2 Minute Medicine Rewind December 28, 2015
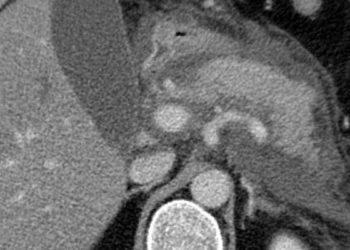
Thoracocentesis and subsequent pleurodesis is an effective method to control dyspnea and chest pain in patients with malignant pleural effusions. However, pain management with NSAIDs is discouraged due to concern that these drugs impair long-term fluid control by suppression of inflammatory responses secondary to pleurodesis agents. Furthermore, there is insufficient data on optimal chest tube size in limiting pain and maximizing pleurodesis efficacy. This study was a 2×2 factorial phase 3 randomized clinical trial involving 320 patients requiring pleurodesis in 16 UK hospitals that investigated these options in patient who underwent chest tube placement for malignant effusions. In patients requiring thoracoscopy, patients received 24F chest tube and were randomized to opiates vs NSAIDs. In patient who did not require thoracoscopy, patients were randomized to 4 groups: 24F chest tube and opiates, 24F tube and NSAIDs, 12F tube and opiates and 12F tube and NSAIDs. Results indicated that pain scores, assessed by the 100-mm visual analog scale (VAS) in the opiate vs NSAID groups were not significantly different (mean VAS score 23.8mm vs 22.1mm; adjusted difference −1.5 mm; 95% CI: −5.0 to 2.0 mm; p = 0.40). Pleurodesis failure occurred in 30 patients (20%) in the opiate group and 33 (23%) in the NSAID group, (Difference, −3%; 95% CI: −10% to ∞; p = .004 for noninferiority). Furthermore, pain scores were lower among patients in the 12F chest tube group vs the 24F group (mean VAS score, 22.0 mm vs 26.8 mm; adjusted difference, −6.0 mm; 95% CI: −11.7 to −0.2 mm; p = 0.04). However, 12F chest tubes were associated with higher pleurodesis failure (30% vs 24%) compared with 24F chest tubes (Difference, −6%; 95% CI: −20% to ∞; p = 0.14 for noninferiority). The main limitation of this study was the lack of blinding among clinicians and patients. However, this study did demonstrate that use of NSAIDs compared with opiates resulted in no significant differences in pain score. Furthermore, NSAID use resulted in non-inferior rates of pleurodesis. Lastly, although 12F tubes were associated with a reduction in pain compared with 24F tubes, they failed to meet the noninferiority criteria for pleurodesis efficacy.
Although anti-thymocyte globulin (ATG) is known to reduce the occurrence of chronic graft versus host disease (GVHD), its role in reducing the need for long term immunosuppression is still unclear. This study was a phase 3, multicenter, open-label, randomized controlled trial at ten transplant centers involving 203 patients with hematologic malignancies. Patients were 1:1 randomized to pre-transplantation ATG plus standard GVHD prophylaxis (n=101) or standard GVHD prophylaxis only (n=102). The primary endpoint was freedom from systemic immunosuppressive drugs without resumption up to 12 months after transplantation. Results showed 37% vs 16% reached the primary endpoint in the ATG vs non-ATG groups (adjusted OR 4.25; 95% CI 1.87 to 9.67; p < 0.001). Adverse event analysis demonstrated EBV reactivation was substantially more common in the ATG vs non-ATG group (20 vs 2 patients). However, no deaths were attributable to ATG. Moreover, the occurrence of serious adverse events was not statistically different between the treatment and control groups. In conclusion, this study demonstrates that ATG should be included in hematopoietic transplantation regimen for patients with hematologic malignancies to reduce long term immunosuppressive burden with care taken to manage EBV re-activation.
