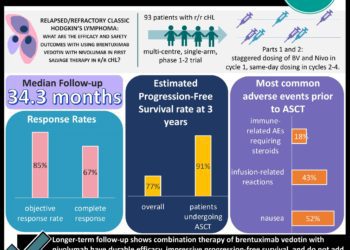
Hodgkin’s Lymphoma survivors at risk for secondary malignancy 40 years post treatment
1. The risk of a second solid cancer following treatment for Hodgkin’s Lymphoma (HL) did not change significantly between those treated during the 1990s (study period of 1989-2000) compared to those treated in earlier decades.
2. HL survivors remain at increased risk of second cancer even after 40 years post treatment.
Evidence Rating Level: 2 (Good)
Study Rundown: While treatment advances for HL has resulted in better survival outcomes, significant trade-offs include increased risk of second solid malignancies and late side effects. This retrospective cohort study was the first to investigate the risk of second solid cancers beyond 25 years of treatment, in the context of changes in radiation and chemotherapy treatments. Across the three study periods spanning 35 years (1965-2000), there was no significant difference in the cumulative incidence of second solid cancers. The strengths of this study include complete and long-term follow up, and detailed treatment data. Given the study period does not include data beyond the year 2000, the effect of newer radiotherapy techniques and dosing since on the risk of second cancers is unknown and thus, represents a limitation for this study. Nevertheless, clinical implications of this study are that HL patients are at increased risk of second cancers 40 years post treatment, and need to be monitored closely during this time. As such, these risks, coupled with treatment toxicity, need to be balanced against the benefits of radiation and chemotherapy.
Click to read the study in NEJM
Relevant Reading: Second malignancy after Hodgkin disease treated with radiation therapy with or without chemotherapy, with long-term risks and risk factors
In-Depth [retrospective cohort]: This retrospective review examined 3905 individuals in the Netherlands having survived treatment for HL (at least 5 years). Treatments spanned from 1965 to 2000 (study periods of 1965-1977, 1978-1988, 1989-2000) with individuals between 15-20 years of age. The second risk of cancer in these individuals was compared against the incident risk of the general population.
A total of 1055 second cancers were diagnosed in 908 patients; a third cancer was diagnosed in 130 patients, and a fourth cancer was diagnosed in 17 patients. The second cancer risk in HL treated patients was higher compared to the general population (standardized incident ratio (SIR), 4.6; 95% [CI], 4.3-4.9). SIRs were significantly higher in the HL cohort for 10 second cancers (except prostate cancer) when compared to the general population. The risk was elevated at 35 years post treatment (SIR, 3.9; 95% [CI] 2.8-5.4), and cumulative incidence in the study cohort at 40 years was 48.5% (95% [CI], 45.4-51.5). Patient receiving supradiaphragmatic radiotherapy not including the axilla had a lower risk of second solid cancers compared to those receiving a mantle-field technique (HR, 0.63; [CI] 95%, 0.49-0.83), largely attributed to the lower risk of breast cancer specifically (HR 0.3; 95% [CI], 0.39-0/84; p=0.002). The cumulative procarbanize dose of 4.3g (or greater, per sq. meter of BSA), was associated with lower breast cancer (HR compared to no chemotherapy, 0.57; 95% [CI] 0.39-0.34) There was no difference in the cumulative second solid cancer incidence across the study periods (p=0.71 for heterogeneity).
Image: CC/Blausen
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.