Fatty liver disease may independently predict high-risk coronary disease
1. Non-alcoholic fatty liver disease (NAFLD) was significantly and independently associated with the presence of one or more high-risk coronary artery plaque features as determined by coronary computed tomography angiography.
2. Among patients with NAFLD, the risk of an acute coronary syndrome (ACS) was nearly 6 times higher than in patients without NAFLD.
Evidence Rating Level: 3 (Satisfactory)
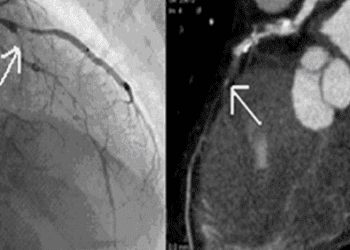
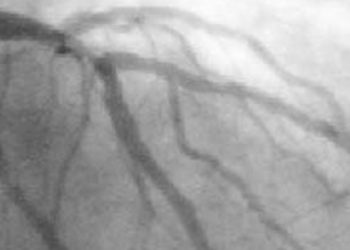
Study Rundown: Non-alcoholic fatty liver disease is a term used to describe a syndrome in which fatty deposits form within the liver and lead to abnormalities in liver function. Untreated, NAFLD can progress to cirrhosis and liver failure, and it is currently the most common cause of liver disease in the United States. The exact cause of NAFLD is not known, but the disease is likely related to inflammation and shares a number of risk factors with coronary artery disease (CAD). Previous research has established NAFLD as an independent risk factor for CAD. In the present study, researchers used coronary computed tomography angiography (CCTA) to study patients with symptoms concerning for reduced blood flow to the heart—or acute coronary syndrome (ACS)—to determine the association between certain high-risk coronary artery plaque features and the presence of NAFLD. Results demonstrated a strong association between high-risk CCTA features and NAFLD, and the presence of NAFLD was shown to predict the existence of these high-risk coronary plaques independent of traditional CAD risk factors. Study patients with NAFLD had a significantly higher risk of being diagnosed with ACS. These results serve to enhance the results from prior trials on the link between NAFLD and CAD, and reinforce the need for formal CAD evaluation in patients with fatty liver.
Click here to read the study in Radiology
Relevant Reading: NAFLD, NASH and liver cancer
In-Depth [retrospective cohort]: Data from this study were obtained from the Rule Out Myocardial Infarction using Computer Assisted Tomography II (ROMICAT II) trial, which enrolled 1000 patients with signs and symptoms concerning for ACS but with normal electrocardiograms and normal cardiac enzymes. A total of 501 patients were randomized to the CCTA arm of the trial, and 452 were included for analysis. This group of patients served as the study population. Using CCTA, the coronary arteries of each patient were evaluated for coronary artery disease plaque burden and morphology by three experienced readers. Note was made as to the presence or absence of several known high-risk plaque features, such as remodeling, low attenuation plaque, the “napkin ring” sign, and spotty calcification. In each patient, the presence of absence of NAFLD was determined using non-contrast computed tomography NCCT obtained alongside CCTA and evaluated by one experienced reader. The resultant data were analyzed using both univariate and multivariate analysis to determine the relationship between variables such as the presence or absence of NAFLD; the presence or absence of high-risk coronary plaque features; coronary artery disease risk factors such as smoking, BMI, and hypertension; and the total extent of coronary artery disease. The presence of NAFLD was strongly positively associated with CAD of all severities (P<0.001). NAFLD independently predicted the presence of high-risk coronary plaque by univariate analysis (OR 3.65; 95% CI: 1.84-7.23; P<0 .001) with a trend toward significance by multivariate analysis. There was also found to be a high study incidence of ACS among patients with NAFLD (15.4% of NAFLD patients versus 3.0% without), for nearly a six-fold risk increase (OR, 5.84; 95% CI: 2.58, 13.22; P<0.001) as compared to non-NAFLD patients.
More from this author: 7 tesla breast MRI may improve assessment of suspicious masses; Breast ultrasound may improve cancer detection in dense breasts; Quantitative MRI may differentiate true from pseudoprogression in glioblastoma
Image: CC/James Heilman, MD
©2012-2014 2minutemedicine.com. All rights reserved. No works may be reproduced without expressed written consent from 2minutemedicine.com. Disclaimer: We present factual information directly from peer reviewed medical journals. No post should be construed as medical advice and is not intended as such by the authors, editors, staff or by 2minutemedicine.com. PLEASE SEE A HEALTHCARE PROVIDER IN YOUR AREA IF YOU SEEK MEDICAL ADVICE OF ANY SORT.