2 Minute Medicine Rewind June 5, 2017
Delirium is a common postoperative complication in seniors, associated with increased morbidity and mortality. There are a number of contributors to the onset of delirium, including pain and its treatment with opioids. Ketamine, an intravenous anesthetic, reduces postoperative pain and opioid consumption, and despite its hallucinogenic properties, may in fact reduce the incidence of postoperative delirium. In this randomized controlled trial, 672 patients were randomized to receive placebo, low-dose ketamine (0.5 mg/kg) or high-dose ketamine (1.0 mg/kg) after induction of anesthesia, in order to determine whether a subanesthetic dose of ketamine reduces the incidence of postoperative delirium in elderly patients. Researchers found that the incidence of delirium over postoperative days 1-3 was 19.82% in the placebo group, 17.65% in the low-dose ketamine group and 21.30% in the high-dose ketamine group. Based on a logistic regression analysis, there was no significant reduction in postoperative delirium with low-dose (OR 0.90, 95% CI 0.54 to 1.50) or high-dose ketamine (OR 0.97, 95% CI 0.59 to 1.61). Instead, increasing ketamine doses were found to be associated with postoperative hallucinations (p=0.01) and nightmares (p=0.03). The incidence of adverse events did not differ significantly across groups. This study therefore shows that a subanesthetic dose of ketamine does not decrease the incidence of postoperative delirium in older adults, and may in fact cause harm by way of its hallucinogenic effects.
Triple therapy versus biologic therapy for active rheumatoid arthritis
Biologic therapy is recommended for patients with rheumatoid arthritis (RA) who fail to achieve control of their disease by way of conventional disease-modifying anti-rheumatic drugs (DMARDs). Research has shown that the most effective DMARD combination is triple therapy with sulfasalazine, hydroxychloroquine and methotrexate. Studies also indicate that triple therapy is neither inferior to nor less safe than adding a biologic to methotrexate. Despite these findings, triple therapy is rarely initiated, with clinicians opting to administer expensive biologics in patients that have failed to achieve disease control DMARD monotherapy. In this randomized controlled trial, 353 patients with suboptimal responses to methotrexate monotherapy were randomized to receive triple therapy or etanercept-methotrexate. The findings of this trial, the RACAT (Rheumatoid Arthritis Comparison of Active Therapies) trial, confirmed non-inferiority and showed that these patients achieve favourable responses to triple therapy. In this within-trial analysis, the authors compared the cost-effectiveness of these two different approaches to therapy. Researchers found that both strategies led to substantial improvements in health status, without a significant difference in accumulated quality-adjusted life-years (QALYs) between the two groups at 24 and 48 weeks. In addition, the etanercept-methotrexate strategy accumulated substantially higher drug costs at 24 weeks ($11,295 vs. $343 cumulative costs) and 48 weeks ($19,634 vs. $3680) of follow-up. The resultant incremental cost-effectiveness ratio (ICER) for etanercept-methotrexate vs. triple therapy was $2.7 Million (CI $0.87 to infinity) per QALY gained over 24 weeks. However, as 27% of patients in the triple therapy group switched to biologic and vice-versa, the incremental cost and subsequent ICER at 48 weeks decreased to $0.98 million (CI $0.39 to infinity) per QALY. A lifetime analysis further indicated that etanercept-methotrexate would result in an additional 0.15 lifetime QALY, however this would cost an incremental $77,290 or ICER of $521,520 per QALY per patient. This study therefore shows that initiating biologic therapy after failure of DMARD monotherapy without trialing triple therapy increases costs while providing minimal incremental benefit.
