2 Minute Medicine Rewind May 3 – May 10, 2015
In this section, we highlight the key high-impact studies, updates, and analyses published in medicine during the past week.
Risk of Substantial Intraocular Bleeding With Novel Oral Anticoagulants
The novel oral anticoagulants (NOAC) are an emerging hot topic in medicine given their cost-effectiveness and monitoring preference compared to the traditional vitamin K antagonist warfarin. One deterrent of their use, however, is their non-reversible nature. The risk of intraocular bleeding associated with the NOACs, a bleeding event that was defined by default as major bleeding in the large randomized controlled studies, has yet to be quantified in the literature. In this study, investigators performed a systematic review and meta-analysis of phase 3 randomized clinical trials (RCTs) comparing NOACs with any other anticoagulant control. The results show that in patients with atrial fibrillation in which NOACs were used for stroke prevention, there was no difference in intraocular bleeding events compared to vitamin K antagonists (RR 0.84; 95% CI 0.59-1.19). In patients with venous thromboembolism there was no increased risk of substantial intraocular bleeding with NOACs compared with sequential treatment with low-molecular weight heparin and warfarin (RR 0.67; 95% CI 0.37-1.20). In patients who underwent orthopedic surgery, the risk of intraocular bleeding was no different between NOACs and low-molecular weight heparin (RR 2.13; 95% CI,0.22-20.50). A review of the literature demonstrates that there is no clinical difference in intraocular bleeding rates when using the NOACs compared to traditional anticoagulants.
Repeat stroke risk is highest during the first few weeks after a transient ischemic attack (TIA) or minor ischemic stroke. The role of antiplatelet therapy for secondary stroke prevention was suggested in The Clopidogrel in High-risk patients with Acute Non-disabling Cerebrovascular Events (CHANCE) trial in which the combined clopidogrel and aspirin decreased the 90-day risk of stroke without increasing bleeding compared to aspirin alone. This data, however, was limited to follow-up up to 90 days. In this study, investigators report the 1-year follow up results of the abovementioned CHANCE trial. The trial was a randomized, double blind, placebo controlled trial that randomly assigned 5170 patients within 24 hours after onset of minor stroke or high-risk TIA to clopidogrel-aspirin therapy or aspirin alone therapy. The primary outcome was a stroke event (either ischemic or hemorrhagic) for the 1-year follow up. The results showed that stroke occurred in 275 (10.6%) patients in the clopidogrel-aspirin group compared to 362 (14%) of patients in the aspirin group (hazard ratio 0.78; 95% CI 0.65-0.93; p = 0.006). In terms of the bleeding risk, moderate to severe hemorrhage occurred in 7 (0.3%) patients in the clopidogrel-aspirin group compared to 9 (0.4%) patients in the aspirin group (p=0.44). These results demonstrate dual antiplatelet therapy post minor ischemic stroke or TIA reduces the risk of subsequent stroke over the duration of 1 year of follow up. The combination of clopidogrel with aspirin did not cause more hemorrhagic events in this patient population than aspirin alone.
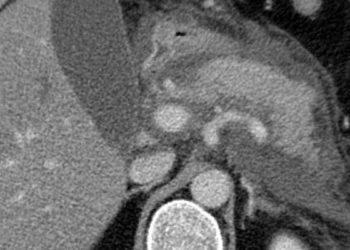
Epilepsy after aneurysmal subarachnoid hemorrhage
Mortality is high following a subarachnoid hemorrhage (SAH) and this is further complicated by the onset of epilepsy. New-onset epilepsy has not been previously studied in large unselected populations. In this population-based study the incidence, risk factors and death from epilepsy were analyzed in 876 patients following a SAH admitted to hospital from 1995 to 2007. Investigators found that epilepsy was diagnosed in 113 patients (13%) in a medium of 8 months after the SAH. Cumulative incidence of epilepsy was 8% at 1 year and 12% at 5 years. The independent risk factors for epilepsy were intracranial hemorrhage, Hunt and Hess grade III-V (grade III = drowsiness, confusion, mild focal neurologic deficit; grade IV= stupor, mod-severe hemiparesis), and acute seizures. Death from epilepsy within the first two weeks after the SAH occurred in 16% of patients. Most importantly, this study demonstrates that the Hunt and Hess grading system for SAH poorly predicted the onset of epilepsy and 12-month mortality. The best predictor of epilepsy was an intracranial hemorrhage. The results may have future implications for treatment of SAH as microsurgical clipping of the aneurysm more often resulted in an intracranial hemorrhage and subsequent epilepsy compared to endovascular occlusive therapy.
