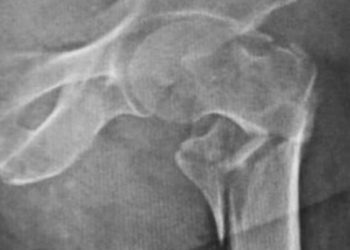
Atopic dermatitis linked with bone and joint injuries
1. Adults with atopic dermatitis (AD) had significantly increased odds of any injury causing limitation when compared to adults without the disease.
2. Patients with AD who concurrently reported fatigue, daytime sleepiness, or insomnia had higher rates of fractures and injury causing limitation than those with disease but without these symptoms.
Evidence Rating Level: 3 (Average)
Study Rundown: AD is a chronic skin disease associated with pruritus, inflammation, increased morbidity and decreased quality of life. A recent study showed that children with AD have increased risk of incurring injuries that require medical care. The elevated risk can be physiologically attributed to disease-associated sleep impairment, use of sedating anti-histamines and use of systemic corticosteroids. In this study, authors aimed to look at the risk of fracture and bone or joint injury (FBJI) in patients with AD to formally establish AD as a risk factor for injury causing limitation. They found that AD was a significant risk factor for injury. A key strength of this study was its large cohort. However, the validity and accuracy were limited by the survey study-design, and because the effect of systemic corticosteroids was not controlled.
Click to read the study in JAMA Dermatology
Relevant Reading: Bone mineral density in children with moderate to severe atopic dermatitis
In-Depth [survey]: Data was sourced from the 2012 National Health Interview Survey, a cohort of 34,500 adults ages 18-85. After controlling for socioeconomic status, asthma, hay fever, food allergies, and other behavioral disorders, adults with AD had an elevated odds ratio of incurring any injury causing limitation with an adjusted odds ratio (aOR) of 1.44 [95% CI, 1.07-1.94]. For FBJI in AD patients in particular the aOR was 1.67 [95% CI, 1.21-2.33]. Other skin problems were not found to be associated with injury. The cohort without AD had gradually increasing prevalence of injuries with increased age as compared to the cohort with AD in which the prevalence of injuries greatly increased initially, peaked at 50-69 years, and subsequently dropped thereafter. Patients who concomitantly had insomnia, daytime sleepiness and fatigue had increased likelihood of FBJI compared to those without sleep symptoms (aOR 1.74 [95% CI, 1.28-2.37]; aOR 1.81 [95% CI, 1.28-2.55]; aOR1.59 [95% CI, 1.16-2.19], respectively).
More from this author: Tech-aided surveillance of patients at high risk for melanoma aids early diagnosis, Indoor tanning linked to high skin cancer risk in US and abroad, Free drug samples may alter prescription habits of dermatologists, Atopic dermatitis may be more persistent than previously understood
Image: PD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.