There is a need to better understand the health of gender minorities, including individuals who identify as transgender or gender-nonconforming. In response, the Centers for Disease Control and Prevention (CDC) developed a gender identity question module for the Behavioural Risk Factors Surveillance System (BRFSS) for states to administer as of 2014. In this cross-sectional study, the authors analyze the results of 315,893 completed gender identity questionnaires from the 2014 and 2015 BRFSS, which include self-reported outcomes on overall health status, limitations in activities due to physical, mental or emotional problems, and serious difficulty concentrating, remembering or making decisions because of a physical, mental or emotional condition. Researchers found that, compared to cisgender adults whose gender corresponds to their birth sex, gender minority adults were younger (p=0.002), less likely to be non-Hispanic white (p<0.001), married or living with a partner (p=0.01), or be English-speaking (p<0.001). These individuals were also more likely to have lower income (p<0.001), be unemployed (p=0.04), uninsured (p<0.001), overweight (p=0.006), and report depression (p=0.04). With respect to self-reported health measures, gender minority adults were more likely to report poor or fair health (OR 1.30, 95% CI 1.09 to 1.56, p=0.004), difficulty concentrating, remembering, or making decisions (OR 1.56, 95% CI 1.27 to 1.93, p<0.001), and being limited in any way (OR 1.22, 95% CI 1.04 to 1.44, p=0.02). This study therefore shows that significant disparities with regards to socioeconomic status and health exist between cisgender adults and gender minority groups.
Trial of minocycline in a clinically isolated syndrome of multiple sclerosis
The risk of conversion to multiple sclerosis following an initial focal clinical demyelinating event or clinically isolated syndrome is high. Recent studies have indicated that minocycline, a tetracycline antibiotic agent with immune-modulating properties, may reduce the risk of conversion. In this randomized controlled trial, 142 patients were randomized to receive 100 mg minocycline twice daily or matching placebo for up to 24 months to determine whether minocycline reduces the risk of conversion from a first clinical demyelinating event to multiple sclerosis within 6 months after randomization. Researchers found that after adjusting for the number of enhancing lesions at baseline, the difference in the risk of conversion to multiple sclerosis within 6 months of randomization was 18.5% (95% CI 3.7 to 33.3, p=0.01). The unadjusted risk difference was not significant at 24 months of follow-up (p=0.06). Outcomes on the basis of magnetic resonance imaging (MRI) also favoured minocycline over placebo at 6 months, but not at 24 months. However, adverse events of rash, dizziness and dental discoloration occurred more frequently in the intervention group. This study therefore shows that the administration of minocycline in patients that have experience a clinically isolated syndrome may reduce the risk of conversion to multiple sclerosis over 6 months, but not over 24 months.
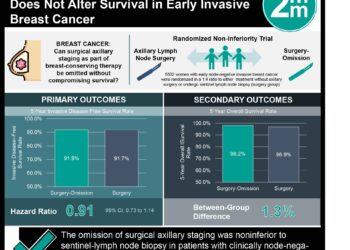
Adjuvant capecitabine for breast cancer after preoperative chemotherapy
Patients with residual invasive breast cancer after receiving neoadjuvant chemotherapy are at a high risk of relapse. While patients with HER2-negative cancer may subsequently receive postoperative radiation therapy, no adjuvant chemotherapy has been established for these patients with residual invasive breast cancer. Capecitabine is an oral prodrug of fluorouracil and has been shown to be efficacious as adjuvant chemotherapy in patients with gastrointestinal cancer. Its role as an adjuvant agent for patients with breast cancer, however, is unclear. In this randomized controlled trial, 910 patients with HER2-negative residual invasive breast cancer after neoadjuvant chemotherapy were randomized to receive standard postsurgical treatment with or without capecitabine in order to evaluate the efficacy and safety of adjuvant capecitabine monotherapy. Researchers found that the rate of disease-free survival was higher in the intervention group at 3 years (82.8% vs. 73.9%) and 5 years (74.1% vs. 67.6%) of follow-up. In other words, the time to recurrence, second cancer or death was longer in the capecitabine group compared to the control group (HR 0.70, 95% CI 0.53 to 0.92, p=0.01). Overall survival was also greater in the capecitabine group (HR 0.59, 95% CI 0.39 to 0.90, p=0.01). Among patients with triple-negative disease, disease-free survival (HR 0.58, 95% CI 0.39 to 0.87) and overall survival (HR 0.52, 95% CI 0.30 to 0.90) rates were also greater in the intervention group. This study therefore shows that after the receipt of standard neoadjuvant chemotherapy, the addition of adjuvant capecitabine therapy may effectively prolong disease-free and overall survival in patients with HER2-negative breast cancer with residual invasive disease.
Image: PD
©2017 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.