2 Minute Medicine Rewind November 9 – 15, 2015
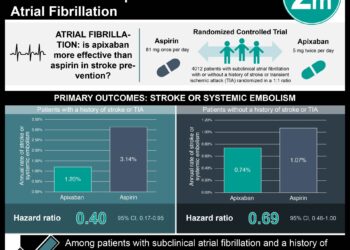
New-onset migraines affect approximately 15% of patients that have undergone transcatheter atrial septal defect (ASD) closure. Following the transcatheter procedure, empirical antithrombotic therapy is indicated, with aspirin over the course of 6 months being commonly prescribed. Recent data, however, has suggested that incidence and severity of migraine headaches following ASD closure can be reduced by adding ticlodipine or clopidogrel to aspirin treatment. In this randomized controlled trial, 171 patients with a clinical indication for transcatheter ASD closure without history of migraines were randomized to receive dual antiplatelet therapy (aspirin and clopidogrel, n = 84) or single antiplatelet therapy (aspirin and placebo, n = 87) to assess the efficacy of clopidogrel for 3 months, used in addition to aspirin, for the prevention of migraine attacks following ASD closure. Researchers found that patients in the clopidogrel group had a reduced mean number of monthly migraine days within the 3-month follow-up period (mean difference -1.02 days, 95% CI -1.94 to -0.10 days; incident risk ratio (IRR) 0.61, 95% CI 0.41 to 0.91) and a lower incidence of migraine attacks post-ASD closure (OR 0.38, 95% CI 0.15 to 0.89). Patients in the intervention group also had less severe migraine attacks according to the MIDAS (migraine disability assessment) questionnaire, where no patients had moderate or severely disabling migraine attacks, compared to 7 patients in the aspirin only group (difference -36.8%, 95% CI -58.5% to -15.2%). There were no between group differences with respect to the incidence of adverse events. This study therefore shows that patients that receive clopidogrel and aspirin, as opposed to aspirin alone, after undergoing transcatheter ASD closure may experience fewer and less severe migraine attacks.
Trial of continuous or interrupted chest compressions during CPR
Standard cardiopulmonary resuscitation (CPR) is comprised of manual chest compressions and positive-pressure ventilation until spontaneous circulation is restored. In the treatment of out-of-hospital cardiac arrest, chest compressions are frequently interrupted by ventilations (rescue breathing). These interruptions decrease blood flow, and may reduce overall effectiveness of CPR. In animal models, the interruption of chest compressions has been associated with decreased survival. In this cluster-randomized trial, 23,711 patients with non-trauma-related cardiac arrest received either continuous chest compressions or interrupted chest compressions, comparing survival, neurologic function and the rate of adverse events between groups. Researchers found that the survival rate was slightly lower in the group that received continuous chest compressions compared to the group that received interrupted chest compressions (9.0% vs. 9.7% survival to discharge, adjusted difference in survival rate -0.7%, 95% CI 1.5% to 0.1%, p = 0.07). Among patients with available data on neurologic status, similar numbers between groups survived with a modified Rankin scale score of 3 or less. There was no significant difference between groups in the rates of individual adverse events. This study therefore shows that in patients with out-of-hospital cardiac arrest, continuous chest compressions during CPR does not result in considerably greater survival rates, favorable neurologic function or decreased rates of adverse events.
A randomized trial of intensive versus standard blood-pressure control
In this randomized controlled trial, 9,361 patients age 50 years and older, with a systolic blood pressure of 130 mmHg or higher and an increased cardiovascular risk without diabetes, were randomized to a systolic blood pressure target of less than 120 mmHg (intensive treatment) or less than 140 mmHg (standard treatment) to determine whether there is a significant benefit in setting a lower systolic blood pressure target with respect to lowering of risks of myocardial infarction (MI), stroke, heart failure or death from cardiovascular causes. Increased cardiovascular risk was defined by having one or more of the following: clinical or subclinical cardiovascular disease, not including stroke, and/or chronic kidney disease, excluding polycystic kidney disease. Researchers found that fewer patients in the intensive group experienced one of the primary outcomes compared to the standard treatment group (HR 0.75, 95% CI 0.64 to 0.89). Mortality was also lower in the intensive-treatment group (HR 0.73, 95% CI 0.60 to 0.90). The numbers needed to treat to prevent a primary outcome event, death from any cause, and death from cardiovascular causes during the median 3.26 years of the trial were 61, 90, and 172, respectively. Serious adverse events, however, were found to occur more often in patients receiving intensive treatment (HR 1.04, p = 0.25). It should be noted that while the rates of serious adverse events overall did not statistically differ between groups, when stratified by type of adverse event, there were statistically significant differences. This includes hypotension (HR 1.67, p = 0.001), syncope (HR 1.33, p=0.05), electrolyte abnormality (HR 1.35, p = 0.02) and acute kidney injury or acute renal failure (HR 1.66, p <0.001). This study therefore shows that among patients with an increased risk of experiencing cardiovascular events, targeting a systolic blood pressure less than 120 mmHg may result in lower rates of fatal and nonfatal major cardiovascular events and death from any cause, as compared to standard therapy. More intensive blood pressure control, however, is associated with significantly higher rates of various adverse events.