Cannabidiol in patients with treatment-resistant epilepsy: an open-label interventional trial
A third of patient with epilepsy have a treatment-resistant epilepsy refractory to two or more antiepileptics. This study was an open-label trial, involving 214 patients (aged 1–30 years) with severe, intractable, childhood-onset, treatment-resistant epilepsy across 11 epilepsy centers. The primary endpoint was the establishment of the safety and tolerability of cannabidiol. The primary efficacy endpoint was median percentage change in the mean monthly frequency of motor seizures at 12 weeks. Patients were given oral cannabidiol at 2-5 mg/kg/day, up titrated to intolerance (capped to a maximum dose based on study site) and evaluated for mean monthly frequency of motor seizures. 162 patients who had at least 12-week follow up were included in the safety and tolerability analysis. 137 patients were included in the efficacy analysis. Analysis indicated that 128 (79%) of patients in the safety group had adverse events, most commonly somnolence, decreased appetite, diarrhea, fatigue and convulsion. 20 (12%) had severe adverse events possibly related to cannabidiol use, most commonly status epilepticus [n=9 (6%)]. The median monthly frequency of motor seizures was 30.0 (interquartile range 11.0 to 96.0) at baseline and 15.8 (5.6 to 57.6) over the 12 week treatment period. The median reduction in monthly motor seizures was 36.5% (IQR 0 to 64.7). Although this study had several limitations, namely the lack of a control group, preliminary analysis does show an adequate safety profile. In conclusion, this study demonstrates the safety of cannabidiol therapy in the management of treatment-resistant epilepsy in children and young adults.
Secukinumab, an Interleukin-17A Inhibitor, in Ankylosing Spondylitis
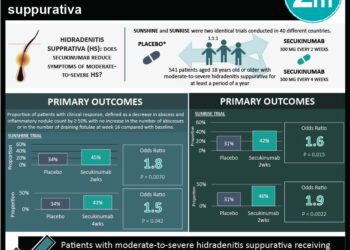
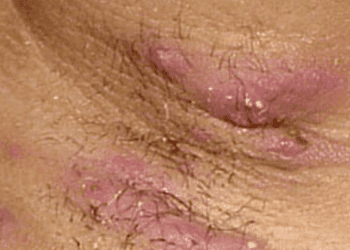
Recent evidence has identified the interleukin-17 pathway as a potential therapeutic target in spondyloarthritis. Preliminary phase 2 trials involving secukinumab, an anti-interleukin-17A monoclonal antibody, have shown promise in symptomatic management. This study is a randomized, double-blind, placebo-controlled phase 3 trial, over 106 multinational centers. The study is separated into 2 segments, MEASURE1 (n=371), a 2-year study followed by a 3-year extension study, and MEASURE2 (n=219), a 5-year study. The primary end point was the proportion of patients with at least 20% improvement in Assessment of Spondyloarthritis International Society (ASAS20) response criteria at 16 weeks. Patients were randomized to receive secukinumab versus placebo in both segments. In MEASURE 1, the ASAS20 response rates at week 16 were 61%, 60%, and 29% for subcutaneous secukinumab at doses of 150 mg, 75 mg and placebo, respectively (p<0.001 compared to placebo). In MEASURE 2, the rates were 61%, 41%, and 28% for subcutaneous secukinumab at doses of 150 mg, 75 mg and placebo, respectively (p<0.001 for the 150-mg dose and p=0.10 for the 75-mg dose). The improvements were sustained at 52 weeks. There was, however, increased risk of infections, primarily candidiasis, in the treatment groups compared with placebo. Furthermore, incidence rates were 0.7, 0.9, and 0.7 cases per 100 patient-years of grade 3 or 4 neutropenia, candidal infections and Crohn’s disease respectively. In conclusion, this study demonstrated that secukinumab provided significant reduction in symptoms of ankylosing spondylitis at 16 weeks.
Warning Symptoms Are Associated With Survival From Sudden Cardiac Arrest
Survival after sudden cardiac arrest (SCA) remains low and strategies to preemptively risk stratify patients at high risk of SCA is needed. This study was a large, prospective community-based study in which warning symptoms were evaluated in the 4 weeks before SCA in 839 patients between 35-65 years of age. Results showed that 430 patients (51%) had warning symptoms, mainly chest pain and dyspnea, in the 4 weeks prior to SCA (50% of men vs. 53% of women; p = 0.59). Most importantly, in most symptomatic patients (93%), symptoms recurred within the 24 hours preceding SCA, yet only 81 patients (19%) called emergency medical services to report symptoms. Survival to hospital discharge when emergency medical services was called was 32.1% (95% CI: 21.8% to 42.4%) versus 6.0% (CI: 3.5% to 8.5%) in those who did not call (p < 0.001). Although these initial results are promising, there were a number of limitations to this study. The most prominent issue was significant recall and response bias. Furthermore, symptom assessment was unavailable in almost a quarter of the patients. In conclusion, this study showed that warning symptoms of SCA are often ignored but when addressed early on lead to significant increased rates of survival.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.