#VisualAbstract: No significant differences in outcomes between pre- and post-treatment administration of P2Y12 inhibitors for NSTE-ACS
1. There does not appear to be any difference in outcome between pre- and post-treatment administration of P2Y12 inhibitors among patients experiencing a non-ST elevation acute coronary syndrome with planned invasive intervention.
2. Prasugrel and ticagrelor showed similar outcomes when administered post-treatment.
Evidence Rating Level: 1 (Excellent)
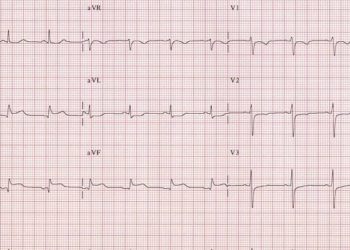
Though it is well established that dual antiplatelet therapy (DAPT) with aspirin and a P2Y12 inhibitor – often prasugrel or ticagrelor – is standard of care in patients experiencing acute coronary syndrome (ACS), the optimal timing of administration is highly contested, especially among patients with non-ST elevation ACS (NSTE-ACS). The administration of prasugrel prior to performing coronary angiography and defining coronary anatomy (i.e. upstream / pre-treatment) may have advantages in theoretically preventing periprocedural thrombotic events, providing more ischemic protection and providing more time for the P2Y12 inhibitor to achieve full anti-platelet effects. However, this is currently not recommended due to an increased risk of bleeding; data for ticagrelor, however, are lacking. This multi-center, randomized trial assessed the efficacy and safety of upstream administration of ticagrelor compared with no pre-treatment and with administration of ticagrelor or prasugrel after defining coronary anatomy (i.e. downstream) among NSTE-ACS patients with planned invasive intervention. 711 patients (median [IQR] age = 64 [57-72] years, 25.3% female) were assigned to an upstream strategy of P2Y12 administration, while 721 patients (median [IQR] age = 65 [56-73] years, 23.6% female) were assigned to a downstream strategy. Among those assigned to the downstream strategy, patients were randomized 1:1 to receive either prasugrel or ticagrelor. The primary endpoint – death at 30 days due to vascular causes, non-fatal myocardial infarction, stroke, and significant bleeding – did not differ between the upstream and downstream groups (3.3% vs. 2.9%, ARR -0.46, 95% CI -2.87 to 1.89). Indeed, the trial was terminated early at the interim analysis in light of a probable futility scenario. Furthermore, when considering the downstream group, the primary endpoint did not differ significantly between patients treated with prasugrel and patients treated with ticagrelor (4.1% vs. 3.1%, ARR 0.9, 95% CI -3 to 5). In all, these findings suggest that both pre-treatment administration of ticagrelor and post-treatment administration of either ticagrelor or prasugrel show similar rates of major ischemic and bleeding events among NSTE-ACS patients with planned invasive intervention. Thus, there is, at this time, little evidence to favor one strategy over the other.
Click to read the study in JACC
©2020 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.