracture was 31 months (IQR, 15-56 months). Among men without previous fractures before ADT, DXA screening was not associated with fracture risk at any site (HR, 0.96; 95%CI, 0.89-1.04; P = .32) but was associated with a decreased risk of major fractures (HR, 0.91; 95%CI, 0.83-1.00; P = .05).
©2022 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![2 Minute Medicine: Pharma Roundup: Price Hikes, Breakthrough Approvals, Legal Showdowns, Biotech Expansion, and Europe’s Pricing Debate [May 12nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/ChatGPT-Image-May-12-2025-at-10_22_23-AM-350x250.png)