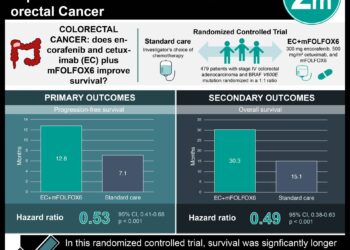
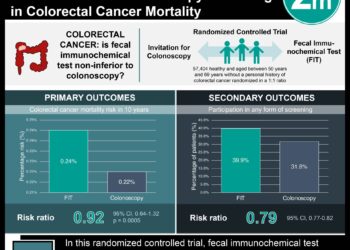
Checkpoint inhibitors show some benefit in patients with microsatellite stable metastatic colorectal cancer without liver metastases
1. In this retrospective cohort study investigating targeted therapy of programmed cell death receptor 1 and programmed cell death ligand 1 in the treatment of microsatellite stable (MSS) metastatic colorectal cancer with and without liver metastases, targeted therapy was found to be effective in patients without liver metastases, but not in patients with liver metastases.
Evidence Rating Level: 2 (Good)
Study Rundown: Microsatellite metastatic colorectal cancers are typically less responsive to targeted immunotherapy than microsatellite instability-high cancers, owing to their relatively low mutation rates and immune cell involvement. The application of various immunotherapies for metastatic colorectal cancer has been recently of interest. The role of programmed cell death receptor 1 (PD-1) and programmed cell death ligand 1 (PDL-1) targeted therapy in the treatment of MSS colorectal cancer is poorly understood, particularly with regards to the location of metastases. Wang et al performed a single center, retrospective cohort study to investigate the efficacy of PD-1/PDL-1 targeted therapy for patients with metastatic colorectal cancer and either with or without liver metastases. 95 patients were included in total with 54 individuals (56.8%) having metastases in their liver. The most common site of metastases were the lungs (66 patients, 69.5%). Patients were treated with the following anti-PD-1/PDL-1 agents: nivolumab, atezolizumab, pembrolizumab or durvalumab. An ORR was observed in 8 patients (8.4%), of which seven had a partial radiographic response and one was complete. Of the non-responders, 17 (17.9%) patients had stable disease after therapy, and 73 (73.7%) continued to experience disease progression. Importantly, none of the patients with liver metastases demonstrated any response to therapy. The median PFS was 4.0 months for patients without liver metastases and 1.5 months for patients with liver metastases. This study demonstrated the ineffectiveness of anti-PD-1/PDL-1 therapy in the treatment of patients with MSS colorectal cancer and liver metastases. These results suggest that further study of anti-PD-1/PDL-1 therapy in this particular subset of patients would be fruitless, and that other treatment options should be explored. The findings of this study support similar investigations of immunotherapy for metastatic cancers at other sites. The effect size reported in this trial is fairly sizable, although the trial itself was small. Additionally, the authors speculate on the mechanism behind variations in response based on metastases location, which reinforces the conceivability of the results. The primary limitations of this study include the small sample size, retrospective design and inclusion of co-interventions. This makes it difficult to interpret the responses to treatment demonstrated by some patients in the trial. Further study of immune therapy for patients with metastatic cancer is warranted.
Click to read the study in JAMA Network Open
Click to read an accompanying editorial in JAMA Network Open
Relevant Reading: Advances in immunotherapy for colorectal cancer: a review
In Depth [retrospective cohort study]: Patient data was collected between January 1, 2014 and December 31, 2020 at a single cancer center in California. Patients receiving concomitant chemotherapy were excluded, but those undergoing radiotherapy or other investigational drug treatments were included. Tumour response was assessed by means of the Response Evaluation Criteria in Solid Tumors (version 1.1). The overall objective response rate was 8.4% (8 of 95 patients, 95% confidence interval 3.7-15.9%). No objective response was seen in the patients with liver metastases. The disease control rate was significantly higher in patients without liver metastases (58.5%) compared to those with liver metastases (1.9%, p<0.001). Similarly, the difference in PFS rates was also statistically significant between those with and without liver metastases. The 6-month PFS rate was 36.6% in patients without liver metastases, versus 1.9% in patients with liver metastases (p<0.001). The PFS was significantly reduced in patients who had liver metastases at the time of treatment initiation, as evidenced by a hazard ratio of 4.98 (95% confidence interval 2.95-8.38) in favour of those without liver metastases. Having an Eastern Cooperative Oncology Group performance status score of 0 was also significantly associated with better response to therapy compared to a score of 1 (objective response rate 16.7% versus 1.9%, p=0.02).
Image: PD
©2021 2 Minute Medicine, Inc. All rights reserved. No works may be reproduced without expressed written consent from 2 Minute Medicine, Inc. Inquire about licensing here. No article should be construed as medical advice and is not intended as such by the authors or by 2 Minute Medicine, Inc.