Pre-labour rupture of membranes occurs in 20% of all births and 40% of all preterm births, and is associated with increased risk of neonatal infection. Immediate delivery, however, is associated with the risks of prematurity. As such, the best course of management for women with preterm pre-labour rupture of membranes before 37 weeks is unclear. In this randomized controlled trial, 1,839 women with singleton pregnancies and pre-labour rupture of membranes were randomized to undergo immediate delivery or receive expectant management to compare outcomes relating to neonatal sepsis, morbidity and mortality, as well as maternal outcomes. Researchers found that rates of neonatal sepsis were similar between groups (RR 0.8, 95% CI 0.5 to 1.3), and found no significant differences in measures or neonatal morbidity and mortality (RR 1.2, 95% CI 0.9 to 1.6). Neonates born after immediate delivery, however, had significantly lower birth weight, were at an increased risk of experiencing respiratory distress (RR 1.6, 95% CI 1.1 to 2.3), and requiring mechanical ventilation (RR 1.4, 95% CI 1.0 to 1.8). With respect to maternal outcomes, compared to women assigned to the immediate delivery group, those assigned to the expectant management group were at an increased risk of antepartum or intrapartum hemorrhage (RR 0.6, 95% CI 0.4 to 0.9), intrapartum fever (RR 95% CI 0.4, 0.2-0.9), and use of postpartum antibiotics (0.8, 0.7–1.0). Women who delivered immediately, however, were less likely to require caesarean delivery (RR 1.4, 95% CI 1.2 to 1.7). This study therefore shows that, in light of the risks of low birth weight and respiratory distress, as well as poor maternal outcomes, women with pre-labour rupture of membranes should receive expectant management as opposed to immediate delivery, provided there are no overt signs of infection or fetal compromise.
Urine cytology in monitoring recurrence in urothelial carcinoma after radical cystectomy and urinary diversion
Urothelial carcinoma of the bladder is the most common cancer of the urinary tract, and radical cystectomy and urinary diversion (RC-UD) remains the standard treatment for patients with muscle-invasive cancer. After surgery, however, 2-6% of patients will experience recurrence of urothelial carcinoma in the upper urinary tract, and up to 17% in the urethra. Recurrence can be monitored through urinary cytology (UCy). While previous studies have evaluated the performance of UCy in patients that have undergone radical cystectomy, the efficacy of UCy in post-RC-UD surveillance is unclear. UCy is, however, the most commonly used method in detecting recurrence of urothelial recurrence after RC-UD. In this retrospective cohort study, 111 patients were followed up for a mean of 40.8 months to determine the value of UCy in the surveillance of recurrences within remnant urothelium (RRU) in patients that have undergone RC-UD for urothelial carcinoma. Disease recurrence was defined as any documented histologic evidence of urothelial carcinoma in the remnant urothelium after cystectomy. With 111 patients having had 1 or more UCy performed, this yielded 477 UCy samples. Researchers found that positive or suspicious UCy results for 12 of 111 patients, 9 of whom had an RRU. A diagnosis of atypical urothelial cells (AUC) was made for 8.6% of samples, corresponding to 29 patients, of which 21.4% went on to develop RRU. The sensitivity, specificity, positive predictive value, and negative predictive value of UCy for RRU were 82%, 97%, 75%, and 98%, respectively. This study therefore shows that UCy may have good sensitivity and high specificity in detecting RRU after after RC-UD for urothelial carcinoma.
Image: PD
©2015 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.


![Adverse pregnancy outcomes associated with thrombophilias [Classics Series]](https://www.2minutemedicine.com/wp-content/uploads/2015/07/Classics-2-Minute-Medicine-e1436017941513-75x75.png)