The etiology of attention-deficit-hyperactivity disorder (ADHD) is multifactorial, including both a genetic and environmental component and the prognosis of ADHD is very variable and difficult to predict with symptoms in some children improving over time and declining in others. In this prospective study, investigators analyzed 8395 twin pairs from the Twins Early Development Study recruited from population records of births between 1994 and 1996. These twins were followed over time at 8 and 16 years of age to determine the impact of genes and the environment on interindividual differences in the developmental course of ADHD symptom domains of hyperactivity/impulsivity and inattention. Researchers founds that the hyperactive/impulsive symptoms decreased over time (mean score of 6.0 at age 8 years to 2.9 at age 16 years). These results were under strong additive genetic influences (81%; 95% CI 73%-88%). Importantly, more than half of the genetic variation was specific to the developmental course of these children and not shared with their baseline level of hyperactivity/impulsivity. The inattentive symptom decline was less pronounced (mean score of 5.8 at age 8 years to 4.9 at age 16 years). These results were under strong nonadditive genetic influences (54%; 95% CI 8%-76%). More than half of the genetic variation was specific to the development course. This study provides evidence for a sharper decline in the levels of hyperactive/impulsive symptoms compared to inattentive symptoms. These interindividual differences in the developmental course of symptoms were mostly explained by genetic influences and independent from those influencing the baseline level of symptoms. Therefore this proposes that different sets of genes may be associated with the developmental course versus the baseline level of symptoms and may explain why some children remit and others persist. These results are important for clinicians since children who display increased symptoms over time (a decline being normative in the population) might represent a marker of genetic vulnerability and warrant closer follow-up.
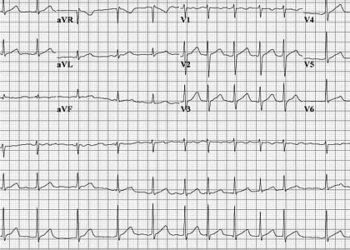
Atrial fibrillation is the most common cardiac arrhythmia, affecting about 46.1 million people globally. It is associated with a 3-5 times increase in risk of stroke. In this retrospective study, researchers investigated the trends in incidence, prevalence and risk factors for atrial fibrillation and its association with stroke and mortality in the 9,511 participants enrolled in the Framingham Heart study from 1958 to 2007. They stratified trends by sexes within 10-year groups. Age-adjusted incidence increased from 3.7 to 13.4 new cases per 1000 person-years in men and from 2.5 to 8.6 new cases per 1000 person-years in women (p<0·0001 for all comparisons). Age adjusted prevalence per 1000 person-years increased however age-adjusted incidence did not change significantly with time. The hazard ratios for atrial fibrillation changed little over time. There was a 74% (05% CI 50-86%) decrease in stroke in 1958-1967 compared to 1998-2007 (HR 3.77, CI 1.98-7.20, p<0.0001) and a 25% decrease in mortality in 1958-1967 compared to 1998-2007 (HR 1.34, CI 0.97-1.86, p<0.003). These results demonstrate that surveillance and awareness of atrial fibrillation in the community over the years has led to more patients treated with anticoagulants reducing their risk of subsequent strokes and has also led to the reported increase in incidence and prevalence. More accurate screening programs in the future will further affect these trends and the detection of this disease.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.




![Weakened grip strength associated with increased morbidity and mortality [PURE study]](https://www.2minutemedicine.com/wp-content/uploads/2015/05/9266_lores1-75x75.jpg)

