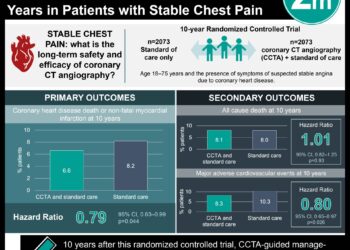
#VisualAbstract: Drug-coated balloons are noninferior to drug-eluting stents for treatment of small vessel coronary artery disease
1. The rate of clinical events and all-cause mortality was similar in patients with drug-coated balloon therapy compared to those with drug-eluting stent therapy.
2. Treatment with drug-coated balloons yielded non-significantly decreased rates of major bleeding and probable or definite stent thrombosis.
Evidence Rating Level: 1 (Excellent)
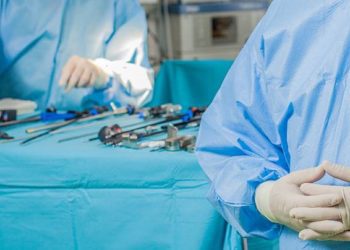
Study Rundown: Drug-coated balloons (DCBs) represent a novel therapeutic option for patients with specific cardiovascular conditions. Compared to drug-eluting stents (DESs), DCBs reduce intravascular foreign material and contain a shorter regimen of dual antiplatelet therapy (DAPT). They also provide the benefit of long-term vascular remodeling associated with paclitaxel. Current evidence shows a sustained effect of DCBs in patients with in-stent-restenosis. However, limited evidence exists surrounding long-term efficacy in patients with small vessel coronary artery disease (SVCAD). This follow-up of an open-label, multicenter, randomized controlled trial aimed to compare the safety of drug-coated balloon therapy versus drug-eluting stent therapy at three years post-randomization for treatment of SVCAD. Primary outcomes for this study included major cardiac events (i.e. cardiac death, non-fatal myocardial infarction, and target-vessel revascularization), all-cause death, major bleeding, and probable or definite stent thrombosis. Study results demonstrated a similar rate of overall and individual major cardiac events, as well as all-cause death, among patients in the DCB and DES groups. In addition, the rate of probable or definite stent thrombosis and major bleeding was lower in the DCB group; however, this was not statistically significant. This randomized controlled trial was limited by a lack of generalizability as the patient population comprised predominantly of European men. In addition, majority of the study findings at the 3-year follow-up lacked statistical significance. Nonetheless, this is the largest randomized controlled trial assessing the safety and efficacy of drug-coated balloons versus drug-eluting stents in patients with small vessel coronary artery disease.
Click to read the study in The Lancet
Relevant Reading: Drug-Coated Balloon Angioplasty Versus Drug-Eluting Stent Implantation in Patients With Coronary Stent Restenosis
In-depth [randomized controlled trial]: Between April 10, 2012, and Feb 1, 2017, 883 patients were assessed from 14 centers in Germany, Switzerland, and Austria. The eligibility criteria included having an indication for percutaneous coronary intervention (PCI), low grade dissection, reduced blood flow, and residual stenosis > 30%. Excluded patients were those with a lesion ≥ 3 mm, in-stent restenosis, life expectancy < 12 months, pregnancy, enrolment in another trial or inability to provide consent. Patients enrolled in the study (n=758, 86%) were randomly assigned to either the DCB group (n=382) or the DES group (n=376), with regular follow-up at 24 and 36 months. The mean patient age was 68 years and one-third of them had cardiovascular risk factors at baseline. Both groups were similar in characteristics, with the exception of fewer male patients in the DES group compared to DCB (70% vs 77%). DAPT duration for stable patients without acute coronary syndrome was 1 and 6 months for the DCB and DES groups, respectively.
Among 382 patients in the DCB group, 349 (91%) completed follow-up at 3-years post-randomization. A similar response rate (92%) was obtained in the DES group (359 out of 376). The rates of major adverse cardiac events (Kaplan-Meier [KM] estimate 15%, hazard ratio [HR] 0.99, 95% confidence interval [CI] 0.68-1.45, p=0.95) and all-cause death (KM estimate 8%, HR 1.05, 95% CI 0.62-1.77, p=0.87) were similar in both groups. The two groups were also similar with regards to individual components of adverse cardiac events: cardiac death (KM estimate 5% vs. 4%, HR 1.29, 95% CI 0.63-2.66, p=0.49), non-fatal myocardial infarction (KM estimate 6%, HR 0.82, 95% CI 0.45-1.51, p=0.52), and target vessel revascularization (KM estimate 9%, HR 0.95, 95% CI 0.58-1.56, p=0.83). Although the rates of probable or definite vessel stent thrombosis (KM estimate 1% vs. 2%, HR 0.33, 95% CI 0.07-1.64, p=0.18) and major bleeding (KM estimate 2% vs. 4%, HR 0.43, 95% CI 0.17-1.13, p=0.088) were lower in the DCB group compared to the DES group, the results were not statistically significant. This was also the case for net clinical benefit in DCB versus DES patients (KM estimate 16% vs. 18%, HR 0.86, 95% CI 0.60-1.24, p=0.43). Overall, findings from this study suggest that DCB is non-inferior to DES at three years post-randomization for treatment of small vessel coronary artery disease, while.
Image: PD
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.

![2 Minute Medicine: Pharma Roundup: Price Hikes, Breakthrough Approvals, Legal Showdowns, Biotech Expansion, and Europe’s Pricing Debate [May 12nd, 2025]](https://www.2minutemedicine.com/wp-content/uploads/2025/05/ChatGPT-Image-May-12-2025-at-10_22_23-AM-350x250.png)